## Clinical Scenario Analysis This patient has **residual cholesteatoma** (disease remaining after initial surgery) with: - Persistent discharge at 18 months post-CWU - New sensorineural hearing loss (high-frequency) — suggests labyrinthine involvement - Imaging confirmation of disease in sinus tympani (notoriously difficult location in CWU approach) ## Residual vs Recurrent Disease | Feature | Residual | Recurrent | | --- | --- | --- | | **Timing** | Within 6–12 months | >12 months post-op | | **Cause** | Incomplete disease removal at first surgery | Retraction pocket reformation | | **Incidence after CWU** | 10–40% | 5–15% | | **Management** | Revision surgery (CWD preferred) | CWU revision or CWD | **Key Point:** Residual disease in sinus tympani is a **known failure point of CWU surgery**. The sinus tympani is difficult to access via canal wall-preserving techniques and is a common site of disease recurrence. ## Why CWD Conversion Is Correct **High-Yield:** Once residual disease is documented (especially in a difficult location like sinus tympani), the **standard of care is conversion to CWD**. Reasons: 1. **Sinus tympani is inaccessible** via standard CWU approach — even endoscopic assistance has limited efficacy here 2. **New SNHL** indicates labyrinthine erosion — risk of further progression 3. **CWD eliminates disease source** and prevents recurrence (>95% disease control) 4. **Patient already has canal abnormality risk** from first surgery; CWD does not add significant morbidity **Clinical Pearl:** The sinus tympani is the **"Achilles heel" of CWU surgery** — located deep in the anterior epitympanum, it is the most common site of residual disease. Endoscopic-assisted CWU may reduce but does not eliminate this risk. **Mnemonic: SINUS** — **S**inus tympani **I**naccessible → **N**eed **U**pgrade to **S**urgical (CWD) approach. 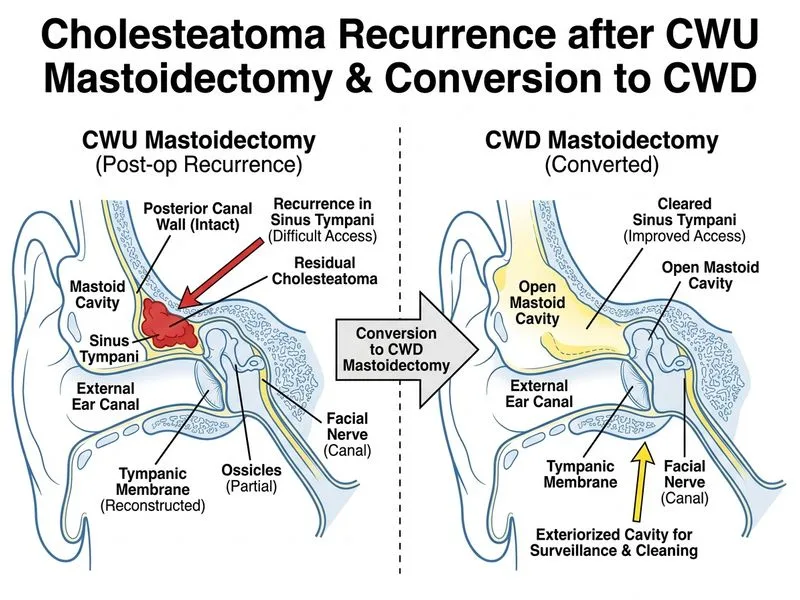
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.