## Clinical Diagnosis The clinical presentation is classic for **basal cell carcinoma (BCC)**: pearly nodule with central ulceration (rodent ulcer), rolled edges, and dermoscopic arborizing vessels on the cheek — a sun-exposed, cosmetically sensitive facial site. ## Why Mohs Micrographic Surgery is the Best Next Step **Key Point:** The cheek is considered a **high-risk anatomical zone** for BCC (along with the nose, eyelids, lips, ears, and temples). For facial BCCs — even those <2 cm — Mohs micrographic surgery (MMS) is the **gold standard** per NCCN and BAD guidelines because: 1. **100% margin assessment** — Mohs examines the entire peripheral and deep margin (vs. ~1% sampled in standard excision), giving the highest cure rate (~99% for primary BCC) 2. **Tissue-sparing** — critical on the face for cosmesis and function 3. **Definitive treatment in a single procedure** — combines excision + histopathology simultaneously 4. **Facial location = high-risk zone** — recurrence on the face carries significant morbidity; MMS minimises this risk **High-Yield:** NCCN guidelines classify BCC on the face (excluding low-risk zones) as **high-risk**, for which MMS is the preferred treatment regardless of size. ## Why Not Other Options? | Option | Reason Not Preferred | |---|---| | **Wide local excision with 5 mm margins under GA** | Unnecessarily aggressive (GA adds morbidity); does not offer 100% margin control; inferior cure rate vs. Mohs on the face | | **Topical imiquimod 5%** | Suitable only for small (<2 cm) **superficial** BCCs; contraindicated for nodular BCC with ulceration; not appropriate for facial high-risk lesions | | **Excisional biopsy with 3 mm margins + histopathology** | A two-step approach (biopsy then re-excision) is suboptimal; 3 mm margins on the face are inadequate for nodular BCC and do not guarantee complete excision; Mohs achieves diagnosis and treatment simultaneously | ## Risk Stratification Summary | Feature | This Patient | Risk Level | |---|---|---| | Location | Cheek (facial H-zone adjacent) | High | | Size | 1.5 cm | Intermediate | | Subtype (clinical) | Nodular with ulceration | Intermediate–High | | Borders | Well-defined | Lower risk | **Clinical Pearl:** Per Harrison's Principles of Internal Medicine and NCCN guidelines, any BCC on the face — particularly with ulceration — warrants Mohs micrographic surgery as the preferred definitive treatment due to the combination of high cure rates, tissue preservation, and real-time margin control. [cite: Harrison's 21e Ch 72; NCCN Guidelines BCC v2.2024; Robbins 10e Ch 25] 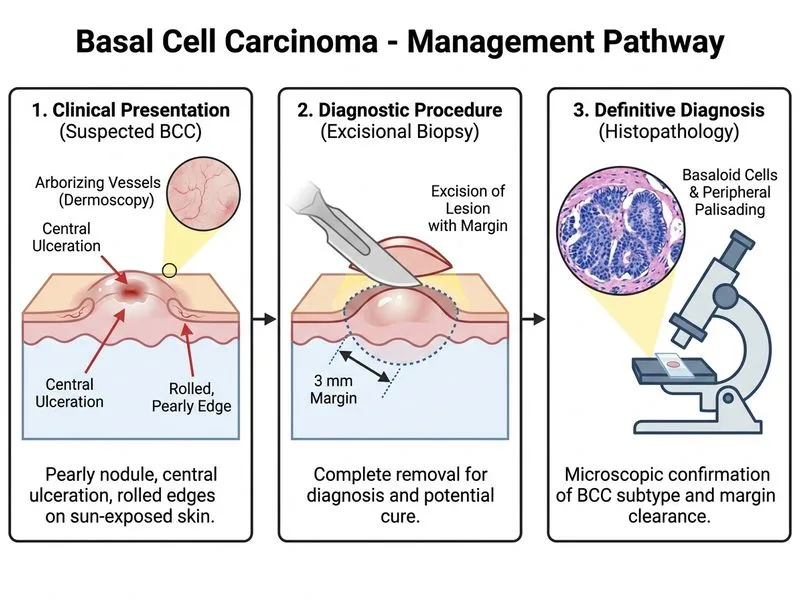
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.