## Diagnosis of Inhalation Injury in Burns **Key Point:** Fiberoptic bronchoscopy is the gold standard investigation for diagnosing inhalation injury in burn patients, particularly when clinical suspicion is high (singed nasal hairs, carbonized sputum, stridor). ### Why Fiberoptic Bronchoscopy? 1. **Direct visualization** of the tracheobronchial tree allows assessment of: - Mucosal edema and erythema - Carbonaceous deposits - Degree of airway obstruction - Need for intubation 2. **Timing and sensitivity:** Performed early (within 24 hours), it has high sensitivity for detecting thermal and chemical injury to airways. 3. **Guides management:** Findings directly influence decisions regarding: - Prophylactic intubation - Airway management strategy - Ventilator settings ### Why Other Investigations Are Insufficient | Investigation | Limitation | |---|---| | **ABG alone** | Detects hypoxemia/hypercarbia but cannot visualize airway injury; normal ABG does not exclude inhalation injury | | **CXR + COHb** | CXR may be normal early in inhalation injury; COHb useful for CO poisoning but does not assess airway structural damage | | **PFTs** | Cannot be reliably performed in acute burn setting; used for follow-up assessment, not acute diagnosis | **Clinical Pearl:** The **Abbreviated Injury Scale (AIS)** for inhalation injury grades findings on bronchoscopy (Grade 0–4), and Grade 3–4 (significant mucosal injury with obstruction) mandates intubation. **High-Yield:** Clinical signs of inhalation injury (singed nasal hairs, carbonized sputum, stridor, hoarseness) warrant bronchoscopy regardless of initial ABG or CXR findings, as airway edema can develop rapidly over 6–24 hours. **Mnemonic: SCOPE** — **S**inged hairs → **C**arbon deposits → **O**bstruction risk → **P**roactive bronchoscopy → **E**arly intubation if needed. 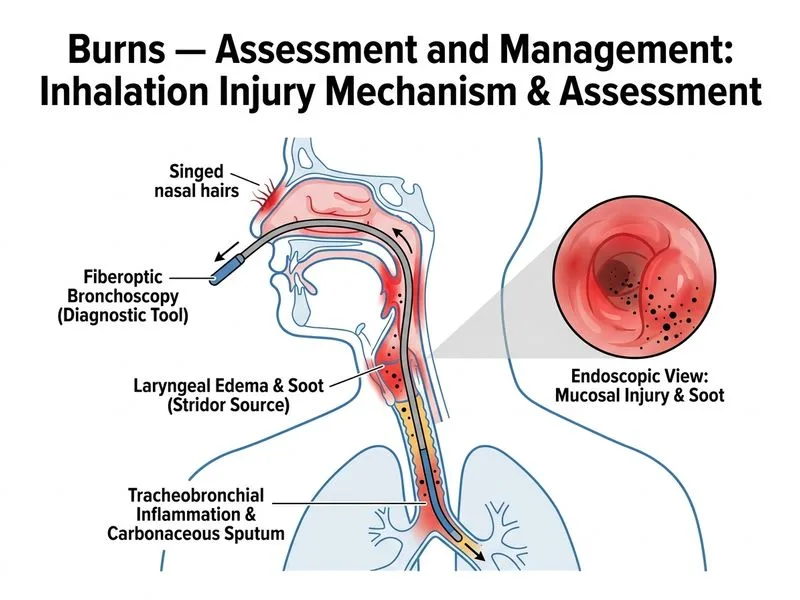
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.