## Distinguishing AMI from Unstable Angina: Role of Cardiac Biomarkers ### The Diagnostic Challenge in Early ACS **Key Point:** In the first 6 hours of symptom onset, clinical presentation and ECG findings may overlap significantly between AMI and unstable angina. Cardiac biomarkers are the gold standard for detecting myocardial necrosis. ### Cardiac Biomarkers as the Best Discriminator **High-Yield:** Elevated cardiac troponins (I or T) or myoglobin on **serial measurement** (baseline, 3 hours, 6 hours) definitively indicate myocardial necrosis and distinguish AMI from unstable angina. - **Troponin I/T:** Most specific for myocardial injury; rise begins at 2–4 hours, peaks at 24–48 hours, remains elevated for 7–14 days - **Myoglobin:** Earliest marker (rises within 1–2 hours) but less specific; useful for early rule-out - **CK-MB:** Traditional marker; rises at 3–12 hours, peaks at 24–48 hours - **Serial measurement is critical:** A single negative troponin at presentation does NOT exclude AMI; repeat at 3 and 6 hours is standard practice **Mnemonic:** **TROP** = **T**roponin **R**ises **O**ver **P**eriod (serial measurement required) ### Why Other Options Are Inadequate Discriminators | Feature | AMI | Unstable Angina | Discriminatory Value | |---------|-----|-----------------|---------------------| | **Chest pain + diaphoresis** | Often present | Can also occur | Low specificity | | **ST elevation on ECG** | Typical in STEMI | Absent in NSTEMI/UA | Good for STEMI but not for NSTEMI vs UA | | **Positive angiography** | Shows occlusion/stenosis | Shows stenosis/plaque | Does not prove active necrosis | | **Elevated biomarkers** | Present | Absent | **HIGH specificity for necrosis** | **Clinical Pearl:** Approximately 20–30% of AMIs present without ST elevation (NSTEMI); in these cases, **troponin elevation is the only way to distinguish NSTEMI from unstable angina**. Angiography may show similar lesions in both conditions. **Warning:** A single negative troponin at presentation does NOT rule out AMI. The "rule-out" protocol requires serial measurement at 0, 3, and 6 hours (or high-sensitivity troponin at 0 and 3 hours). ### Diagnostic Algorithm ```mermaid flowchart TD A[Acute Chest Pain]:::outcome --> B{ST elevation on ECG?}:::decision B -->|Yes| C[STEMI]:::outcome B -->|No| D[Measure troponin at 0h]:::action D --> E{Troponin elevated?}:::decision E -->|Yes| F[NSTEMI]:::outcome E -->|No| G[Repeat troponin at 3h and 6h]:::action G --> H{Any elevation?}:::decision H -->|Yes| I[NSTEMI]:::outcome H -->|No| J[Unstable Angina or other diagnosis]:::outcome ``` [cite:Harrison 21e Ch 297] 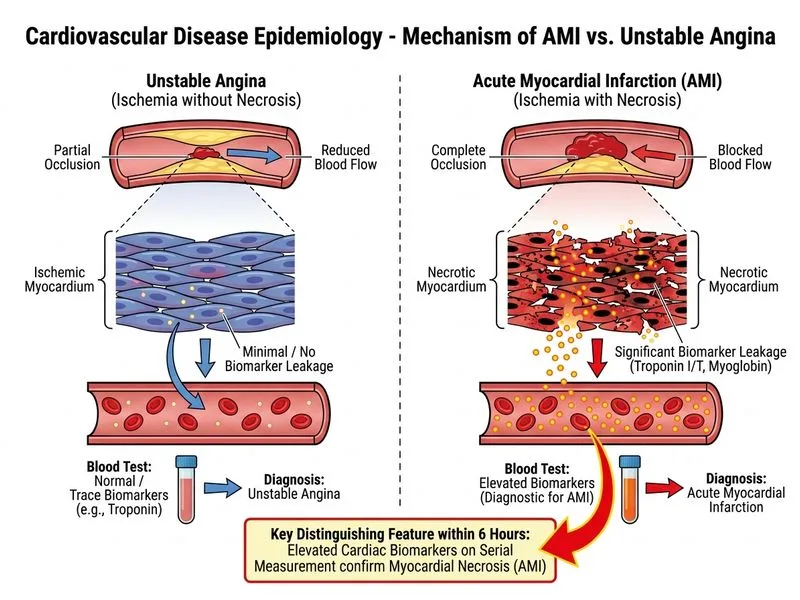
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.