## Prognostic Assessment in Chemical Eye Injury ### Why Limbal Ischemia Assessment is Correct **High-Yield:** The extent of limbal stem cell damage (assessed by vital dye staining and slit-lamp examination) is the **single most important prognostic indicator** in chemical eye injury. Limbal ischemia predicts: - Risk of symblepharon and anterior synechiae - Corneal scarring and opacity - Neovascularization - Long-term visual prognosis **Key Point:** Roper Hall classification (the gold standard prognostic system for chemical injuries) is based on: 1. **Corneal clarity** (epithelial loss, stromal haze) 2. **Limbal involvement** (percentage of limbal circumference with ischemia) 3. **Conjunctival involvement** (conjunctival epithelial loss) **Mnemonic: LICE** — **L**imbal ischemia, **I**njury extent, **C**orneal clarity, **E**xtent of conjunctival loss (prognostic factors in order of importance) ### Clinical Assessment of Limbal Ischemia Limbal ischemia is detected by: - **Lissamine green or rose bengal staining** — vital dyes highlight devitalized limbal epithelium - **Slit-lamp biomicroscopy** — direct visualization of blanching, loss of limbal vessels, and epithelial loss - **Percentage of limbal circumference affected** — >50% ischemia = poor prognosis **Clinical Pearl:** Limbal stem cells reside in the basal epithelium of the limbus. Alkaline injuries (ammonia, lime) penetrate deeper and cause more limbal damage than acidic injuries (HCl). However, HCl can still cause significant limbal ischemia depending on concentration and exposure time. ### Roper Hall Classification (Prognostic Staging) | Grade | Corneal Clarity | Limbal Ischemia | Conjunctival Loss | Prognosis | |---|---|---|---|---| | **I** | Clear | 0% | 0% | Excellent | | **II** | Hazy, iris visible | <1/3 | <1/3 | Good | | **III** | Opaque, iris obscured | 1/3–1/2 | 1/3–1/2 | Guarded | | **IV** | Opaque, iris not visible | >1/2 | >1/2 | Poor | This patient's white, opaque cornea with stromal haze suggests Grade III–IV injury; limbal ischemia assessment will determine whether aggressive anti-inflammatory and stem cell–sparing therapy is warranted. ### Why Other Investigations Are Suboptimal **Specular microscopy** measures endothelial cell count and morphology—relevant for assessing corneal decompensation risk, but does NOT predict symblepharon or anterior synechiae (which depend on limbal and conjunctival damage, not endothelial function). **Ultrasound B-scan** images the posterior segment and is used to rule out globe rupture or retinal detachment, not to assess anterior segment prognosis. **Corneal topography and keratometry** measure corneal curvature and astigmatism—useful for refractive planning in healed cases, not for acute prognostic assessment. [cite:Kanski's Clinical Ophthalmology 9e Ch 5; Roper Hall classification] 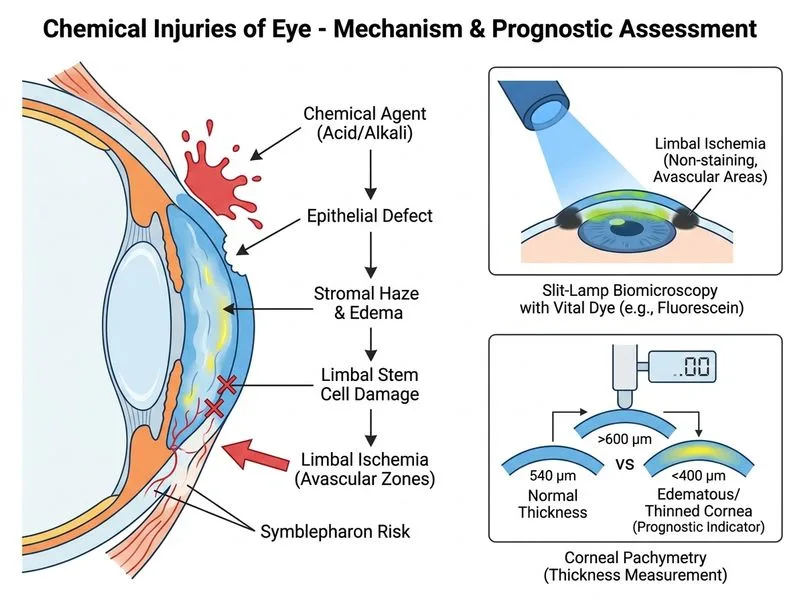
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.