## Timing and Indications for Surgical Intervention in Deep Burns **Key Point:** This patient has full-thickness (3rd degree) burns with clear demarcation, which are characterized by painless, leathery, charred tissue that will NOT heal spontaneously. Early excision and grafting is the standard of care for deep burns and significantly improves outcomes. ### Burn Depth and Healing Potential | Depth | Appearance | Pain | Spontaneous Healing | Management | |-------|-----------|------|-------------------|-------------| | Partial-thickness (2nd degree) | Blistered, moist, red | Painful | Yes (2–3 weeks) | Conservative + topical care | | Full-thickness (3rd degree) | Charred, leathery, white/brown | Painless | No — requires grafting | Early excision + skin grafting | | 4th degree | Muscle/bone involvement | Painless | No — requires amputation | Surgical debridement + amputation | **High-Yield:** Early excision and grafting (performed within 24–72 hours, ideally by day 5) is superior to delayed grafting because it: 1. Reduces bacterial proliferation in the eschar 2. Decreases systemic inflammatory response and sepsis risk 3. Shortens hospital stay 4. Improves functional and cosmetic outcomes 5. Reduces contracture formation ### Surgical Management Timeline ```mermaid flowchart TD A[Full-thickness burn identified]:::outcome --> B[Stabilize patient: fluids, airway]:::action B --> C{TBSA and patient stability?}:::decision C -->|Small <5% TBSA| D[Can delay grafting]:::action C -->|Large >5% TBSA| E[Plan early excision]:::action E --> F[Timing: day 1–5 post-injury]:::action F --> G[Tangential excision to viable tissue]:::action G --> H[Autologous skin graft or temporary coverage]:::action H --> I[Monitor graft take and infection]:::outcome A --> J[Resuscitation ongoing]:::action J --> K[Assess for inhalation injury]:::action K --> L[Nutritional support]:::action ``` **Clinical Pearl:** The eschar in full-thickness burns acts as a foreign body and a nidus for bacterial growth. It must be surgically removed (excised) and replaced with viable tissue (autograft, allograft, or temporary dressing). Conservative management with topical agents alone will NOT prevent eschar separation, infection, and sepsis. **Warning:** Delaying excision beyond 7–10 days increases infection risk, particularly from beta-hemolytic streptococci and Pseudomonas aeruginosa. Prophylactic antibiotics are NOT a substitute for early excision. **Mnemonic:** **ESGRAFT** — **E**arly excision, **S**kin grafting, **G**raft monitoring, **R**esuscitation, **A**ntibiotics (therapeutic, not prophylactic), **F**unctional rehabilitation, **T**emperature control. ## Why Early Excision Is Standard Full-thickness burns have no viable epithelium and cannot heal spontaneously. The eschar becomes necrotic tissue that promotes bacterial overgrowth and systemic infection. Early surgical excision removes this source of infection and allows coverage with autologous skin (gold standard) or temporary biological dressing, dramatically improving survival and reducing morbidity. 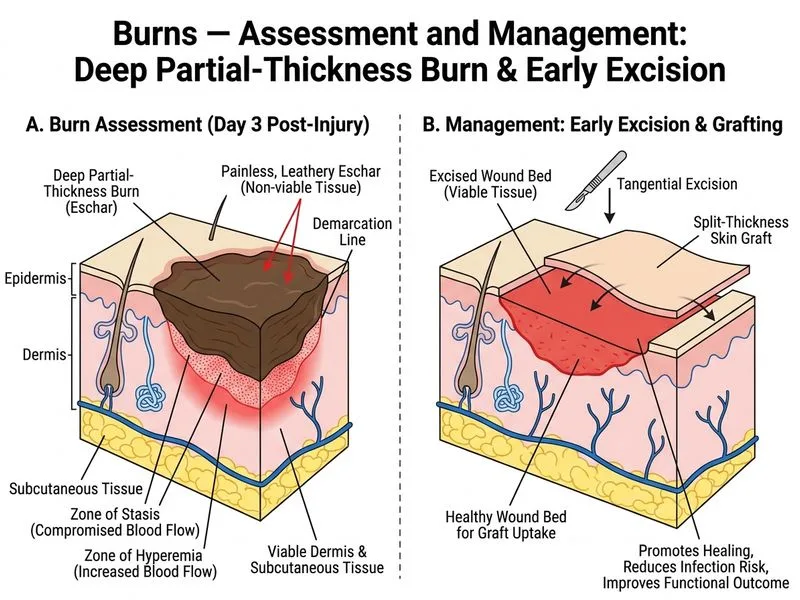
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.