## Diagnosis: Bullous Pemphigoid ### Clinical Presentation **Key Point:** Bullous pemphigoid presents with large, tense, intact blisters on flexural and lower abdominal skin, typically in elderly patients (>60 years). - Blisters are **non-flaccid** and do **not rupture easily** (unlike pemphigus) - **Negative Nikolsky sign** — pathognomonic for subepidermal blistering - **Absence of oral involvement** — oral mucosa is spared (cf. pemphigus vulgaris) - Urticarial or eczematous lesions may precede blisters ### Immunofluorescence Pattern **High-Yield:** DIF shows **linear IgG and C3 deposits at the basement membrane zone** — this is the gold standard for diagnosis. | Feature | Bullous Pemphigoid | Pemphigus Vulgaris | |---------|-------------------|--------------------| | Blister type | Tense, intact | Flaccid, ruptures easily | | Nikolsky sign | Negative | Positive | | Oral involvement | Rare | Common, often first site | | DIF pattern | Linear at BMZ | Intercellular IgG ("tombstone") | | Autoantigen | BP180, BP230 (hemidesmosomes) | Desmoglein 3 ± 1 | ### Pathophysiology **Key Point:** Autoantibodies against hemidesmosomal proteins (BP180 and BP230) cause subepidermal blistering at the dermal–epidermal junction. ### Treatment Approach 1. **First-line:** Topical or intralesional corticosteroids for localized disease 2. **Systemic:** Oral corticosteroids (prednisolone 0.5–1 mg/kg/day) for extensive disease 3. **Steroid-sparing agents:** Azathioprine, mycophenolate mofetil for long-term control **Clinical Pearl:** Bullous pemphigoid has a better prognosis than pemphigus vulgaris; many patients achieve remission or low-dose maintenance therapy. 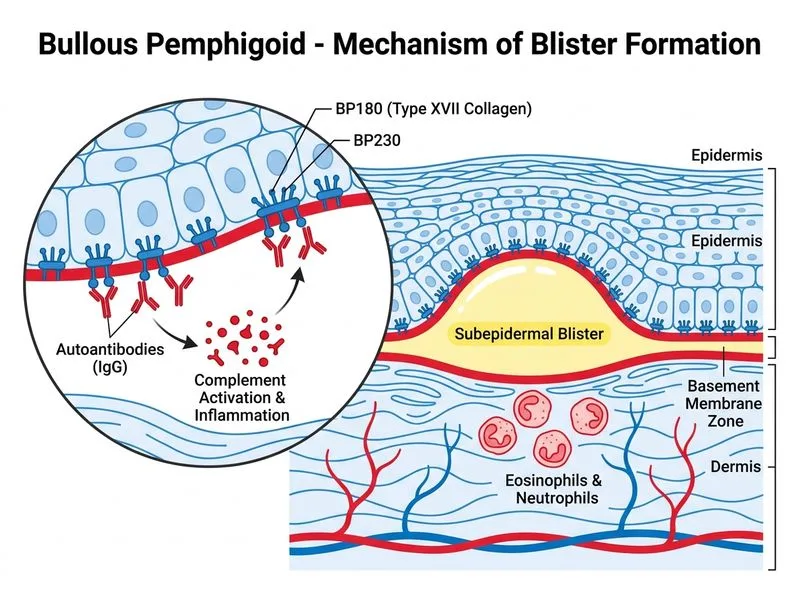
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.