## Clinical Scenario Analysis The imaging findings—mixed lytic-sclerotic lesion with cortical destruction, indistinct margins, and heterogeneous MRI signal—are highly suspicious for primary malignant bone tumor, most likely osteosarcoma given the patient's age (peak incidence 10–25 years) and distal femur location (most common site). ## Staging Before Biopsy: The Critical Principle **Key Point:** In suspected primary malignant bone tumors, systemic staging (CT chest ± abdomen/pelvis) MUST precede biopsy to: - Detect pulmonary metastases (present in ~20% of osteosarcoma at diagnosis) - Assess for skeletal metastases - Establish baseline for treatment planning - Avoid contaminating tissue planes before definitive imaging **High-Yield:** The biopsy tract itself becomes part of the surgical resection specimen; therefore, staging must be complete first to guide the surgical approach and margins. ## Why This Sequence? | Step | Rationale | |------|----------| | **1. CT chest** | Osteosarcoma has 15–20% pulmonary metastasis rate; changes staging and prognosis | | **2. CT abdomen/pelvis** | Assess for skeletal or visceral involvement | | **3. Biopsy** | Only after staging is complete; tissue diagnosis confirms malignancy | | **4. Treatment planning** | Surgery ± neoadjuvant chemotherapy based on stage | **Clinical Pearl:** Biopsy should be performed by the treating surgeon or under their guidance to ensure proper tract placement for eventual en bloc resection. ## Why Staging Matters in Osteosarcoma Osteosarcoma is a systemic disease at presentation in ~20% of cases. Staging determines: - Chemotherapy protocol (neoadjuvant vs. adjuvant) - Surgical margins and approach - Prognosis and survival estimates Skipping staging and proceeding directly to biopsy or chemotherapy risks incomplete treatment planning and suboptimal outcomes. 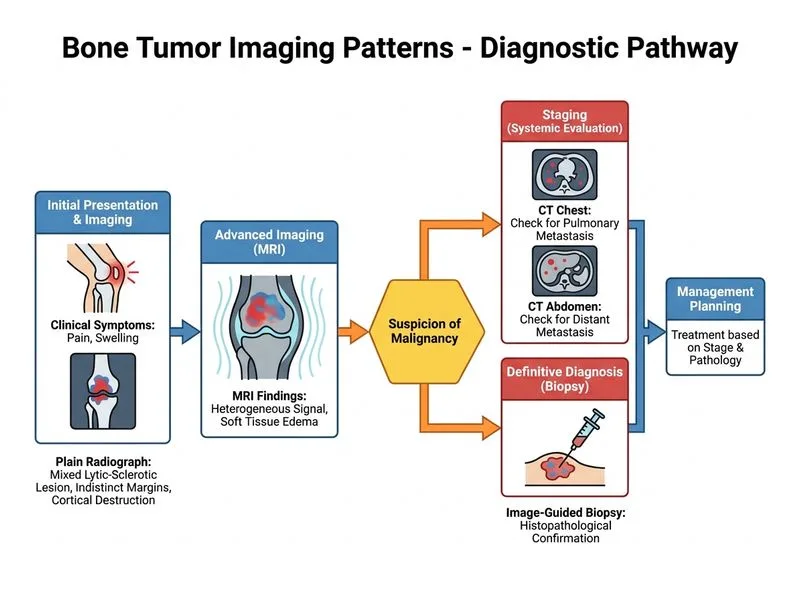
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.