## T2-Hyperintensity in Cervical Spondylotic Myelopathy ### Pathophysiology of Signal Changes **Key Point:** T2-hyperintensity on MRI in cervical spondylotic myelopathy (CSM) represents a spectrum of cord pathology, ranging from reversible edema to irreversible myelomalacia. The presence and nature of T2-signal abnormality is a critical prognostic indicator: | Feature | Reversibility | Prognosis | Pathology | |---------|---------------|-----------|----------| | **Transient T2 edema** | Yes | Good | Cytotoxic edema, inflammation | | **Myelomalacia (cavitation)** | No | Poor | Gliosis, axonal loss, necrosis | | **Cord atrophy** | No | Very poor | Chronic degeneration | ### Why Myelomalacia Predicts Poor Outcome 1. **Chronic Ischemic Injury**: Myelomalacia reflects chronic spinal cord ischemia from: - Sustained compression reducing microcirculatory perfusion - Oxidative stress and free radical accumulation - Loss of gray matter neurons and white matter tracts 2. **Irreversible Neuronal Damage**: Unlike edema, myelomalacia involves: - Cystic necrosis and cavitation - Gliosis (astrocytic replacement of lost neurons) - Permanent axonal degeneration 3. **Surgical Limitation**: Even after successful decompression, myelomalacia does not recover because: - Dead neurons cannot regenerate in the adult spinal cord - Gliotic scar tissue prevents functional reorganization - Published series show <30% functional improvement vs. >60% with edema alone ### Clinical Correlation **High-Yield:** Patients with myelomalacia have: - Longer symptom duration (typically >18 months) - Greater baseline neurological deficit - Slower and incomplete recovery post-decompression - Higher risk of post-operative deterioration **Clinical Pearl:** The presence of cord atrophy in addition to myelomalacia is an even worse prognostic sign, indicating end-stage cord damage. ### Why Other Options Are Wrong **Option 0 (Reversible cord edema):** While edema is T2-hyperintense and reversible, it does NOT represent the poorest prognosis. Edema alone has excellent recovery potential (60–80% improvement) after decompression. The question specifically asks what predicts the POOREST prognosis. **Option 2 (Acute demyelination):** Demyelination (as in MS or transverse myelitis) would present with acute symptom onset and inflammatory CSF findings. CSM is a chronic compressive process, not inflammatory demyelination. Demyelination is also potentially reversible with immunotherapy. **Option 3 (Venous congestion):** Transient signal changes from venous stasis are not permanent findings on standard MRI. This does not explain persistent T2-hyperintensity or poor prognosis. Venous congestion is a mechanism of injury but not a specific pathological diagnosis. ## Summary Myelomalacia—cavitary necrosis with gliosis—represents irreversible cord damage and is the single most powerful negative prognostic factor in CSM. Its presence should prompt urgent surgical decompression to prevent further deterioration, but expectations for functional recovery must be tempered. [cite:Harrison 21e Ch 380] 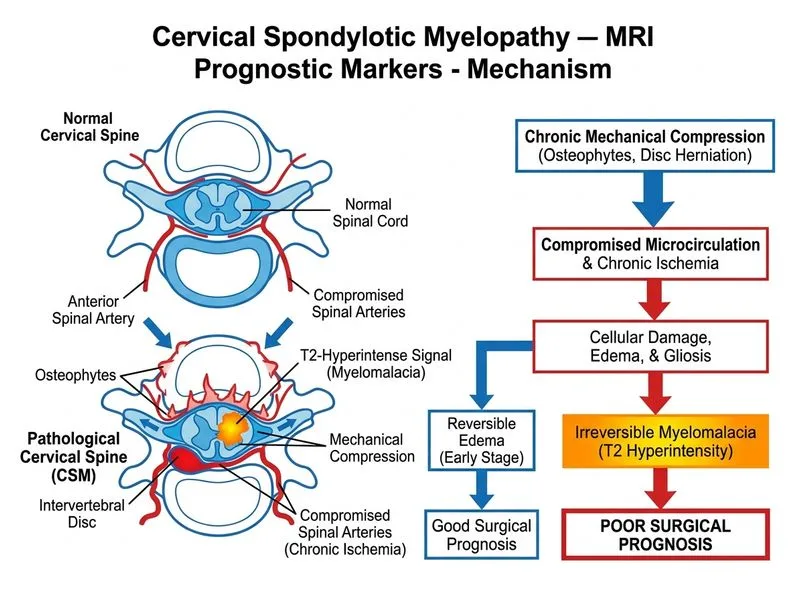
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.