## Clinical Scenario Analysis This patient presents with acute cerebellar stroke (superior cerebellar artery territory) with classic signs of cerebellar dysfunction: vertigo, dysmetria, nystagmus, and ataxia. The key clinical decision is determining the appropriate acute stroke management pathway. ## Pathophysiology of Cerebellar Infarction **Key Point:** Cerebellar infarcts carry risk of brainstem compression and obstructive hydrocephalus due to swelling, making early intervention critical. The superior cerebellar artery territory infarct affects the superior cerebellum, which can lead to significant edema within 24–72 hours. Unlike supratentorial strokes, cerebellar infarcts can cause life-threatening complications even when initially small. ## Management Algorithm for Acute Cerebellar Stroke ```mermaid flowchart TD A[Acute cerebellar stroke suspected]:::outcome --> B{Time from onset?}:::decision B -->|< 4.5 hours| C[Non-contrast CT to exclude hemorrhage]:::action B -->|4.5-24 hours| D[Consider advanced imaging: MRI/CTA]:::action C --> E{Hemorrhage present?}:::decision E -->|No| F[Eligible for IV thrombolysis]:::action E -->|Yes| G[Contraindicated for thrombolysis]:::urgent F --> H[Administer alteplase 0.9 mg/kg]:::action D --> I[Assess for edema/hydrocephalus risk]:::action I --> J[Aspirin + other antiplatelets]:::action H --> K[ICU monitoring for deterioration]:::action J --> K G --> L[Supportive care + ICU monitoring]:::action ``` **High-Yield:** The time window for IV thrombolysis in acute ischemic stroke is **4.5 hours** from symptom onset. The first step is always **non-contrast CT** to exclude hemorrhage, which is a contraindication to thrombolysis. ## Why Option 2 (CT then Thrombolysis) is Correct 1. **Exclude hemorrhage first:** Non-contrast CT is mandatory before thrombolysis to rule out intracerebral hemorrhage (ICH), which would be catastrophic if thrombolyzed. 2. **Within thrombolysis window:** At presentation (acute onset), the patient is likely within 4.5 hours, making him a candidate for IV thrombolysis if CT is negative. 3. **Standard acute stroke protocol:** This follows the American Heart Association / American Stroke Association (AHA/ASA) guideline for acute ischemic stroke management. 4. **Prevents complications:** Early reperfusion therapy reduces risk of edema and hydrocephalus in cerebellar infarcts. ## Clinical Pearl **Clinical Pearl:** Cerebellar infarcts can deteriorate rapidly (hours 2–3) due to brain edema compressing the brainstem and fourth ventricle. Early thrombolysis or thrombectomy (if large vessel occlusion) can prevent this catastrophic progression. ## Comparison of Distractors | Option | Why Incorrect | Mechanism | |--------|---------------|----------| | Aspirin alone without thrombolysis | Suboptimal acute therapy | Aspirin is secondary prevention; thrombolysis is superior in acute window | | Neurosurgical decompression first | Premature intervention | Surgery is reserved for failed medical management or acute deterioration | | High-dose steroids as primary therapy | Not evidence-based for acute stroke | Steroids are not indicated for acute ischemic stroke; may worsen outcome | **Warning:** Do not confuse acute cerebellar infarction management with chronic cerebellar atrophy or degenerative disease — acute infarcts require emergent reperfusion therapy. 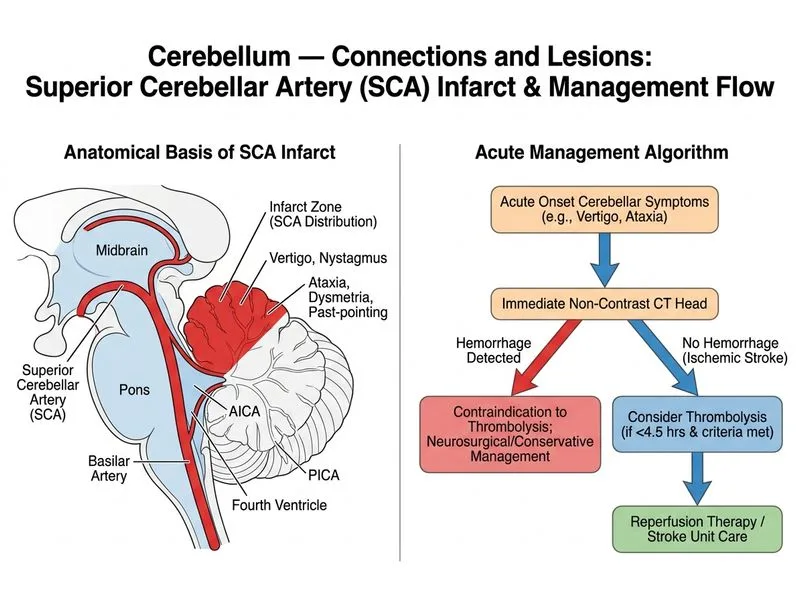
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.