## Molecular Confirmation of Bullous Pemphigoid ### Role of ELISA and Immunoblot in BP Diagnosis **Key Point:** ELISA or immunoblot assay using recombinant BP180 and BP230 antigens is the most specific molecular test for identifying and quantifying circulating autoantibodies in bullous pemphigoid. ### Why ELISA/Immunoblot is Superior for Molecular Confirmation | Investigation | Principle | Specificity | Sensitivity | Clinical Use | |---|---|---|---|---| | **ELISA (recombinant Ag)** | Detects IgG against purified BP180/BP230 | Very high (>95%) | 60–80% | Diagnostic confirmation; antibody quantification | | **Immunoblot** | Identifies specific epitopes on BP antigens | Very high | 70–85% | Molecular characterization; prognostic value | | **Indirect IF (human skin)** | Detects IgG binding to BMZ on tissue | Moderate specificity | 60–80% | Screening; less specific than ELISA | | **Salt-split skin IF** | Distinguishes dermal vs epidermal location | Moderate | 70–80% | Differentiates BP from pemphigoid variants | | **TEM** | Ultrastructural visualization | Not diagnostic | N/A | Research; shows hemidesmosomes | **High-Yield:** ELISA with recombinant antigens is superior to indirect IF because it: - Directly targets the pathogenic antigens (BP180 NC16A domain, BP230) - Eliminates cross-reactivity with other BMZ antigens - Quantifies antibody levels (useful for monitoring remission) - Is standardized and reproducible across laboratories ### Molecular Basis of BP Autoimmunity **Mnemonic: BP180/BP230 — **B**ullous **P**emphigoid antigens - **BP180 (BPAG2/Collagen XVII):** Transmembrane protein; NC16A domain is immunodominant - **BP230 (BPAG1):** Intracellular plakin; associated with more severe disease Anti-BP180 antibodies correlate with: - Active disease and blister formation - More severe phenotype - Slower remission Anti-BP230 antibodies correlate with: - Milder disease - Better prognosis - Seronegativity in some cases ### Clinical Application **Clinical Pearl:** When DIF is equivocal (as in this case), ELISA or immunoblot provides molecular confirmation by: 1. Identifying the specific autoantigen (BP180 vs BP230 vs both) 2. Quantifying antibody titers 3. Predicting disease severity and treatment response 4. Monitoring remission (antibody levels decline with successful therapy) ### Comparison with Other Investigations **Salt-split skin IF:** - Useful for distinguishing BP (dermal IgG/C3) from anti-p200 pemphigoid (epidermal IgG) - Less specific for BP180/BP230 identification than ELISA - Does not quantify antibodies **Indirect IF on human skin:** - Detects circulating antibodies but does not identify the specific antigen - Lower sensitivity (60–80%) than ELISA - Subject to variation depending on substrate quality **TEM:** - Shows ultrastructural features (hemidesmosomes, sub-basal lamina location of immune deposits) - Not diagnostic; research tool only 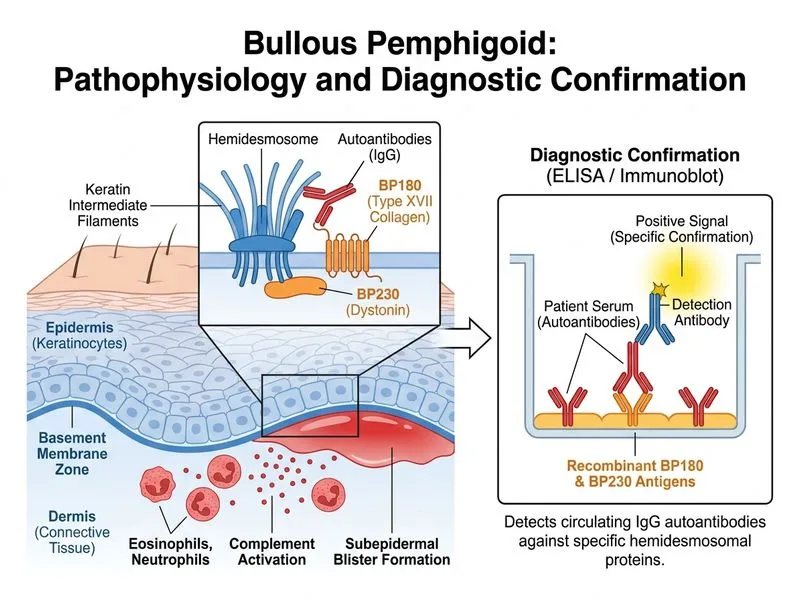
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.