## Prognostic Stratification in Childhood ALL **Key Point:** Cytogenetic analysis and molecular studies, including detection of specific translocations and minimal residual disease (MRD), are the most powerful prognostic tools in childhood ALL and directly guide treatment intensification. ### Prognostic Factors in Childhood ALL **High-Yield:** Modern ALL risk stratification integrates: 1. **Cytogenetic abnormalities** — most powerful prognostic markers 2. **Molecular markers** — MRD detection 3. **Clinical features** — age, WBC count, CNS involvement 4. **Early response to therapy** — day 14 marrow response (secondary) ### Key Cytogenetic and Molecular Abnormalities | Abnormality | Prognosis | Frequency | Clinical Significance | |-------------|-----------|-----------|----------------------| | t(9;22) BCR-ABL (Philadelphia chromosome) | Very poor | 3–5% | Requires TKI + chemotherapy | | t(4;11) MLL-AF4 | Very poor | 5–10% (infants) | Requires intensive therapy | | Hyperdiploidy (>50 chromosomes) | Favorable | 25–30% | Standard risk therapy may suffice | | Normal karyotype | Intermediate | 40% | Depends on MRD status | | t(12;21) ETV6-RUNX1 | Favorable | 20–25% | Standard risk therapy | **Mnemonic: BCMH** — **B**CR-ABL (poor), **C**ytogenetics (essential), **M**RD (predicts relapse), **H**yperdiploidy (favorable). ### Minimal Residual Disease (MRD) **Clinical Pearl:** MRD assessment by flow cytometry or PCR at end of induction (day 28–35) is the single most powerful predictor of relapse risk in ALL: - **MRD negative** (<0.01%) — excellent prognosis, standard therapy often sufficient - **MRD positive** (≥0.01%) — high relapse risk, requires therapy intensification (escalated chemotherapy, stem cell transplantation consideration) **Warning:** MRD positivity overrides favorable cytogenetics; even children with t(12;21) and MRD positivity require intensified therapy. ### Why Other Investigations Are Secondary ```mermaid flowchart TD A[Newly diagnosed ALL]:::outcome --> B[Cytogenetics + Molecular Studies]:::action B --> C{Philadelphia chromosome<br/>or t4;11?}:::decision C -->|Yes| D[Very high risk:<br/>TKI + intensive chemo]:::urgent C -->|No| E[Assess MRD at day 28]:::action E --> F{MRD positive?}:::decision F -->|Yes| G[High risk:<br/>Intensify therapy/<br/>Consider SCT]:::urgent F -->|No| H[Standard risk:<br/>Continue standard protocol]:::action I[Day 14 marrow response<br/>is supportive only] -.-> E ``` - **Day 14 marrow response:** Historically used but now considered secondary; MRD at day 28–35 is more predictive. - **Immunophenotyping alone:** Identifies lineage but does not provide cytogenetic/molecular prognostic data. - **Lumbar puncture:** Essential for CNS prophylaxis but does NOT determine long-term prognosis or guide chemotherapy intensification. **High-Yield:** The 2016 COG (Children's Oncology Group) and modern European protocols mandate cytogenetic and molecular analysis (including MRD) for all newly diagnosed ALL to assign risk group and determine therapy intensity. [cite:Park 26e Ch 10] 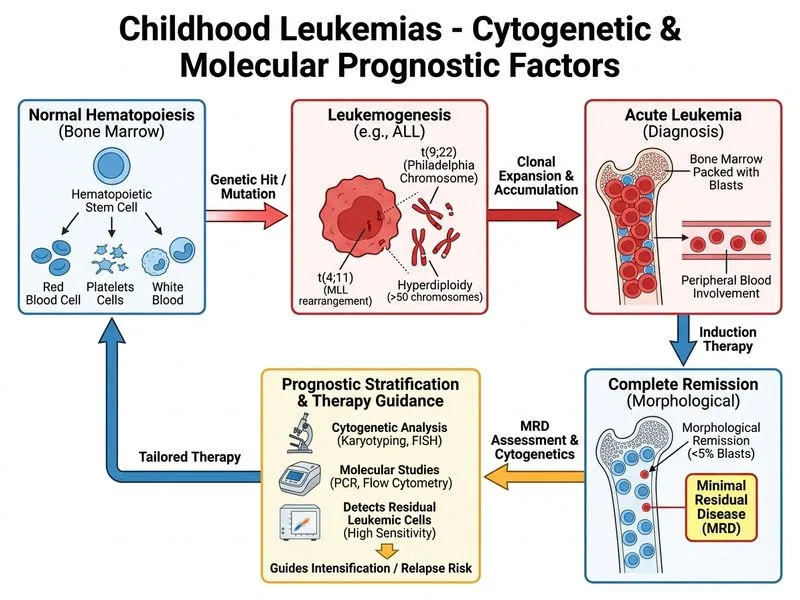
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.