## Management of Bullous Pemphigoid: First-Line Therapy ### Treatment Algorithm ```mermaid flowchart TD A[Bullous Pemphigoid Diagnosis Confirmed]:::outcome --> B{Extent of Disease?}:::decision B -->|Localized/Mild| C[Topical Corticosteroids ± Antihistamines]:::action B -->|Generalized/Moderate-Severe| D[Systemic Corticosteroids]:::action D --> E[Prednisolone 0.5-1 mg/kg/day]:::action E --> F[Taper over 3-6 months]:::action F --> G{Response Adequate?}:::decision G -->|Yes| H[Continue maintenance]:::action G -->|No/Steroid-Dependent| I[Add Steroid-Sparing Agent]:::action I --> J[Azathioprine or Mycophenolate]:::action ``` ### Why Systemic Corticosteroids Are First-Line **Key Point:** Systemic corticosteroids are the **gold standard first-line therapy** for generalized bullous pemphigoid. Prednisolone at **0.5–1 mg/kg/day** achieves remission in >90% of patients. ### Rationale for This Patient - **Generalized distribution** (lower legs AND abdomen) — not localized - **Multiple bullae over 2 months** — indicates progressive, moderate disease - **Positive serology** (circulating IgG) — suggests active, systemic autoimmunity - **No contraindications mentioned** — age alone is not a contraindication in elderly patients with BP ### Mechanism of Action Corticosteroids suppress: 1. T-cell activation and IL-2 production 2. Eosinophil recruitment and degranulation 3. Antibody production by B cells 4. Complement activation at the basement membrane ### Treatment Escalation Strategy | Stage | Therapy | Indication | |-------|---------|------------| | **Mild/Localized** | Potent topical steroids ± antihistamines | <10% BSA involvement | | **Moderate/Generalized** | Systemic prednisolone 0.5–1 mg/kg/day | >10% BSA; multiple bullae | | **Steroid-dependent** | Add azathioprine (1–2 mg/kg/day) or mycophenolate | Cannot taper below 10–15 mg/day | | **Severe/Refractory** | Rituximab, IV immunoglobulin, or plasmapheresis | Failure of conventional therapy | **High-Yield:** The goal is to achieve **complete remission within 4–8 weeks**, then gradually taper over 3–6 months to minimize long-term steroid toxicity. ### Clinical Pearl Unlike pemphigus vulgaris (which often requires higher doses and longer treatment), bullous pemphigoid responds more readily to lower-dose corticosteroids, and many patients achieve long-term remission or even cure after tapering. **Mnemonic: STEROID SPARING** — When to add steroid-sparing agents: - **S**teroid-dependent (cannot taper <10–15 mg/day) - **T**oxicity concerns (diabetes, osteoporosis, infections) - **E**arly introduction (some centers add at baseline in elderly) - **R**efractoriness to monotherapy - **O**ther comorbidities precluding high-dose steroids - **I**mmune suppression desired - **D**uration >3 months anticipated [cite:Robbins 10e Ch 25; Harrison 21e Ch 324] 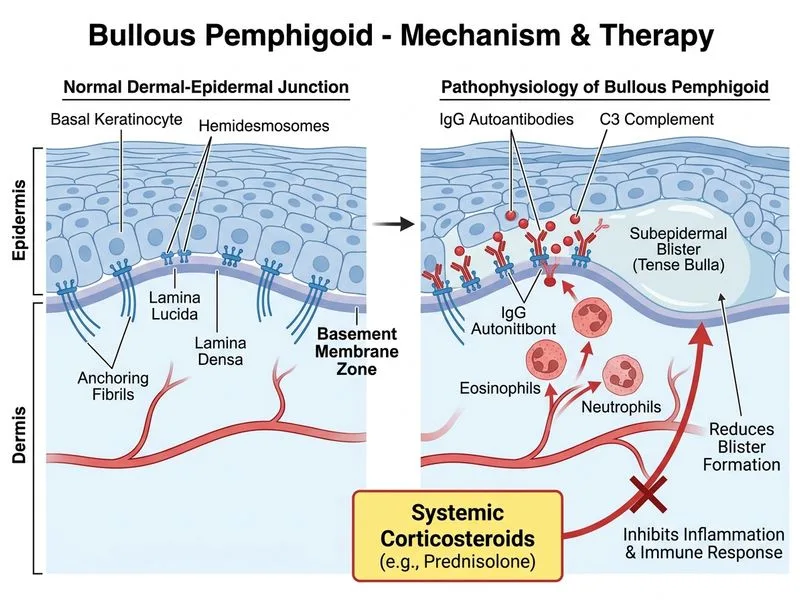
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.