## Investigation of Choice for Cholesteatoma Diagnosis and Staging **Key Point:** HRCT temporal bone is the **first-line investigation** for confirming cholesteatoma and assessing its extent, ossicular involvement, and complications prior to surgery. ### Why HRCT Temporal Bone is the Correct Answer 1. **Structural/Bony Detail**: Provides unparalleled resolution of bony anatomy — demonstrating scutum erosion, ossicular chain destruction, tegmental defects, and labyrinthine involvement. 2. **Preoperative Planning**: Mandatory before any tympanomastoid surgery; guides surgical approach and identifies critical anatomical variants (e.g., high jugular bulb, dehiscent facial canal). 3. **Complication Detection**: Identifies erosion of the facial canal, lateral semicircular canal, tegmen tympani, and sigmoid plate. 4. **Availability & Cost**: Widely available, fast, and far less expensive than MRI — making it the practical first-line choice in most centres. ### Why MRI-DWI is NOT the First-Line Investigation Although MRI with diffusion-weighted imaging (DWI) has very high sensitivity and specificity (~95–100%) for cholesteatoma tissue, it is **not** the investigation of choice for initial diagnosis because: - It provides **poor bony detail** — cannot adequately assess ossicular erosion or bony complications. - It is **more expensive, less available**, and more time-consuming than HRCT. - Its primary role is **postoperative surveillance** — detecting residual or recurrent cholesteatoma (especially in the context of canal-wall-up mastoidectomy) without exposing the patient to radiation. > *Scott-Brown's Otorhinolaryngology* and *Dhingra's Diseases of Ear, Nose and Throat* both designate HRCT temporal bone as the gold-standard preoperative imaging for cholesteatoma. ### Clinical Diagnosis vs. Imaging **Clinical Pearl:** The diagnosis of cholesteatoma is often made clinically — a retraction pocket in the posterosuperior quadrant (pars flaccida or pars tensa) with foul-smelling otorrhoea is virtually pathognomonic. However, **HRCT is mandatory for preoperative planning** to define extent, identify complications, and guide surgical strategy. Imaging alone cannot replace clinical assessment. ### Comparison of Investigations | Investigation | Role | Limitation | |---|---|---| | **HRCT Temporal Bone** | First-line; bony erosion, extent, preoperative planning | Cannot reliably differentiate cholesteatoma from granulation tissue on soft-tissue windows alone | | **MRI DWI** | Postoperative surveillance for residual/recurrent disease | Poor bony detail; not first-line for initial diagnosis | | **Otoacoustic Emissions** | Cochlear function screening | Cannot visualize or diagnose cholesteatoma | | **Tympanometry** | Middle ear pressure/compliance assessment | Non-specific; cannot diagnose cholesteatoma | **High-Yield:** The combination of **clinical presentation** (foul-smelling otorrhoea + posterosuperior retraction pocket) + **HRCT findings** (scutum erosion, ossicular erosion, soft-tissue mass in epitympanum/mastoid) = definitive workup for cholesteatoma. **Warning:** ~~Tympanometry~~ and ~~otoacoustic emissions~~ are functional tests — they cannot diagnose cholesteatoma. MRI-DWI, while highly sensitive, is reserved for detecting **residual/recurrent** disease postoperatively, not for initial diagnosis. 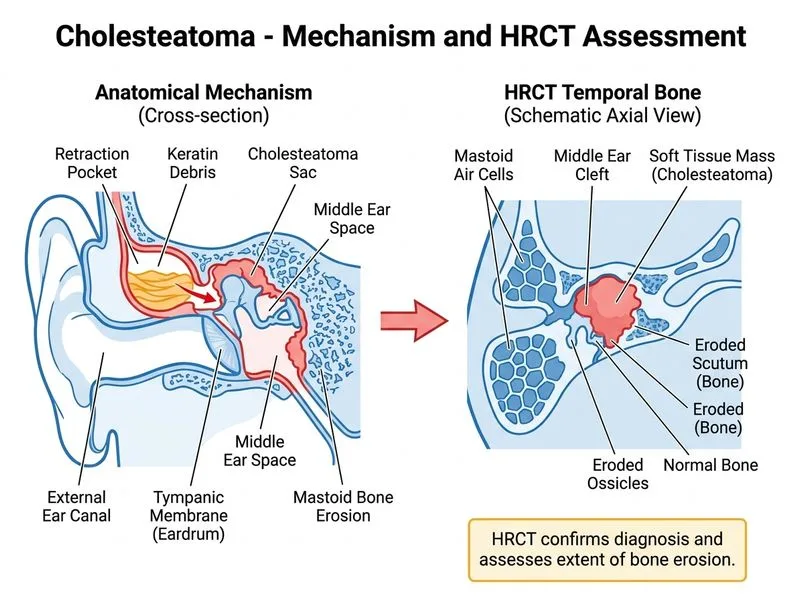
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.