## Distinguishing CIN 3 from Invasive Cervical Cancer ### Histopathological Basis **Key Point:** The defining feature that separates CIN 3 (a preinvasive lesion) from invasive squamous cell carcinoma (SCC) is the **integrity of the basement membrane**. CIN 3 shows full-thickness dysplasia but the basement membrane remains intact; invasive SCC shows breach and invasion beyond the basement membrane into the underlying stroma. ### Comparative Histology | Feature | CIN 3 | Invasive SCC | |---------|-------|-------------| | **Basement membrane** | Intact, preserved | Breached and disrupted | | **Invasion pattern** | Confined to epithelium | Infiltrates stroma | | **Stromal response** | None | Desmoplasia, inflammation | | **Depth of involvement** | Full thickness epithelium only | Beyond epithelium | | **Nuclear atypia** | Present | Present | | **Mitoses** | Increased, abnormal | Increased, abnormal | ### Why Other Features Are Not Discriminatory **High-Yield:** Nuclear enlargement, increased mitotic activity, and keratinization abnormalities are present in **both** CIN 3 and invasive SCC—they reflect dysplasia but do not distinguish preinvasive from invasive disease. **Clinical Pearl:** Koilocytes (HPV-infected cells with perinuclear halos) are seen in CIN 1 and CIN 2, but may be sparse or absent in high-grade CIN 3, so their presence is not a reliable discriminator. ### Clinical Significance **Key Point:** This distinction is critical because CIN 3 is curable by excisional procedures (loop electrosurgical excision procedure [LEEP], cold knife conization) with high success rates, whereas invasive SCC requires radical hysterectomy, radiation, or chemoradiation depending on stage and grade. [cite:Robbins 10e Ch 22] 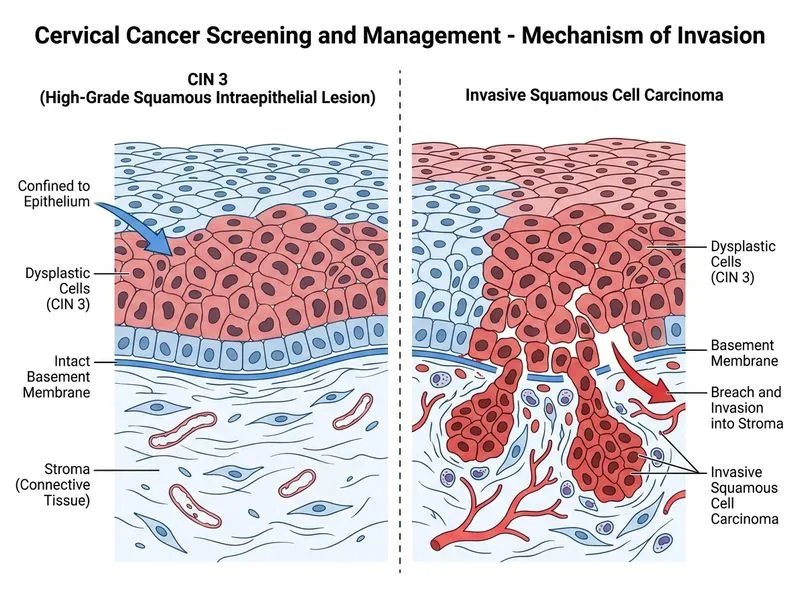
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.