## Clinical Scenario This patient presents with **diabetic cardiomyopathy** — a maladaptive form of LVH that progresses to systolic dysfunction (EF 35%) and diastolic dysfunction. The combination of chronic hyperglycemia and hypertension in diabetes causes: 1. **Myocyte hypertrophy** (adaptive response to metabolic stress) 2. **Myocardial fibrosis** (collagen deposition via AGE formation and RAAS activation) 3. **Mitochondrial dysfunction** and oxidative stress 4. **Progression to systolic heart failure** ## Pathophysiology: From Adaptation to Decompensation **Key Point:** In diabetes, LVH initially represents myocyte hypertrophy as an adaptive response to increased metabolic demand and pressure overload. However, uncontrolled hyperglycemia drives **pathological remodeling** — fibrosis, apoptosis, and impaired diastolic relaxation — converting adaptation into disease. ```mermaid flowchart TD A[Chronic Hyperglycemia + HTN]:::outcome --> B[Myocyte Hypertrophy]:::outcome B --> C[AGE Formation & RAAS Activation]:::outcome C --> D[Myocardial Fibrosis]:::outcome D --> E[Diastolic Dysfunction]:::outcome E --> F[Systolic Dysfunction]:::urgent F --> G[Heart Failure with Reduced EF]:::urgent H[Intensive Glycemic Control]:::action --> I[Slow Progression]:::action H --> J[Reduce Fibrosis]:::action ``` ## Management of Diabetic Cardiomyopathy **High-Yield:** The management triad for diabetic heart failure: | Intervention | Mechanism | Evidence | |---|---|---| | **ACE-I/ARB** | Blocks Ang II–mediated hypertrophy & fibrosis; reduces proteinuria | Reduces HF progression in diabetes | | **Beta-blocker** | Reduces HR, afterload, myocardial O₂ demand; anti-arrhythmic | Standard HFrEF therapy; cardioprotective | | **Intensive glycemic control** | Reduces AGE formation, oxidative stress, RAAS activation | Slows LVH progression and fibrosis | **Clinical Pearl:** In diabetic patients with HFrEF, insulin therapy (despite initial weight gain concerns) is often necessary to achieve tight glycemic control (target HbA1c <7%) and halt disease progression. Metformin is contraindicated if eGFR <30 mL/min. ## Why This Is the Next Step The patient has: - **Systolic dysfunction** (EF 35%) — requires ACE-I/ARB + beta-blocker per HF guidelines - **Suboptimal glycemic control** (HbA1c 9.2%) — intensification is critical to prevent further fibrosis - **No acute decompensation** — stable enough for outpatient optimization before considering advanced therapies ## Mnemonic: RAAS Blockade in Diabetic HF **RAAS** = Renin–Angiotensin–Aldosterone System - **R**eduction of hypertrophy - **A**bortion of fibrosis - **A**meliorates diastolic dysfunction - **S**lows progression to systolic failure 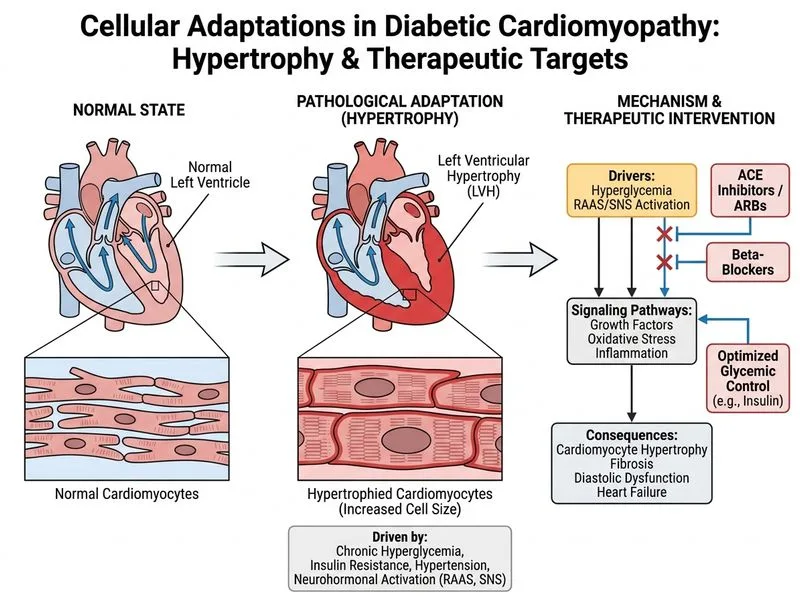
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.