## Distinguishing Cephalopelvic Disproportion from Uterine Inertia ### Key Clinical Discriminator **Key Point:** Molding of the fetal skull and caput succedaneum *despite adequate uterine contractions* indicate that the fetus is being pushed against an insurmountable mechanical obstacle (CPD), not a contractility problem. ### Comparative Table | Feature | Cephalopelvic Disproportion (CPD) | Uterine Inertia | |---------|-----------------------------------|------------------| | **Uterine contractions** | Strong, adequate, regular | Weak, infrequent, or absent | | **Molding & caput** | Present (fetus compressed against pelvis) | Absent or minimal | | **Cervical dilation progress** | Arrested despite good contractions | Slow or absent; improves with augmentation | | **Fetal descent** | Minimal or absent | Minimal; improves with oxytocin | | **Response to oxytocin** | No improvement (mechanical obstruction) | Improves with augmentation | | **Maternal effort** | Exhausted (pushing against resistance) | Variable | | **Fetal distress** | Common (prolonged compression) | Variable | ### Clinical Pearl **Clinical Pearl:** The presence of **molding and caput succedaneum with adequate uterine contractions** is the pathognomonic sign of CPD. These findings indicate that the uterus is contracting normally but the fetus cannot descend because the pelvis is too small or the fetal head is too large. In contrast, uterine inertia shows weak contractions with minimal molding; augmentation with oxytocin typically improves progress. ### High-Yield Distinction **High-Yield:** **Molding + adequate contractions = CPD (cesarean section). Weak contractions + no molding = inertia (trial of augmentation).** This is the single most important discriminator in labor management. ### Pathophysiology **Cephalopelvic Disproportion:** 1. Mechanical mismatch between fetal head and maternal pelvis 2. Strong uterine contractions push fetus against pelvic bones 3. Fetal skull bones compress and overlap (molding) 4. Caput succedaneum forms from localized edema 5. No progress despite adequate contractions → cesarean delivery **Uterine Inertia:** 1. Inadequate myometrial contractility 2. Weak or infrequent contractions 3. Minimal fetal compression → no molding 4. Responds to oxytocin augmentation 5. Vaginal delivery often possible after augmentation 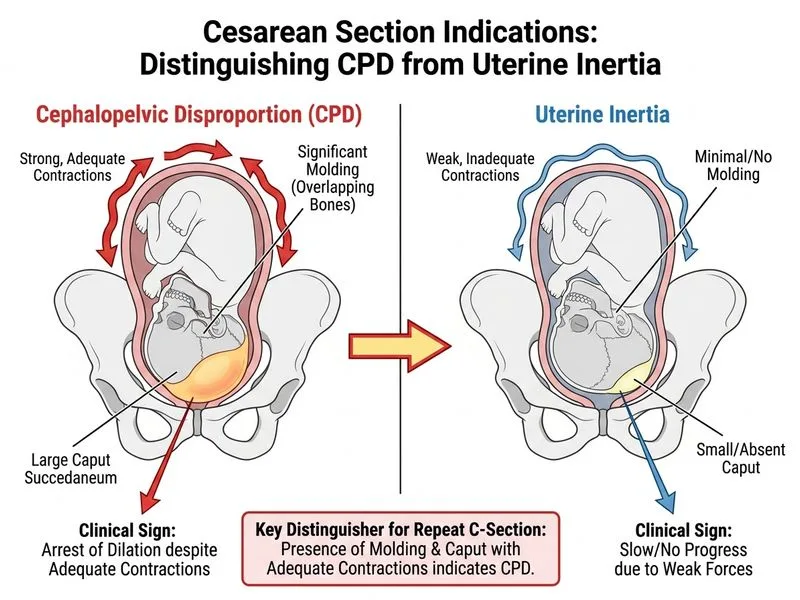
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.