## Postoperative Hyperopia After Cataract Surgery ### Analysis of Refractive Outcome **Key Point:** The patient achieved +1.50 D of hyperopia postoperatively, indicating that the IOL power was stronger than predicted (or the eye became more hyperopic than expected). This is a **hyperopic shift** or **undercorrection** relative to the emmetropia target. ### Causes of Unexpected Hyperopia **High-Yield:** Common causes include: 1. **Inaccurate biometry** — Most common cause; A-scan or keratometry error. 2. **IOL power miscalculation** — Formula error or incorrect A-constant. 3. **Effective lens position (ELP) prediction error** — The IOL sits deeper or shallower than predicted. 4. **Posterior capsule contraction** — Occurs weeks to months postoperatively, not on POD 1. 5. **Corneal flattening** — From surgical trauma (less likely on POD 1 with intact capsule). ### Differential Diagnosis of Refractive Error | Cause | Timing | Refraction | Investigation | |-------|--------|-----------|----------------| | Biometry error | Immediate | Hyperopic or myopic shift | Repeat A-scan, keratometry | | IOL power error | Immediate | Opposite of target | Verify IOL power in eye | | ELP misprediction | Immediate | Hyperopic (IOL too weak) | Assess IOL position on OCT | | Posterior capsule contraction | Weeks–months | Progressive myopic shift | Slit-lamp examination | | Corneal edema | POD 1–3 | Transient myopic shift | Resolves with time | **Clinical Pearl:** On postoperative day 1 with intact posterior capsule and good visual acuity (6/6 with correction), the most likely cause is a **biometry or IOL power error** rather than a structural complication. ### Recommended Management **Step 1: Verify IOL Power** - Confirm the IOL power implanted matches the surgical plan (check operative note and IOL box). - If discrepancy exists, document for future reference and plan refractive correction. **Step 2: Assess Refractive Stability** - Defer final refraction until 4–6 weeks postoperatively to allow corneal edema to resolve and IOL position to stabilize. - The +1.50 D hyperopia may partially resolve as corneal clarity improves. **Step 3: Refractive Correction Options** - If hyperopia persists at 6 weeks: **Spectacle correction** (safest, reversible) or **contact lens** (if patient prefers). - **IOL exchange** is rarely indicated for a +1.50 D error unless patient is highly motivated and biometry is confirmed accurate. - **Refractive surgery** (LASIK, PRK) can be considered if the patient desires monovision or if the contralateral eye is myopic. **Warning:** Do NOT perform IOL exchange on POD 1 based on refraction alone. Wait for refractive stability and verify biometry accuracy first. ### Why This Outcome Is Manageable - **Visual acuity is good** (6/6 with correction) — the IOL is well-centered and the eye is optically healthy. - **Hyperopia is mild** (+1.50 D) — easily corrected with spectacles or contact lenses. - **No structural complications** — intact capsule, centered IOL, no inflammation. 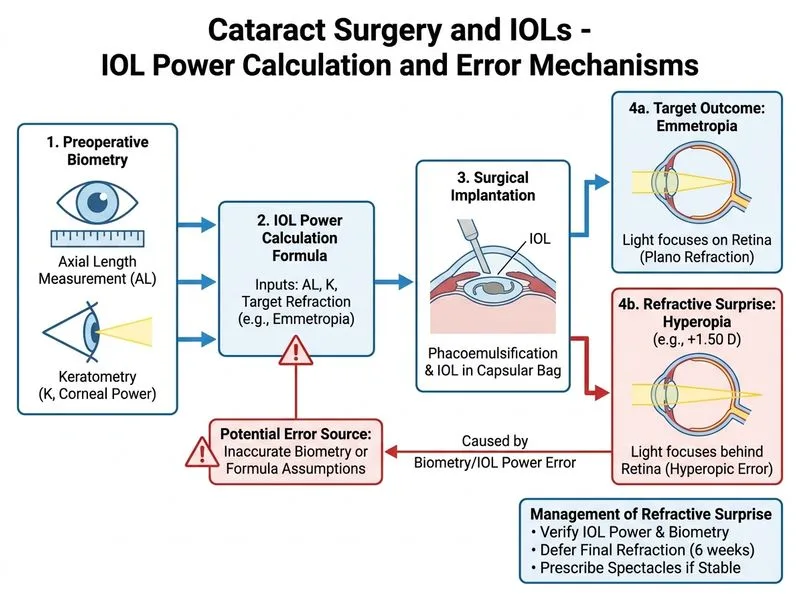
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.