## Diagnosis of Inhalation Injury **Key Point:** Fiberoptic bronchoscopy is the gold standard and most specific investigation for confirming inhalation injury in burn patients. It allows direct visualization of the airway for thermal injury, soot deposition, mucosal edema, and carbonaceous material. ### Why Fiberoptic Bronchoscopy is Superior **High-Yield:** Fiberoptic bronchoscopy provides: - Direct visualization of thermal damage to the airway mucosa - Identification of soot and carbonaceous debris in the tracheobronchial tree - Assessment of mucosal edema severity - Ability to grade the extent of injury (Abbreviated Injury Scale for inhalation) - Early detection of airway compromise requiring intubation ### Role of Other Investigations | Investigation | Finding in Inhalation Injury | Limitation | | --- | --- | --- | | COHb & ABG | ↑ COHb (if CO exposure); metabolic acidosis | Non-specific; may be normal early | | Chest X-ray | May show pulmonary edema, atelectasis (late) | Insensitive in first 24 hours; non-specific | | PFTs | Reduced FEV₁, FVC (if performed) | Impractical acutely; not diagnostic | **Clinical Pearl:** Clinical signs alone (singed nasal hairs, carbonaceous sputum, hoarseness) are suggestive but NOT diagnostic. Fiberoptic bronchoscopy is indicated when inhalation injury is suspected because early airway assessment guides intubation decisions and fluid resuscitation protocols. **Mnemonic — SCOPE for Bronchoscopy:** **S**oot visualization, **C**arbon deposits, **O**pportunity for early intubation, **P**rognostic grading, **E**dema assessment. ### Timing Bronchoscopy should be performed within the first 24–48 hours after admission to guide management and predict respiratory complications. 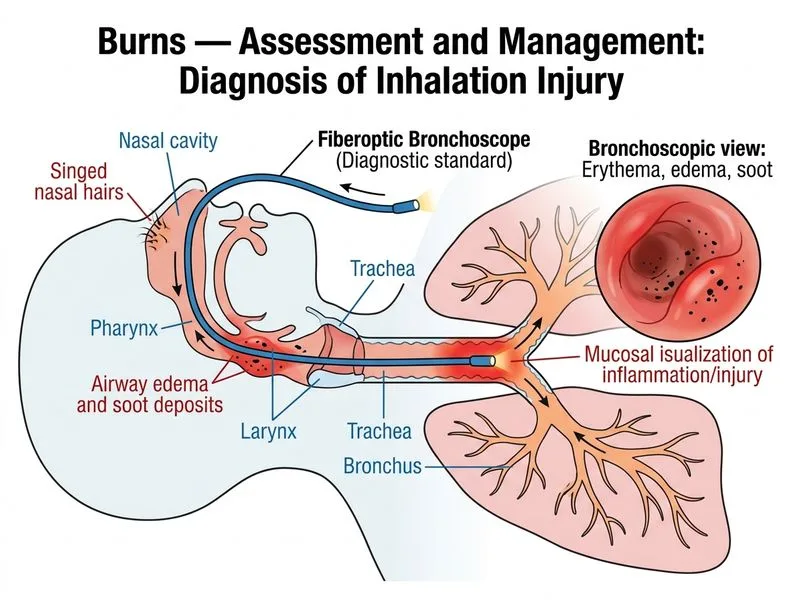
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.