## Clinical Context This patient is on post-injury day 3 with a 35% TBSA deep partial-thickness (2nd and 3rd degree) burn. She has successfully completed the resuscitation phase and is hemodynamically stable. The burned tissue is now at risk for infection, sepsis, and contracture. The focus shifts from fluid resuscitation to **wound management and prevention of complications**. ## Burn Depth Classification and Healing Potential | Depth | Appearance | Healing | Management | |-------|-----------|---------|-------------| | **Superficial (1st degree)** | Erythema, no blistering | Spontaneous (3–7 days) | Topical care only | | **Partial-thickness (2nd degree)** | Blistered, wet, painful, blanching | Spontaneous (2–3 weeks) if <15% TBSA; risk of scarring | Topical care ± grafting if >15% TBSA | | **Deep partial-thickness (deep 2nd degree)** | Blistered, leathery, minimal blanching | **Poor spontaneous healing**; high risk of infection & contracture | **Early excision & grafting** | | **Full-thickness (3rd degree)** | Charred, leathery, non-blanching | **No spontaneous healing** | **Mandatory excision & grafting** | **Key Point:** Deep partial-thickness and full-thickness burns (>15–20% TBSA) require **early tangential excision and autografting** to prevent infection, sepsis, and severe contractures. This is now the standard of care. ## Timing of Excision **High-Yield:** Early excision (within 24–72 hours of injury, ideally by day 3–5) is superior to delayed excision because: 1. Reduces bacterial colonization and sepsis risk 2. Minimizes inflammatory response and systemic complications 3. Reduces hospital stay and mortality 4. Improves functional and cosmetic outcomes 5. Decreases contracture formation This patient is on day 3 — the **ideal window for excision is now open**. ## Escharotomy vs. Tangential Excision **Mnemonic: ESCHAR = Emergency Surgery for Circumferential Airway/Hemodynamic Restriction** | Procedure | Indication | Timing | Goal | |-----------|-----------|--------|------| | **Escharotomy** | Circumferential burns causing compartment syndrome (decreased perfusion, loss of pulses) OR circumferential chest burns restricting ventilation | **Emergent** (within hours if compartment syndrome) | Relieve pressure; restore perfusion | | **Tangential excision** | Deep partial-thickness and full-thickness burns (any TBSA) | **Early** (day 3–5) | Remove all nonviable tissue; prepare for grafting | This patient has no signs of compartment syndrome (stable vitals, no mention of decreased perfusion), so escharotomy is not urgently needed. However, **tangential excision is the definitive management** for her deep partial-thickness burns. ## Why Not the Other Options? **Conservative topical care alone (Option 2):** - Deep partial-thickness burns do NOT heal well with topical agents alone - Risk of infection, sepsis, prolonged hospitalization - High risk of severe contractures and poor functional outcomes - This approach is outdated and is associated with increased mortality **Prophylactic antibiotics without excision (Option 3):** - Antibiotics do not prevent infection in devitalized tissue - Delaying excision until day 7 increases infection risk and worsens outcomes - Antibiotics are given only for **documented infection**, not prophylactically in burns - Early excision is more effective than antibiotics at preventing sepsis **Bedside eschar removal under local anesthesia (Option 4):** - Eschar removal requires operative anesthesia (general or regional) for adequate analgesia and hemostasis - Bedside removal is incomplete, painful, and risks hemorrhage - Must be done in the operating room with proper hemostasis and grafting capability ## Management Algorithm ```mermaid flowchart TD A[Deep partial-thickness or full-thickness burn]:::outcome A --> B{TBSA and timing?}:::decision B -->|Day 0-2: Resuscitation phase| C[Stabilize, fluid resuscitation, assess airway]:::action B -->|Day 3-5: Early excision window| D[Prepare for OR]:::action C --> E{Compartment syndrome or circumferential chest burn?}:::decision E -->|Yes| F[Emergent escharotomy at bedside]:::urgent E -->|No| D D --> G[Tangential excision under GA]:::action G --> H[Autografting with split-thickness skin]:::action H --> I[Healing and rehabilitation]:::outcome F --> J[Monitor perfusion; proceed to OR for excision]:::action J --> H ``` 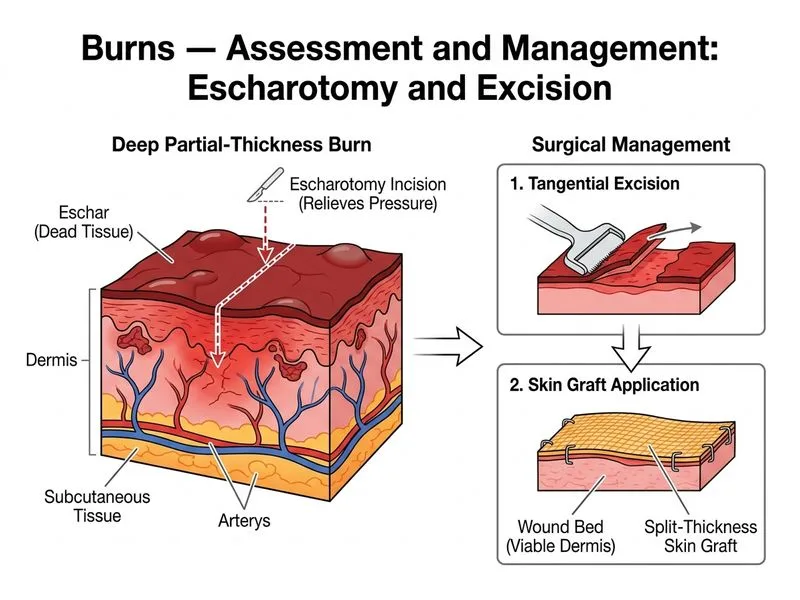
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.