## Diagnosis: B-cell Precursor ALL (BCP-ALL) with t(12;21) TEL-AML1 Fusion ### Clinical & Immunophenotypic Profile The vignette describes a 5-year-old with: - **Age:** Peak incidence for childhood ALL (2–5 years) - **Presentation:** Insidious onset over 2 months (typical for ALL, not AML) - **Organomegaly:** Lymphadenopathy, hepatomegaly, splenomegaly (common in ALL) - **Immunophenotype:** CD19+ (B-cell marker), CD10+ (common ALL antigen, CALLA), TdT+ (terminal deoxynucleotidyl transferase — marker of lymphoid precursors) **Key Point:** CD19+ CD10+ TdT+ blasts define **Common B-cell Precursor ALL (BCP-ALL)**, which accounts for ~80% of childhood ALL. This is the most favorable immunophenotypic subtype. ### Cytogenetic Abnormalities in Childhood ALL — Prognostic Hierarchy | Cytogenetic Finding | Frequency | Prognosis | 5-yr EFS | |---|---|---|---| | **t(12;21) TEL-AML1** | 20–25% of BCP-ALL | **Excellent** | **85–90%** | | **Hyperdiploidy (>50 chr)** | 25–30% of BCP-ALL | Excellent | 80–85% | | **Hypodiploidy (<45 chr)** | 1–2% | Poor | <30% | | **t(9;22) Ph+ (BCR-ABL)** | 3–5% of childhood ALL | Poor | 40–50% (improved with TKI) | | **t(4;11) MLL-AF4** | 2–3% of BCP-ALL | Poor | <40% | | **Complex karyotype** | 5–10% | Poor | <30% | **High-Yield:** t(12;21) TEL-AML1 fusion is the **single most favorable cytogenetic abnormality** in childhood ALL and is associated with excellent long-term survival (>85%) with standard chemotherapy. It is found in ~20–25% of BCP-ALL cases. ### Why t(12;21) TEL-AML1 is Favorable 1. **Chemotherapy sensitivity:** Blasts with this fusion are highly responsive to standard multi-agent chemotherapy 2. **Low relapse rate:** Even with standard-intensity therapy, relapse rates are <10–15% 3. **Age & immunophenotype synergy:** When combined with CD10+ BCP-ALL in a 5-year-old, outcomes are optimal 4. **Molecular mechanism:** The TEL-AML1 fusion disrupts normal transcriptional regulation but does not confer the aggressive proliferative advantage seen in other fusions (e.g., BCR-ABL, MLL) **Clinical Pearl:** The presence of t(12;21) may allow de-escalation of therapy in some protocols, reducing long-term toxicity while maintaining cure rates. ### Why Other Cytogenetic Abnormalities Are Inferior **t(9;22) Philadelphia Chromosome (BCR-ABL):** - Accounts for 3–5% of childhood ALL - Associated with poor prognosis (5-yr EFS ~40–50% historically) - Now improved with tyrosine kinase inhibitors (imatinib, dasatinib) combined with chemotherapy - Still considered high-risk **t(4;11) MLL Rearrangement:** - Accounts for 2–3% of BCP-ALL - Associated with poor prognosis (5-yr EFS <40%) - Often presents with high WBC, CNS involvement, and early relapse - Requires intensive chemotherapy and often allogeneic HSCT **Complex Karyotype (≥3 abnormalities):** - Indicates genomic instability - Associated with poor prognosis (5-yr EFS <30%) - Requires high-intensity therapy ### Next Steps in Management 1. **Confirm t(12;21)** via FISH or RT-PCR (more sensitive than conventional karyotyping) 2. **Risk stratification:** This patient is **Standard Risk** (age 1–9 years, WBC <50,000, t(12;21) present) 3. **Treatment:** Standard-intensity multi-agent chemotherapy (CCLSG, COG, or UKALL protocol) 4. **Prognosis:** Expected 5-year EFS >85% with appropriate therapy [cite:Robbins 10e Ch 13; Harrison 21e Ch 110] 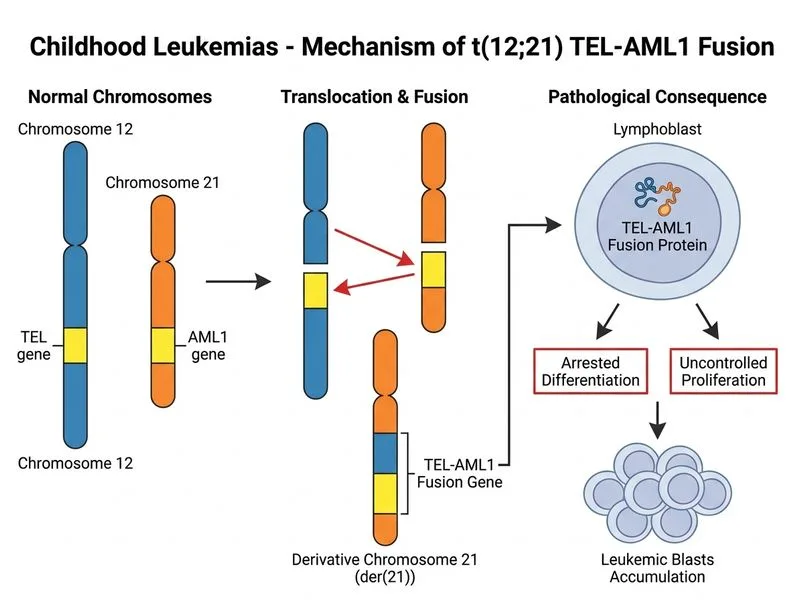
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.