## Diagnosis: Bullous Pemphigoid ### Clinical Presentation **Key Point:** Bullous pemphigoid (BP) is characterized by large, tense, intact blisters that do not rupture easily, typically affecting flexural areas, lower abdomen, and inner thighs in elderly patients. ### Histopathology & Immunofluorescence **High-Yield:** The hallmark finding is: - **Subepidermal blister** with eosinophil-rich infiltrate (eosinophils are prominent in BP) - **Linear IgG and C3 deposits along the basement membrane zone** on DIF — this is pathognomonic for BP ### Distinguishing Features from Other Bullous Disorders | Feature | Bullous Pemphigoid | Pemphigus Vulgaris | Linear IgA Disease | Dermatitis Herpetiformis | |---------|-------------------|-------------------|-------------------|------------------------| | **Blister level** | Subepidermal | Intraepidermal (acantholysis) | Subepidermal | Subepidermal | | **Blister integrity** | Tense, intact | Flaccid, ruptures easily | Variable | Vesicles (smaller) | | **Oral involvement** | Rare | Common (>90%) | Possible | No | | **Nikolsky sign** | Negative | Positive | Negative | Negative | | **DIF pattern** | Linear IgG + C3 at BMZ | Intercellular IgG ("tombstone") | Linear IgA at BMZ | Granular IgA at dermal–epidermal junction | | **Age of onset** | Elderly (>60 years) | Any age | Any age | Young adults | | **Eosinophils on histology** | Prominent | Absent | Variable | Absent | ### Clinical Pearl **Key Point:** Negative Nikolsky sign + negative oral involvement + linear IgG/C3 at BMZ = BP, not pemphigus. ### Pathophysiology **Mnemonic: BP-180 and BP-230** — Bullous pemphigoid autoantibodies target hemidesmosomal proteins (BP180 and BP230), leading to complement activation and subepidermal blister formation. ### Management Overview - Mild: Topical corticosteroids - Moderate to severe: Systemic corticosteroids (prednisolone 0.5–1 mg/kg/day) - Steroid-sparing agents: Azathioprine, mycophenolate mofetil [cite:Robbins 10e Ch 25] 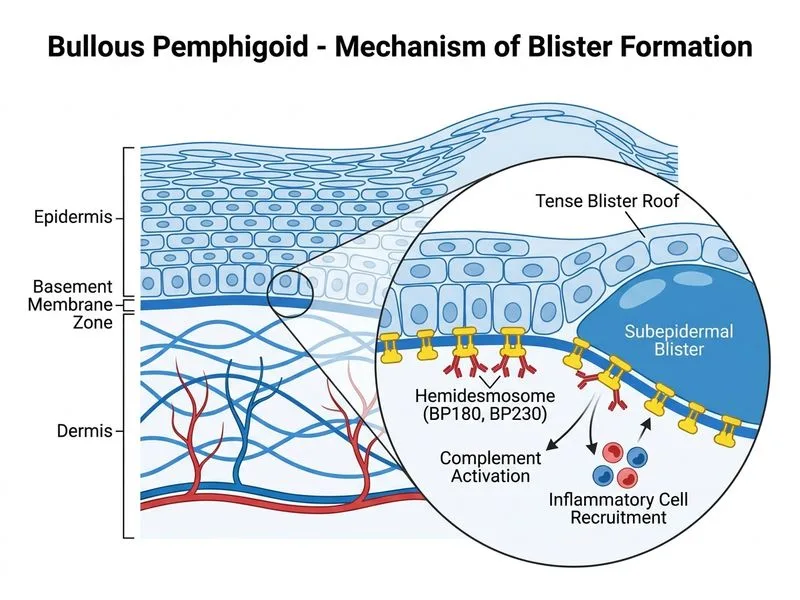
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.