## Clinical Scenario Analysis The patient presents with clinical signs highly suggestive of invasive cervical cancer: a visible cervical mass, post-coital bleeding, and cytology showing HSIL. The presence of a **grossly visible lesion** mandates tissue diagnosis. ## Next Step Rationale **Key Point:** When a cervical mass is **clinically visible** (not just cytologically abnormal), cervical biopsy is the standard of care to confirm invasive disease and grade the malignancy. **High-Yield:** The diagnostic algorithm differs based on presentation: - **Visible cervical lesion** → Direct cervical biopsy (bypass colposcopy) - **No visible lesion, abnormal cytology** → Colposcopy with directed biopsy - **No visible lesion, normal cytology** → Observation or repeat cytology ## Why Cervical Biopsy? 1. **Confirms invasiveness:** Distinguishes CIN from invasive squamous cell carcinoma 2. **Grades the tumor:** Determines differentiation (well/moderately/poorly differentiated) 3. **Guides staging:** Histology is required before MRI/CT staging can be interpreted 4. **Immediate action:** No delay in diagnosis when malignancy is clinically suspected **Clinical Pearl:** A friable, bleeding cervical mass with HSIL cytology has >95% likelihood of invasive cancer. Biopsy confirmation is mandatory before staging investigations. ## Staging Sequence (After Biopsy) ```mermaid flowchart TD A[Visible cervical mass + HSIL]:::outcome --> B[Cervical biopsy]:::action B --> C{Histology confirms<br/>invasive cancer?}:::decision C -->|Yes| D[MRI pelvis ± CT chest/abdomen]:::action C -->|No| E[Reassess diagnosis]:::outcome D --> F[FIGO staging]:::outcome F --> G[Treatment planning]:::action ``` [cite:FIGO Cervical Cancer Guidelines 2019] 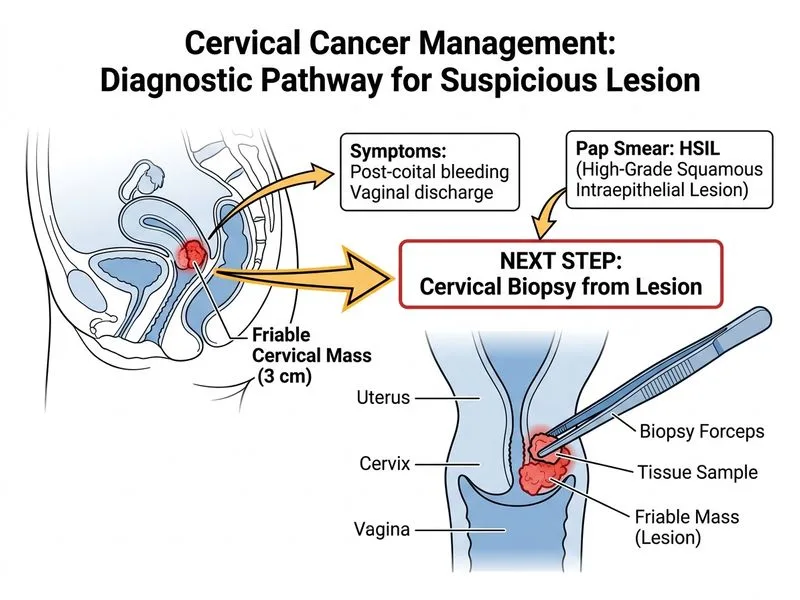
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.