## Clinical Presentation: Cavernous Sinus Thrombosis (CST) The clinical triad of **ophthalmoplegia** (CN III, IV, VI involvement), **proptosis**, and **chemosis** with fever and headache is pathognomonic for cavernous sinus thrombosis. ## Why Immediate Antibiotics? **Key Point:** Cavernous sinus thrombosis is a medical emergency with mortality rates of 20–40% if untreated. Delays in antibiotic initiation directly correlate with poor outcomes. **High-Yield:** The source is often a paranasal sinus infection (ethmoid, sphenoid), otitis media, or facial furuncles (especially the "danger triangle" of the face). Common pathogens include *Staphylococcus aureus* (including MRSA), *Streptococcus pneumoniae*, and gram-negative organisms. ## Management Algorithm ```mermaid flowchart TD A[Clinical suspicion of CST]:::outcome --> B{Imaging available immediately?}:::decision B -->|No| C[Start broad-spectrum IV antibiotics NOW]:::action B -->|Yes| D[Quick CT/MRI to confirm diagnosis]:::action C --> E[Imaging after antibiotics started]:::action D --> E E --> F[Blood cultures, LP if no contraindication]:::action F --> G[Continue antibiotics for 4-6 weeks]:::action G --> H[Treat primary source]:::action ``` **Clinical Pearl:** Do NOT delay antibiotics waiting for imaging, LP, or culture results. Empirical broad-spectrum coverage is started **immediately** based on clinical diagnosis. Imaging and cultures are obtained **concurrently** or immediately after antibiotics are initiated. **Warning:** Lumbar puncture is NOT the first step — it delays life-saving antibiotics and carries risk if there is raised intracranial pressure. LP is done only if meningitis is suspected AND no contraindications exist, but it should never delay antibiotic initiation. ## Empirical Antibiotic Regimen | Agent | Rationale | |-------|----------| | Ceftriaxone 2g IV Q12H | Third-generation cephalosporin; good CNS penetration; covers *Streptococcus*, gram-negatives | | Vancomycin 15–20 mg/kg IV Q8–12H | Covers MRSA and penicillin-resistant *Streptococcus pneumoniae* | | ± Metronidazole 500 mg IV Q6H | Added if anaerobes suspected (e.g., from dental/sinus source) | **Mnemonic:** **STAT-AB** = **S**tart **T**herapy **A**t **T**riage, **A**void **B**elayed antibiotics. ## Why Not the Other Options? - **Lumbar puncture first:** Delays antibiotics; CST may cause raised ICP, making LP risky. - **Imaging before antibiotics:** Imaging is important for confirmation and source identification, but should NOT delay empirical therapy. - **Antifungal monotherapy:** Fungal CST is rare; bacterial pathogens dominate. Antifungals are added only if fungal infection is suspected (immunocompromised, specific risk factors). 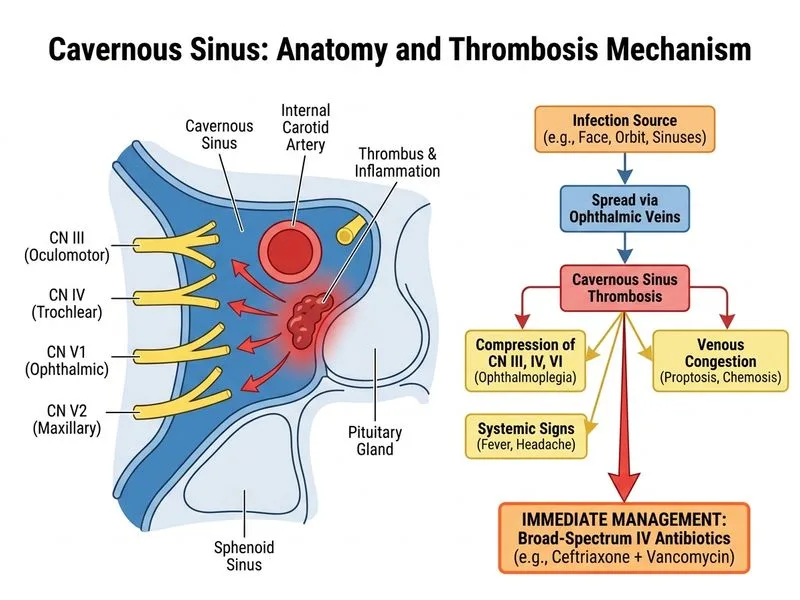
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.