## Management of Severe, Refractory Atopic Dermatitis ### Clinical Context: Severe AD Unresponsive to Conventional Therapy **Key Point:** When moderate-to-potent topical corticosteroids and phototherapy fail, systemic immunosuppressive agents are indicated. The choice depends on efficacy, safety profile, and availability. ### Dupilumab: The Modern Gold Standard **High-Yield:** Dupilumab is a fully human monoclonal antibody against the IL-4 receptor alpha subunit, blocking both IL-4 and IL-13 signaling — the key Th2 cytokines driving AD. #### Why Dupilumab is Preferred in This Case: 1. **Efficacy:** Rapid onset (improvement within 2–4 weeks), sustained remission in >70% of patients with severe AD. 2. **Safety:** No systemic immunosuppression, no hepatotoxicity, no monitoring of renal function or blood counts required. 3. **Mechanism:** Directly targets the pathogenic Th2 pathway, not non-specific immunosuppression. 4. **Elevated IgE:** Dupilumab is particularly effective in IgE-high phenotypes (>2000 IU/mL). 5. **Guideline status:** First-line biologic for moderate-to-severe AD per EAACI, AAD, and Indian Dermatology Society guidelines (2023). ### Comparison of Systemic Agents for Severe AD | Agent | Onset | Efficacy | Monitoring | Adverse Effects | Use | | --- | --- | --- | --- | --- | --- | | **Dupilumab** | 2–4 weeks | 70–80% improvement | Minimal | Conjunctivitis, headache | **First-line biologic** | | Cyclosporine | 4–8 weeks | 60–70% improvement | Renal function, BP, K^+^ | Nephrotoxicity, HTN, infections | Second-line if dupilumab unavailable/contraindicated | | Systemic corticosteroids | Days | Rapid but temporary | HPA axis, glucose | Rebound flares, osteoporosis, infections | **Acute flares only**, not maintenance | | Azathioprine | 8–12 weeks | 50–60% improvement | CBC, LFTs | Hepatotoxicity, myelosuppression | Third-line; rarely used now | ### Why NOT the Other Options? **Systemic Corticosteroids (Option B):** - Provide rapid but temporary control; high risk of **rebound flares** upon withdrawal. - Long-term use causes HPA axis suppression, osteoporosis, metabolic complications. - Not suitable for chronic management of severe AD. - Reserved for acute exacerbations only. **Cyclosporine (Option A):** - Effective but requires close monitoring (renal function, blood pressure, potassium). - Nephrotoxicity and hypertension limit long-term use. - Dupilumab is safer and more effective; cyclosporine is now second-line. **Hematopoietic Stem Cell Transplantation (Option D):** - Experimental; not standard of care for AD. - Reserved for severe immunodeficiency syndromes with AD (e.g., SCID, Omenn syndrome), not primary AD. - Unacceptable risk–benefit ratio for benign skin disease. **Clinical Pearl:** Dupilumab can unmask or worsen pre-existing conjunctivitis in ~15% of patients — counsel on eye care and consider ophthalmology referral if symptomatic. [cite:Harrison 21e Ch 325; EAACI Atopic Dermatitis Guidelines 2023; AAD Guidelines 2023] 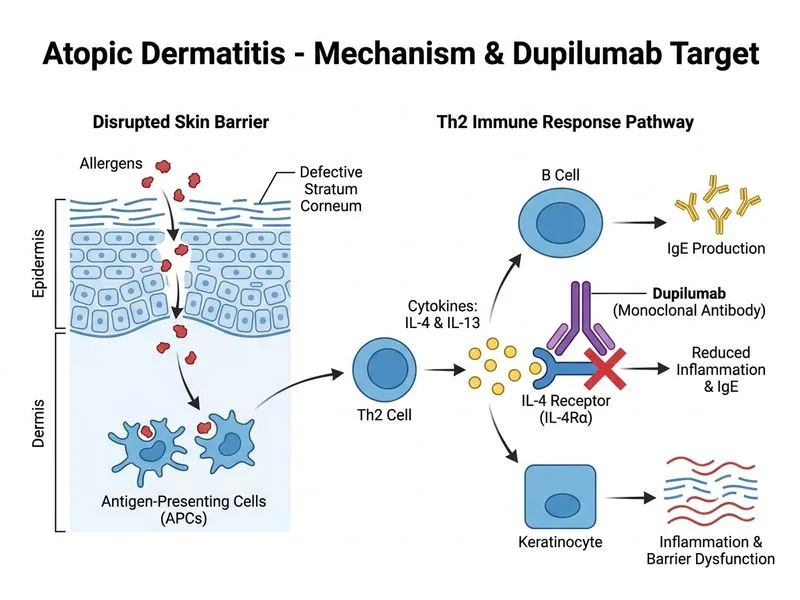
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.