## Diagnosis: Placenta Previa (Major) with Active Bleeding ### Classification of Placenta Previa | Type | Definition | Risk of Vaginal Delivery | | --- | --- | --- | | **Complete/Total** | Placenta completely covers internal os | Absolute contraindication to vaginal delivery | | **Partial** | Placenta partially covers internal os | Absolute contraindication to vaginal delivery | | **Marginal** | Placental edge within 2 cm of internal os | Relative contraindication; vaginal delivery may be considered | | **Low-lying** | Placental edge >2 cm from internal os | Vaginal delivery usually safe | **Key Point:** This patient has **major placenta previa** (2 cm of placental tissue over the os = partial previa), which is an **absolute contraindication to vaginal delivery**. ### Clinical Presentation & Risk Factors **High-Yield:** Placenta previa presents with: - Painless vaginal bleeding (most common) - Bleeding may be recurrent and unpredictable - Risk increases with multiparity, advanced maternal age, prior cesarean, smoking, cocaine use, IVF **Clinical Pearl:** This patient is a G2P1 (multipara), which increases previa risk. The presence of **active bleeding at term** with **major previa** mandates immediate cesarean delivery. ### Management Algorithm ```mermaid flowchart TD A[Vaginal bleeding at 3rd trimester]:::outcome --> B{Placenta previa on ultrasound?}:::decision B -->|No previa| C[Rule out other causes]:::action B -->|Yes| D{Type of previa?}:::decision D -->|Low-lying or marginal| E{Active bleeding?}:::decision D -->|Partial or complete| F[Absolute contraindication to vaginal delivery]:::urgent E -->|No| G[Admit for observation, strict pelvic rest]:::action E -->|Yes| H[Cesarean section]:::action F --> I{Gestational age ≥37 weeks?}:::decision I -->|Yes| H I -->|No| J[Admit, corticosteroids if <34 weeks, plan CS at 37 weeks]:::action ``` ### Why Immediate Cesarean Section? 1. **Major Placenta Previa:** Partial or complete previa is an absolute contraindication to vaginal delivery. Cervical dilation or descent of the fetal head will cause massive placental hemorrhage. 2. **Active Bleeding at Term:** The patient is at 38 weeks with active vaginal bleeding. Cesarean delivery should be performed urgently to prevent maternal hemorrhage and fetal compromise. 3. **Maternal Hemodynamics Stable (for now):** Although BP and HR are currently stable, placenta previa can lead to rapid, life-threatening hemorrhage. Delaying delivery increases this risk. **Key Point:** ~~Vaginal delivery with placenta previa~~ is never safe. Even marginal previa requires careful assessment; major previa mandates cesarean. ### Why Not the Other Options? - **Observation with planned vaginal delivery:** Major placenta previa is an absolute contraindication to vaginal delivery. Attempting labour will cause catastrophic hemorrhage from placental separation. - **Amniotomy:** This is contraindicated in placenta previa. Rupturing membranes will not help assess fetal blood and may precipitate massive bleeding. - **Discharge home:** Active bleeding with major previa at term is a medical emergency. Discharge is unsafe and risks maternal hemorrhage and fetal loss. ### Timing & Preparation **High-Yield:** Cesarean section for placenta previa at term should be: - Performed urgently (within 30 minutes if active bleeding) - With blood products available (cross-matched RBC, FFP, platelets) - With anesthesia and neonatology on standby - Preferably under spinal anesthesia (if hemodynamically stable) to avoid general anesthesia risks **Clinical Pearl:** Placenta previa increases risk of: - Massive postpartum hemorrhage (PPH) - Placenta accreta (especially if prior cesarean) - Maternal transfusion requirement - Fetal prematurity (if delivery before 37 weeks) [cite:ACOG Practice Bulletin 208, RCOG Green-top Guideline 27] 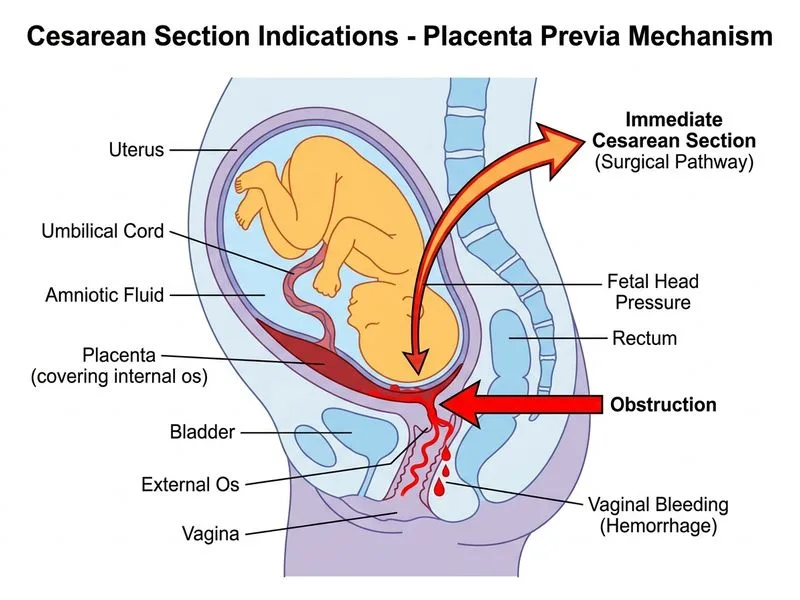
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.