## Clinical Context The patient presents with a clinical and histological picture consistent with **uterine leiomyoma (fibroid)** — a benign smooth muscle tumor arising from myometrial hyperplasia and hypertrophy. The key diagnostic challenge is determining the extent of myometrial invasion and relationship to the endometrial cavity. ## Investigation of Choice: Pelvic MRI with T1 and T2-Weighted Sequences **Key Point:** Pelvic MRI is the gold standard for fibroid assessment because it: 1. **Characterizes tissue composition** — T2-weighted imaging distinguishes fibroids (low signal) from adenomyosis (high signal with ill-defined margins) 2. **Maps myometrial involvement** — determines submucosal, intramural, and subserosal components (FIGO classification) 3. **Assesses degeneration** — identifies red degeneration, hyaline degeneration, or cystic changes 4. **Guides treatment planning** — critical for deciding between hysteroscopic resection, myomectomy, or expectant management **High-Yield:** MRI is superior to ultrasound for: - Distinguishing fibroids from adenomyosis - Determining exact location and number of fibroids - Assessing junctional zone involvement - Detecting complications (torsion, necrosis, malignant transformation) ## FIGO Classification of Fibroids (Requires MRI) | Type | Location | Submucosal Extent | Clinical Significance | |------|----------|-------------------|----------------------| | 0 | Pedunculated, intracavitary | 100% in cavity | Hysteroscopic resection possible | | 1 | Submucosal | ≥50% intracavitary | Hysteroscopic or combined approach | | 2 | Submucosal | <50% intracavitary | Myomectomy preferred | | 3 | Intramural, abutting endometrium | — | Medical or surgical management | | 4 | Intramural, away from endometrium | — | Expectant or myomectomy | | 5 | Subserosal | — | Laparoscopic myomectomy | | 6 | Parasitic/pedunculated subserosal | — | Laparoscopic resection | | 7 | Cervical | — | Specialized approach | | 8 | Extrauterine (broad ligament, etc.) | — | Surgical planning required | **Clinical Pearl:** In a woman of reproductive age with fibroids, MRI-based FIGO classification directly determines surgical approach and fertility outcomes. Ultrasound alone cannot reliably assign FIGO type. ## Why MRI > Ultrasound for Fibroid Characterization ```mermaid flowchart TD A[Pelvic mass on ultrasound]:::outcome --> B{Fibroid vs<br/>adenomyosis?}:::decision B -->|Ultrasound unclear| C[Pelvic MRI]:::action B -->|MRI obtained| D{FIGO type?}:::decision D -->|Type 0-2| E[Hysteroscopic resection<br/>± myomectomy]:::action D -->|Type 3-4| F[Myomectomy or<br/>medical management]:::action D -->|Type 5-6| G[Laparoscopic myomectomy]:::action E --> H[Fertility preserved]:::outcome F --> I[Treatment individualized]:::outcome G --> J[Minimal morbidity]:::outcome ``` **Tip:** The phrase "assess the extent of myometrial involvement" in the stem is a red flag for **MRI** — it is the only investigation that provides layer-by-layer tissue characterization and FIGO classification. 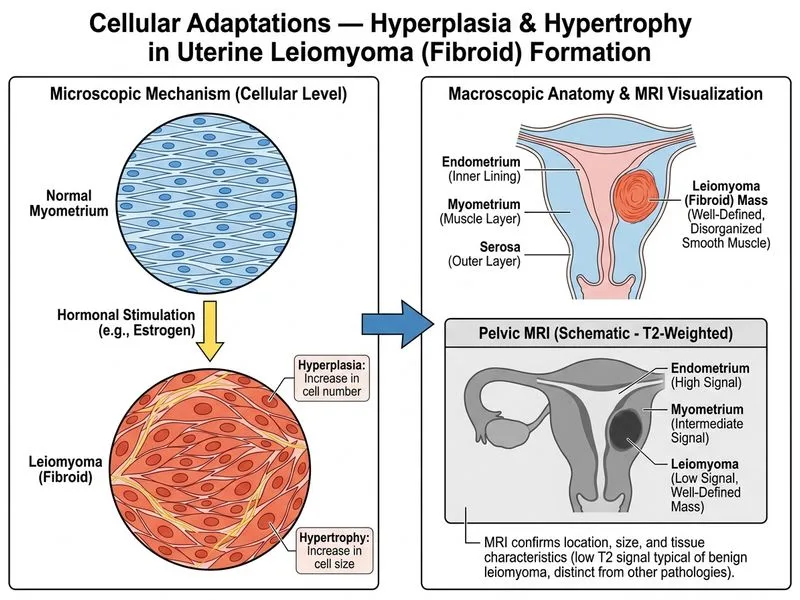
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.