## Management of Brachial Plexus Avulsion Injuries ### Clinical Context This patient presents with clinical features consistent with an **upper trunk brachial plexus injury** (C5–C6): - Loss of shoulder abduction (supraspinatus via suprascapular nerve) - Loss of external rotation (infraspinatus via suprascapular nerve) - Sensory loss over lateral shoulder (axillary nerve distribution) - Imaging suggesting avulsion at C5–C6 level ### Why MRI of the Brachial Plexus Is the Most Appropriate Immediate Next Step **Key Point:** Even when initial imaging (plain X-ray or CT) suggests avulsion, **MRI of the brachial plexus is the gold-standard confirmatory investigation** and is the essential next step before any surgical planning. **High-Yield:** MRI (particularly MRI myelography / MR neurography) is critical because: 1. It precisely delineates the **level and extent** of injury — distinguishing preganglionic (avulsion) from postganglionic (rupture) lesions, which fundamentally changes surgical strategy 2. It identifies associated injuries (pseudomeningocele, cord contusion, vascular injury) 3. Surgical planning for nerve grafting, nerve transfer, or free muscle transfer **cannot proceed safely without MRI confirmation** 4. It guides the neurosurgeon regarding donor nerve availability and reconstruction options **Clinical Pearl:** The distinction between avulsion (preganglionic) and rupture (postganglionic) is critical — avulsions cannot be directly repaired and require nerve transfers (e.g., intercostal, phrenic, contralateral C7), while ruptures may be amenable to direct grafting. MRI is the investigation that makes this distinction reliably (Narakas classification; Mackinnon & Dellon, *Surgery of the Peripheral Nerve*). ### Why Other Options Are Suboptimal | Option | Why Incorrect | |--------|---------------| | Urgent nerve grafting within 72 hours (Option A) | Surgical intervention for brachial plexus injuries is **not** performed within 72 hours; the standard practice is to confirm injury level with MRI, allow acute swelling to resolve, and operate at **3–6 weeks** post-injury. Rushing to the OR without MRI confirmation risks inappropriate surgery. | | High-dose corticosteroids + EMG at 3 weeks (Option B) | Corticosteroids have **no established role** in traumatic brachial plexus avulsion. EMG/NCS at 3 weeks is useful for prognostication but is not the *immediate* next step. | | Immobilization + physiotherapy alone (Option D) | Conservative management alone is inadequate for confirmed avulsion injuries; however, physiotherapy for passive ROM is an adjunct, not the primary immediate management step. | ### Standard Timeline for Brachial Plexus Avulsion Management 1. **Immediate (0–72 hours):** Stabilize patient, pain management, **MRI brachial plexus** to confirm level and extent 2. **Weeks 1–3:** EMG/NCS baseline; surgical planning 3. **Weeks 3–6:** Surgical exploration, nerve grafting/transfer 4. **Post-op:** Intensive physiotherapy, serial EMG/NCS to monitor reinnervation **High-Yield:** Per *Gray's Anatomy for Students* and *Mackinnon's Nerve Surgery*, MRI neurography is the investigation of choice for pre-surgical mapping of brachial plexus injuries and must precede any operative intervention. [cite: Mackinnon SE, Nerve Surgery, 2015; Tubbs RS, Nerves and Nerve Injuries, 2015; Moore KL, Clinically Oriented Anatomy 8e Ch 6] 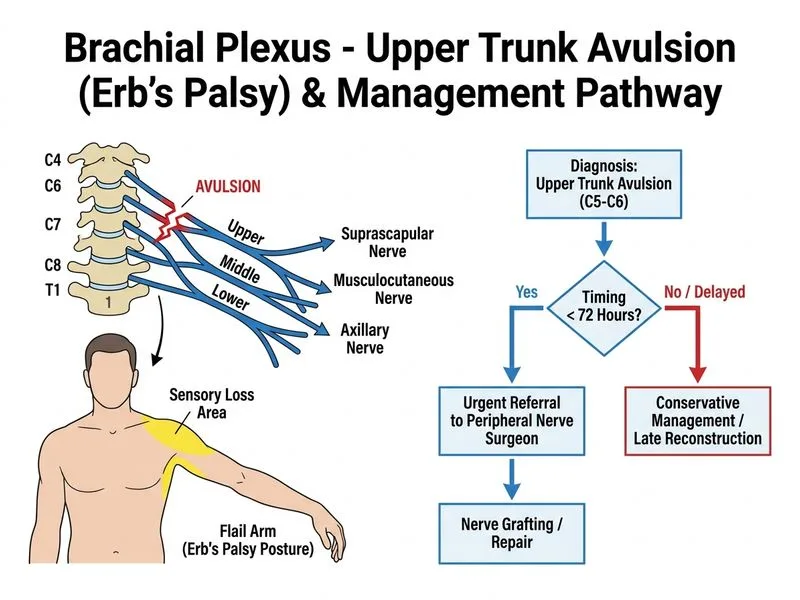
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.