## Clinical Diagnosis: Weber Syndrome (Ventromedial Midbrain Infarct) ### Anatomical Localization The combination of **bilateral CN III palsies (ptosis, ophthalmoplegia)** with **contralateral motor weakness (right-sided hemiparesis)** localizes the lesion to the **ventromedial midbrain**. This is Weber syndrome, caused by infarction in the territory of the **penetrating branches of the proximal basilar artery** or the **superior cerebellar artery**. ### Brainstem Cross-Section at Midbrain Level ```mermaid flowchart TD A[Ventromedial midbrain lesion]:::outcome --> B[Damages CN III nerve fibers]:::outcome B --> C[Bilateral ptosis + ophthalmoplegia]:::outcome A --> D[Damages corticospinal tract]:::outcome D --> E[Contralateral hemiparesis]:::outcome A --> F{Vascular territory?}:::decision F -->|Basilar perforators| G[Acute ischemic stroke]:::outcome F -->|Hemorrhage| H[Acute hemorrhagic stroke]:::outcome G --> I[IV thrombolysis if time window met]:::action H --> J[Supportive care + neurosurgical consultation]:::action ``` ### Pathophysiology 1. **Oculomotor nerve (CN III) fascicles** pass through the ventromedial midbrain → bilateral involvement causes ptosis and ophthalmoplegia 2. **Corticospinal tract** lies medial to CN III → damage causes contralateral hemiparesis 3. **Medial longitudinal fasciculus (MLF)** may be involved → internuclear ophthalmoplegia (INO) if bilateral **Key Point:** Weber syndrome is characterized by the combination of **ipsilateral CN III palsy + contralateral motor weakness**. When bilateral CN III involvement is present, the lesion is midline and ventromedial. ### Management of Acute Midbrain Stroke | Step | Action | Rationale | |------|--------|----------| | **1. Time assessment** | Determine exact time of symptom onset | Thrombolytic window is 0–4.5 hours | | **2. Neuroimaging** | MRI (or CT if MRI unavailable) to exclude hemorrhage | Mandatory before thrombolysis | | **3. Vascular imaging** | CTA/MRA to identify large vessel occlusion | Guides decision for thrombectomy | | **4. Thrombolysis** | IV alteplase if ischemic, within window, no contraindications | First-line acute stroke therapy | | **5. Monitoring** | ICU-level care; monitor for complications | Brainstem strokes carry high morbidity | **High-Yield:** Midbrain infarcts are often supplied by the **proximal basilar artery** and its penetrating branches. These are high-risk lesions because: - Bilateral CN III involvement indicates midline pathology - Corticospinal tract involvement causes significant motor disability - Risk of extension to pons or medulla is high **Clinical Pearl:** Unlike unilateral Weber syndrome (CN III on one side + contralateral hemiparesis), bilateral CN III involvement suggests a midline basilar artery occlusion with potential for rapid deterioration. This warrants urgent vascular imaging and consideration of mechanical thrombectomy if large vessel occlusion is confirmed. **Warning:** ~~Mannitol and head elevation~~ are temporizing measures for increased intracranial pressure but do NOT address the underlying ischemia. In acute ischemic stroke, reperfusion therapy (thrombolysis or thrombectomy) takes priority over osmotic therapy. ### Why IV Thrombolysis Is the Best Next Step - Acute ischemic stroke within potential thrombolytic window - No hemorrhage on imaging (assumed from clinical presentation) - Restores blood flow to ischemic midbrain and prevents further neuronal death - Guideline-recommended first-line therapy - Mechanical thrombectomy is considered AFTER IV thrombolysis if it fails or is contraindicated [cite:Harrison 21e Ch 297] 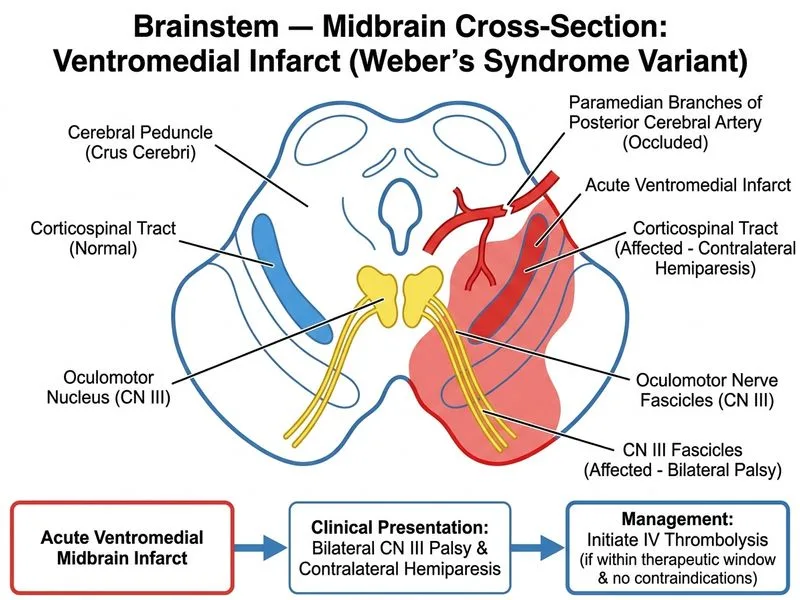
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.