## Clinical Scenario Analysis This patient presents with acute ischaemic stroke (left-sided weakness, facial droop) confirmed on MRI, within the thrombolytic window, with a normal non-contrast CT head (no haemorrhage). The most appropriate **immediate** next step is intravenous alteplase. ## Why IV Alteplase (Option D) is the Correct Answer **Key Point:** Per AHA/ASA 2019 Acute Ischaemic Stroke Guidelines, IV alteplase (0.9 mg/kg, max 90 mg) should be administered **as soon as possible** in eligible patients within 4.5 hours of symptom onset, provided there is no haemorrhage on CT and no absolute contraindications. Time-to-treatment is the single most important determinant of outcome — "time is brain." **High-Yield:** The presence of ICA stenosis (even 85%) is **not** a contraindication to IV thrombolysis. Thrombolysis should not be delayed to obtain additional vascular imaging when the patient is already within the treatment window and the diagnosis of ischaemic stroke is confirmed. Rapid MRI DWI protocols (≤10 minutes) are now available at many stroke centres and do not preclude thrombolytic eligibility — the thrombolytic window is calculated from symptom onset, not from imaging time. ## Why the Other Options Are Incorrect - **Option C (CTA neck + intracranial):** While CTA is valuable for thrombectomy planning, it should **not delay** IV alteplase. Current guidelines recommend initiating alteplase first; CTA can be obtained simultaneously or immediately after. Delaying thrombolytics to obtain CTA wastes the treatment window and worsens outcomes. - **Option A (Urgent carotid endarterectomy):** CEA is contraindicated in the acute stroke phase. It is considered electively after neurological stabilisation (typically 2–6 weeks post-stroke for symptomatic stenosis ≥50–99%). - **Option B (Dual antiplatelet + defer):** Appropriate for TIA or minor non-disabling stroke not eligible for thrombolysis, but not for an acute MCA territory infarct within the thrombolytic window. ## Treatment Algorithm ``` Acute ischaemic stroke confirmed (MRI/CT) ↓ Normal CT head (no haemorrhage) ↓ Within thrombolytic window + no contraindications ↓ → Administer IV alteplase IMMEDIATELY (Option D) ↓ Obtain CTA (can be done simultaneously/post-bolus) ↓ If large vessel occlusion → consider mechanical thrombectomy ``` **Clinical Pearl:** The "drip-and-ship" or "drip-and-stay" model mandates that alteplase is given first. CTA for thrombectomy planning runs in parallel — it does not precede thrombolysis. The door-to-needle time target is ≤60 minutes; any additional imaging that delays this is not the best next step. (Reference: AHA/ASA Guidelines for Early Management of Acute Ischaemic Stroke, *Stroke* 2019; Harrison's Principles of Internal Medicine, 21st ed., Chapter on Cerebrovascular Disease.) 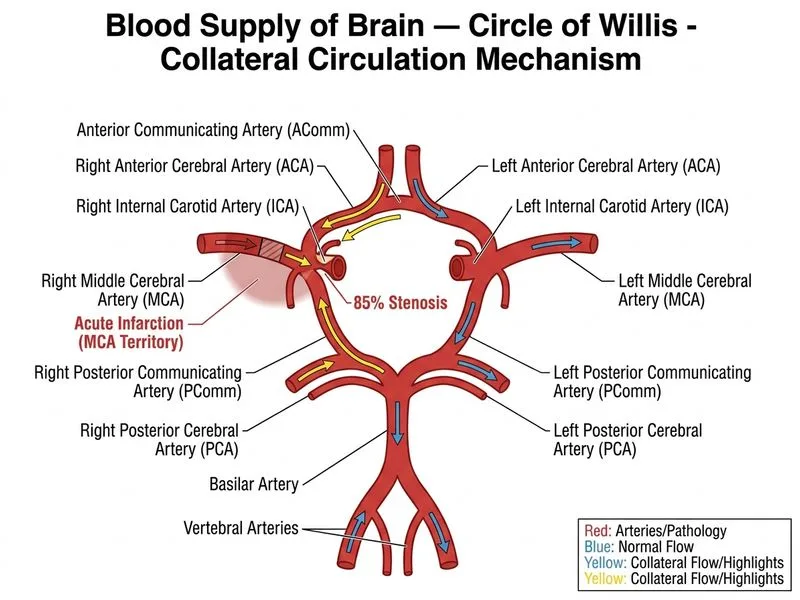
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.