## Diagnosis: Giant Cell Tumor of Bone ### Clinical Presentation A 28-year-old woman with a 6-month history of progressive right hip pain. Imaging reveals a well-defined, eccentric, lytic lesion in the **epiphysis** of the femoral head with a thin sclerotic rim, cortical bulging, no periosteal reaction, and MRI showing hemosiderin deposition and fluid-fluid levels. This constellation is classic for **Giant Cell Tumor (GCT) of bone**. ### Radiological Features **Key Point:** Giant cell tumor of bone is characterized by an eccentric, lytic lesion in the **epiphysis** (extending toward the articular surface) with a thin sclerotic rim, occurring in skeletally mature patients aged 20–40 years. The epiphyseal location in a skeletally mature patient is the single most important distinguishing feature. | Feature | GCT | ABC | Simple Cyst | Osteomyelitis | |---------|-----|-----|-------------|---------------| | **Age** | 20–40 years | 10–30 years | 5–15 years | Any age | | **Location** | Epiphysis (post-fusion) | Metaphysis/metadiaphysis | Metaphysis | Metaphysis/diaphysis | | **Pattern** | Eccentric, lytic | Eccentric, lytic | Central, lytic | Ill-defined, lytic | | **Sclerotic rim** | Thin, well-defined | Absent/thin | Thin | Absent | | **Fluid-fluid levels** | Occasionally present (secondary hemorrhage) | Frequently present | Absent | Absent | | **Periosteum** | Intact (no reaction) | Intact | Intact | Periosteal reaction | | **Cortical bulging** | Yes (expansile) | Yes (expansile) | Minimal | No | **High-Yield:** The **epiphyseal location in a skeletally mature patient** is the single most important distinguishing feature of GCT. Once the growth plates fuse, GCT characteristically arises in the epiphysis; aneurysmal bone cyst (ABC) typically arises in the metaphysis or metadiaphysis. ### Fluid-Fluid Levels: GCT vs. ABC **Clinical Pearl:** Fluid-fluid levels on MRI are classically associated with ABC and reflect blood-filled cavities with sedimentation. However, they are **not pathognomonic for ABC** — they can also occur in GCT due to secondary hemorrhage and cystic degeneration within the tumor (secondary ABC formation). In this vignette, the **epiphyseal location in a 28-year-old skeletally mature woman** is the decisive discriminator in favor of GCT. ABC occurs predominantly in younger patients (10–30 years) in the metaphysis, not the epiphysis. ### Pathological Basis GCT is a locally aggressive but usually benign tumor composed of mononuclear stromal cells (expressing RANKL) and multinucleated osteoclast-like giant cells. The eccentric, epiphyseal location with cortical expansion and a thin sclerotic rim reflects its slow growth and reactive bone formation at the margin. Hemosiderin deposition on MRI results from prior hemorrhage within the tumor. ### Why Not the Other Options? - **Simple bone cyst (A):** Central (not eccentric), metaphyseal, occurs in children (5–15 years); no fluid-fluid levels or hemosiderin. - **Aneurysmal bone cyst (D):** Metaphyseal/metadiaphyseal location, typically younger patients; fluid-fluid levels are common but the epiphyseal location here argues strongly against ABC. - **Osteomyelitis (C):** Ill-defined margins, periosteal reaction, clinical signs of infection; no fluid-fluid levels. ### Management & Prognosis Wide local excision or curettage with adjuvant therapy (phenol, cryotherapy, or bone cement) is standard. Recurrence rate is 10–65% depending on treatment method, making imaging follow-up essential. Malignant transformation is rare (~1–5%). Denosumab (anti-RANKL) is used for unresectable or recurrent cases. [cite:Robbins 10e Ch 26; Helms CA, Fundamentals of Skeletal Radiology 4e] 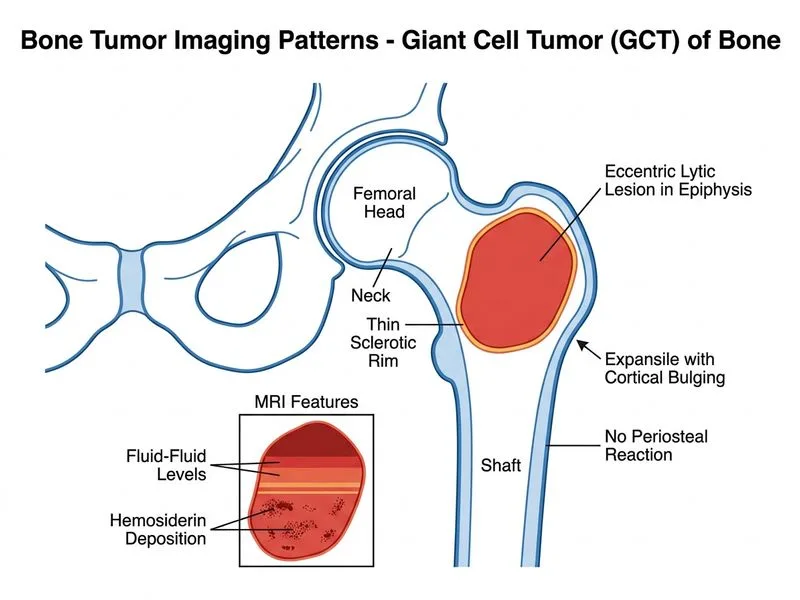
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.