## Clinical Diagnosis: Septic Cavernous Sinus Thrombosis **Key Point:** Cavernous sinus thrombosis (CST) is a medical emergency with mortality rates of 5–10% even with treatment. The classic triad is fever, headache, and ophthalmoplegia (CN III, IV, VI involvement). Proptosis and chemosis are common. **High-Yield:** Septic CST typically arises from: - Paranasal sinusitis (ethmoid > sphenoid > maxillary) - Facial furuncles ("danger triangle" of face) - Otitis media/mastoiditis - Dental infections This patient has fever, headache, and CN palsies (CN III, IV, VI) — classic presentation. ## Management Algorithm ```mermaid flowchart TD A[Suspected Cavernous Sinus Thrombosis]:::outcome --> B{Septic or Aseptic?}:::decision B -->|Septic| C[Blood cultures + IV broad-spectrum antibiotics]:::action B -->|Aseptic| D[Anticoagulation ± corticosteroids]:::action C --> E[MRI/MRV/MRA to confirm diagnosis]:::action D --> E E --> F[Identify source of infection]:::action F --> G[Source control: ENT/Dental/Neurosurgical intervention]:::action ``` ## Immediate Management Steps 1. **Blood cultures** — obtain before antibiotics (if possible without delay) 2. **Broad-spectrum IV antibiotics** — start immediately (do NOT wait for culture results) - Ceftriaxone 2 g IV 6-hourly - Vancomycin 15–20 mg/kg IV 8–12-hourly (for MRSA coverage) - Consider adding metronidazole if anaerobic source suspected 3. **Neuroimaging** — MRI brain with contrast + MRV/MRA to: - Confirm diagnosis (loss of normal flow void, hyperintense thrombus) - Exclude abscess, empyema - Assess venous patency 4. **Identify source** — imaging of paranasal sinuses, mastoid, dental evaluation 5. **Source control** — ENT/neurosurgical intervention as needed **Clinical Pearl:** Lumbar puncture is contraindicated in suspected CST due to risk of herniation from raised intracranial pressure. Blood cultures and imaging take priority. **Warning:** Anticoagulation (heparin) is NOT standard for septic CST; it is reserved for aseptic thrombosis (e.g., hypercoagulable states, thrombophilia). Septic CST requires antibiotics and source control. **High-Yield:** Do NOT delay antibiotics waiting for LP or imaging. Start empiric broad-spectrum coverage immediately in suspected septic CST. [cite:Harrison 21e Ch 381] 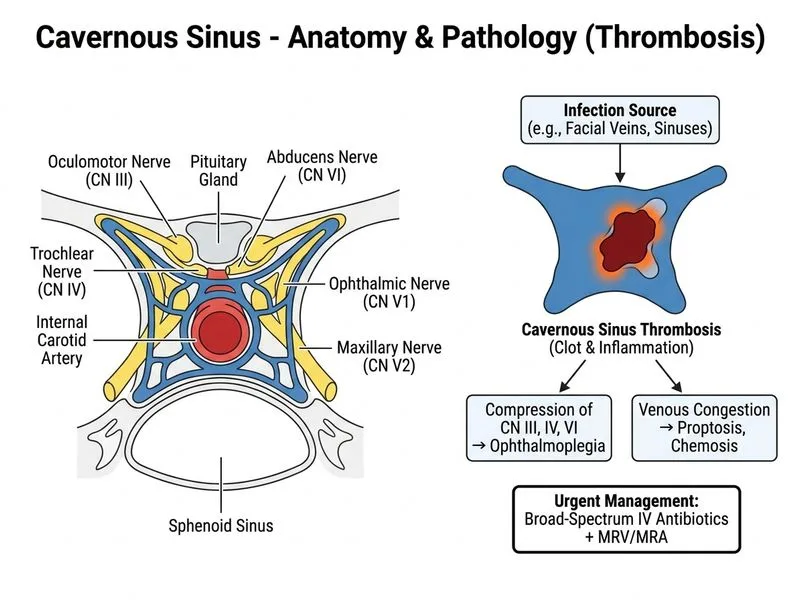
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.