## Posterior Subcapsular Cataract (PSC) — Steroid-Induced **Key Point:** Posterior subcapsular cataracts are strongly associated with chronic corticosteroid use and are characterized by vacuoles and water clefts in the posterior cortex, just anterior to the posterior capsule. ### Etiology and Risk Factors **High-Yield:** Corticosteroids are the most common **modifiable risk factor** for posterior subcapsular cataract. The risk is dose- and duration-dependent: - Systemic corticosteroids (especially >15 mg/day prednisolone for >1 year) - Topical corticosteroids (chronic use, especially potent agents) - Inhaled corticosteroids (lower risk than systemic) **Mnemonic: PSC Risk Factors — "SCRAP"** - **S**teroids (systemic, topical, inhaled) - **C**omplications of diabetes (osmotic stress) - **R**adiation (UV, ionizing) - **A**ging (age >60) - **P**ancreatic disease (myotonic dystrophy, galactosemia) ### Pathophysiology 1. Corticosteroids disrupt the Na⁺/K⁺-ATPase pump in lens epithelial cells 2. Osmotic imbalance → water influx into lens fibers 3. Formation of **vacuoles** and **water clefts** in the posterior cortex 4. Posterior location due to direct diffusion of steroids through the posterior capsule ### Clinical Features of PSC | Feature | Details | |---------|----------| | **Location** | Posterior cortex, just anterior to posterior capsule | | **Morphology** | Vacuoles, water clefts, breadcrumb appearance | | **Onset** | Relatively rapid (weeks to months with high-dose steroids) | | **Visual symptoms** | Glare and difficulty with bright light (disproportionate to opacity) | | **Refraction** | Minimal refractive change | | **Reversibility** | Partially reversible if steroids stopped early; permanent if advanced | **Clinical Pearl:** Patients with PSC often report **disproportionate visual symptoms** — they complain of significant glare and difficulty reading despite relatively mild opacity on slit-lamp examination. This is because the posterior location of the opacity disrupts the visual axis more than a cortical opacity of similar density. ### Why This Patient Has PSC - Chronic corticosteroid use for rheumatoid arthritis (classic risk) - Posterior cortical location with vacuoles and water clefts (pathognomonic morphology) - Age 65 (additional age-related risk) ### Management 1. **Reduce corticosteroid dose** if possible (may halt progression or cause partial reversal) 2. **Surgical referral** when cataract affects vision (phacoemulsification) 3. **Prophylaxis:** Use lowest effective corticosteroid dose; consider topical NSAIDs (may reduce risk) 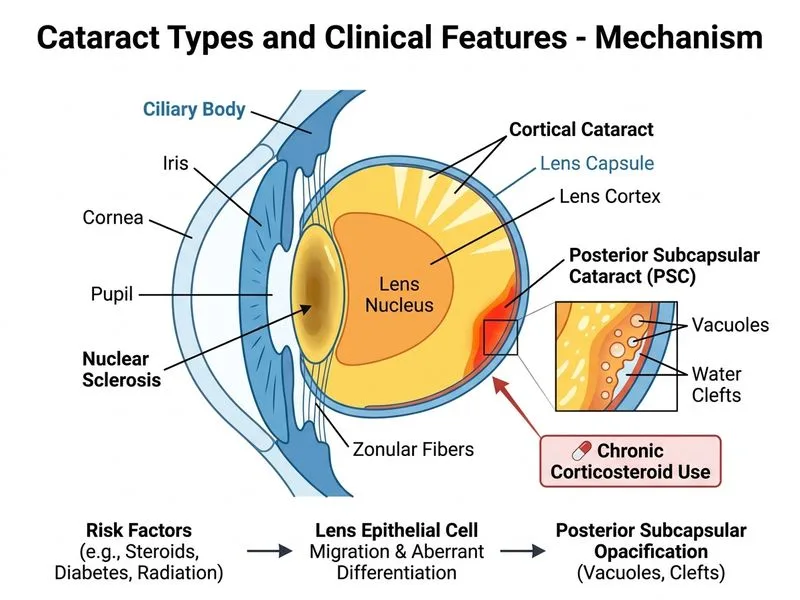
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.