## Clinical Context: Acute Aortic Regurgitation with Inferior STEMI This patient has acute aortic regurgitation (AR) secondary to aortic dissection or endocarditis complicated by an acute inferior myocardial infarction. The combination of new early diastolic murmur, ST elevation, and echocardiographic evidence of a flail cusp indicates a surgical emergency. ## Pathophysiology of Acute AR **Key Point:** In acute aortic regurgitation, the left ventricle has not had time to dilate and compensate. The sudden volume overload during diastole causes: - Premature mitral valve closure (before atrial contraction) - Elevated left ventricular end-diastolic pressure (LVEDP) - Pulmonary edema and cardiogenic shock - Reduced coronary perfusion pressure (widened pulse pressure) Unlike chronic AR, acute AR is poorly tolerated and rapidly decompensates. ## Rationale for Nitroprusside + Emergency Catheterization 1. **Afterload reduction** is the cornerstone of acute AR management: - Nitroprusside (or hydralazine) reduces systemic vascular resistance - This decreases the regurgitant fraction and improves forward flow - Reduces LVEDP and pulmonary congestion 2. **Emergency catheterization** serves dual purposes: - Confirms the diagnosis of acute AR and identifies the etiology (dissection vs. endocarditis) - Enables primary PCI for the concurrent inferior STEMI - Allows hemodynamic monitoring via Swan-Ganz catheter 3. **Definitive surgical repair/replacement** is indicated urgently once the acute MI is managed, as acute AR with hemodynamic compromise is a surgical emergency. **High-Yield:** Acute AR + STEMI = medical stabilization (afterload reduction) → emergency catheterization (PCI for MI) → urgent surgical consultation for valve intervention. **Clinical Pearl:** Beta-blockers are contraindicated as monotherapy in acute AR because they increase diastolic time, worsening regurgitation. Afterload reduction must precede any beta-blockade. ## Cardiac Cycle Correlation In acute AR, the regurgitant jet during diastole (when the aortic valve should be closed) floods the left ventricle at high pressure. This disrupts the normal diastolic filling phase and elevates LVEDP, compromising both diastolic function and coronary perfusion. 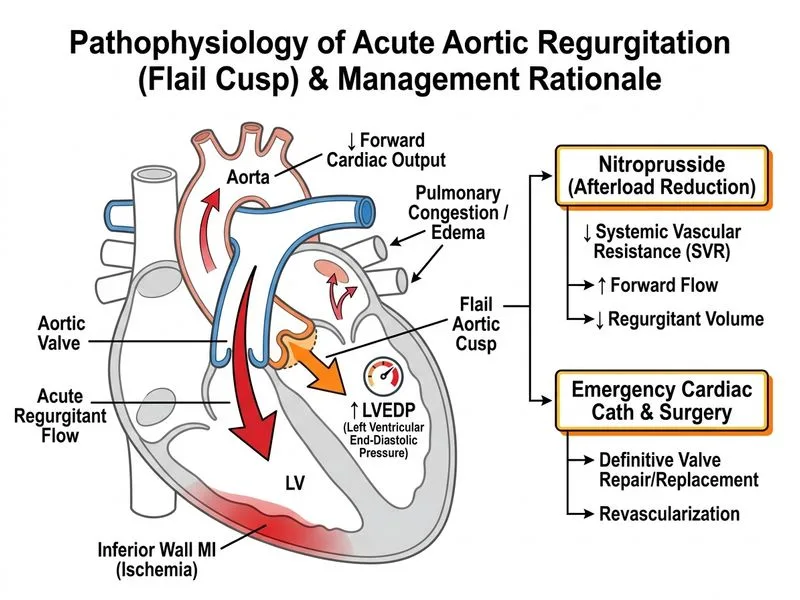
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.