## Clinical Context This patient has invasive ductal carcinoma with clinical evidence of axillary lymph node involvement (palpable 1.5 cm node). The presence of a clinically positive axillary node (cN1) mandates axillary lymph node dissection rather than sentinel lymph node biopsy alone. ## Surgical Decision-Making **Key Point:** In breast cancer, the choice between breast-conserving therapy (BCT) and mastectomy depends on: - Tumor size relative to breast volume - Ability to achieve negative margins - Patient preference - Presence of contraindications to BCT With a 2 cm tumor in a 48-year-old woman, BCT (wide local excision) would normally be considered. However, the presence of a **clinically palpable axillary lymph node** is a critical finding. ## Axillary Management Algorithm ```mermaid flowchart TD A[Breast cancer diagnosed]:::outcome --> B{Axillary nodes?}:::decision B -->|Clinically negative| C[SLNB]:::action B -->|Clinically positive| D[ALND]:::action C --> E{SLNB positive?}:::decision E -->|Yes| F[ALND]:::action E -->|No| G[No further axillary surgery]:::action D --> H[Modified Radical Mastectomy or BCT + ALND]:::action ``` **High-Yield:** Clinically positive axillary nodes (cN1) require **axillary lymph node dissection (ALND)**, not SLNB. SLNB is reserved for clinically node-negative (cN0) patients. ## Why Modified Radical Mastectomy (MRM) with ALND? 1. **Clinically positive axillary node** → ALND is mandatory 2. **2 cm tumor** → Could be managed with BCT if margins are adequate, BUT the presence of cN1 disease shifts the risk-benefit profile 3. **MRM** (removal of breast + axillary lymph nodes + pectoralis major fascia preservation) is the standard of care when ALND is indicated 4. BCT + ALND is an alternative IF the patient desires breast conservation and margins can be achieved; however, MRM is the most straightforward and commonly performed approach in this scenario **Clinical Pearl:** A clinically palpable axillary node in breast cancer is a strong indicator for axillary dissection. Modern practice increasingly uses imaging (ultrasound ± FNA) to confirm nodal involvement before surgery, but clinical examination findings guide the surgical plan. ## Staging Implication This patient is at least **Stage IIB–IIIA** (T2N1M0 or T2N2M0), depending on the exact number of involved nodes found at dissection. This mandates systemic therapy (chemotherapy ± hormonal therapy) in addition to surgery. 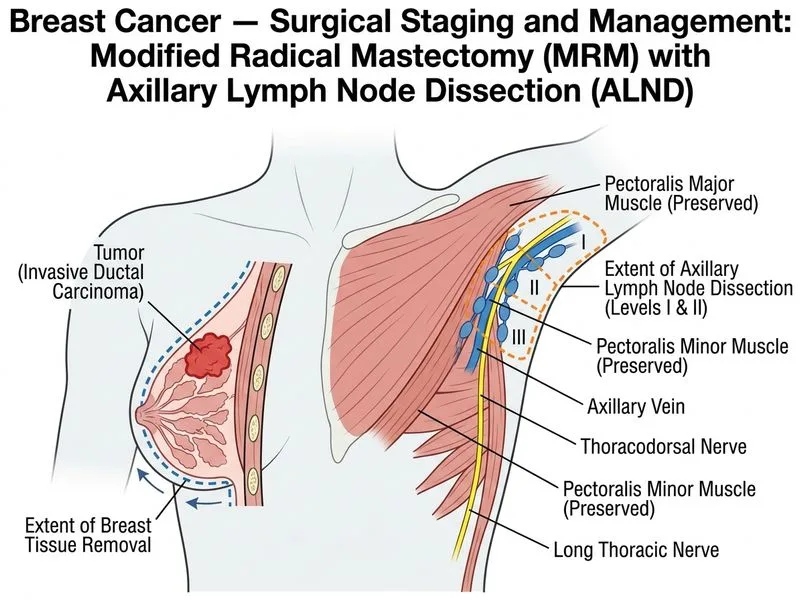
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.