## Investigation for Confirming Diagnosis and Assessing Histological Grade in Aggressive Bone Lesions **Key Point:** Core needle biopsy under imaging guidance is the most specific investigation for **confirming the diagnosis AND assessing histological grade** in suspected malignant bone tumors such as osteosarcoma. Only tissue examination can provide histological grading. ### Why Core Needle Biopsy (Option D) is the Answer The stem explicitly asks for the investigation "most specific for **confirming the diagnosis** and **assessing histological grade**." This requires tissue — MRI alone cannot determine histological grade (low vs. high grade). The gold standard for tissue diagnosis in suspected malignant bone tumors is **image-guided core needle biopsy**, which: - Provides adequate tissue for histopathological diagnosis - Allows assessment of cellularity, pleomorphism, mitotic rate, and necrosis (histological grading) - Is performed under imaging guidance (CT or ultrasound) to target viable, enhancing tumor periphery - Minimizes morbidity compared to excisional biopsy - Does not contaminate surgical planes (unlike excisional biopsy) ### Biopsy Strategy in Bone Tumors (Standard of Care) | Investigation | Role | Limitation | |---|---|---| | **Plain radiographs** | Initial characterization | No tissue diagnosis or grade | | **MRI with contrast** | Local staging, biopsy planning | Cannot assess histological grade | | **Core needle biopsy (imaging-guided)** | Tissue diagnosis + histological grade | Sampling error if wrong site chosen | | **Excisional biopsy** | NOT recommended | Contaminates surgical field | | **FNA (FNAC)** | NOT recommended for bone tumors | Cytology only; inadequate for grading | **Clinical Pearl:** Per standard oncology guidelines (ESMO, NCCN) and surgical oncology texts (Enneking staging system), **image-guided core needle biopsy** is the preferred method for tissue diagnosis in suspected primary malignant bone tumors. MRI is performed *before* biopsy to plan the biopsy approach, but MRI itself does not confirm diagnosis or provide histological grade. **Why Option B (MRI with contrast followed by biopsy planning) is incorrect:** MRI is an essential *prerequisite* step for planning the biopsy, but it does not itself confirm the diagnosis or assess histological grade. The question asks for the investigation that is "most specific for confirming diagnosis AND assessing histological grade" — this is unambiguously the **core needle biopsy**, not MRI. **Why Option A (Excisional biopsy) is wrong:** Excisional biopsy is contraindicated in suspected malignant bone tumors because it violates tissue planes, contaminates the surgical field, and makes definitive limb-salvage surgery more difficult or impossible. **Why Option C (FNA) is wrong:** Fine-needle aspiration cytology provides only cytological material — insufficient for histological grading, assessment of matrix production, or architectural features required to diagnose and grade osteosarcoma. **High-Yield Sequence for Suspected Osteosarcoma:** 1. Plain radiographs → Initial characterization (sunburst, Codman's triangle, cortical destruction) 2. MRI with contrast → Define local extent, identify viable tumor, plan biopsy site 3. **Image-guided core needle biopsy** → Confirm diagnosis + histological grade ✓ 4. CT chest + bone scan → Metastatic staging **Mnemonic: RICE** — Radiograph first, Image (MRI) for planning, Core needle biopsy for Confirmation and grading, Excisional biopsy is contraindicated. [cite: Robbins & Cotran Pathologic Basis of Disease 10e Ch 26; Harrison's Principles of Internal Medicine 21e; Enneking WF, Musculoskeletal Tumor Surgery] 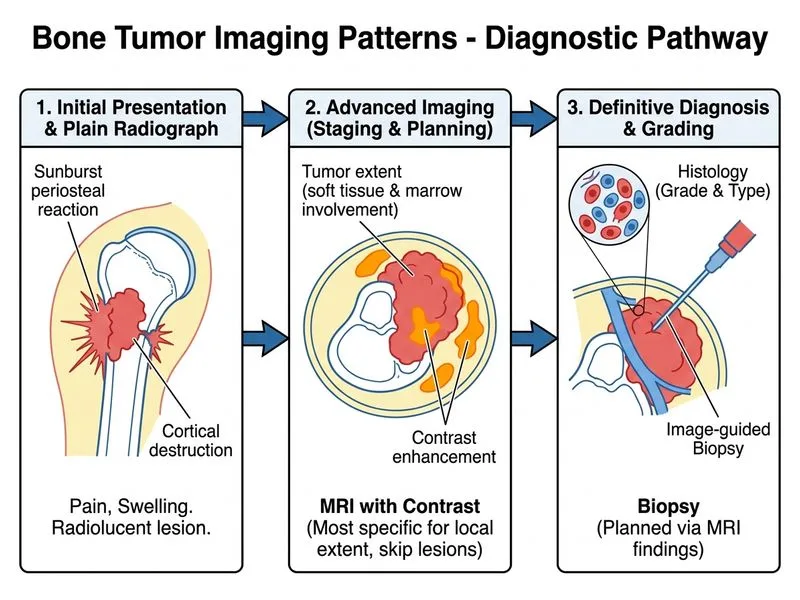
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.