## Clinical Context The clinical and radiological presentation is highly suggestive of **osteosarcoma**: - Age 16 (peak incidence 10–20 years) - Distal femur (most common site) - Sunburst periosteal reaction (aggressive malignancy) - Mixed lytic-sclerotic pattern with cortical destruction - Soft tissue extension ## Next Step: Staging Before Biopsy **Key Point:** In suspected bone malignancy, staging investigations MUST precede biopsy to avoid contamination of tissue planes and to guide surgical planning. **High-Yield:** The standard workup for osteosarcoma is: 1. **MRI of the primary site** — defines intramedullary and soft tissue extent, surgical margins, neurovascular involvement 2. **Chest CT** — detects pulmonary metastases (present in ~20% at diagnosis) 3. **Referral to orthopedic oncology** — ensures multidisciplinary planning before biopsy **Clinical Pearl:** Biopsy is performed AFTER staging, typically by the orthopedic oncologist in the operating room to avoid contaminating tissue planes that will be resected. ## Why This Approach? | Step | Rationale | |------|----------| | MRI first | Defines soft tissue and marrow involvement; essential for surgical planning | | Chest CT | Staging for metastases; prognostic and therapeutic implications | | Orthopedic oncology referral | Ensures coordinated biopsy, chemotherapy, and surgery | | Avoid open biopsy now | Contaminates tissue planes; increases surgical difficulty | **Mnemonic:** **STAMP** — **S**taging, **T**hen **A**ssess margins, **M**ultidisciplinary plan, **P**roceed to biopsy [cite:Robbins 10e Ch 26] 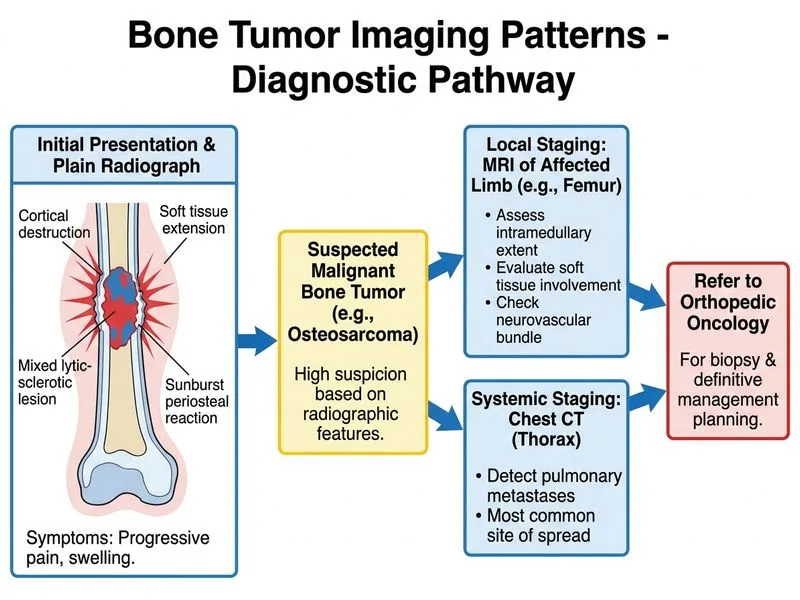
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.