## Diagnostic Approach to Chronic Myeloid Leukemia ### Why BCR-ABL1 Detection is the Gold Standard **Key Point:** Philadelphia chromosome (t(9;22)) and its molecular correlate BCR-ABL1 fusion gene are pathognomonic for CML and mandatory for diagnosis. **High-Yield:** BCR-ABL1 can be detected by: - Conventional cytogenetics (karyotype) — Philadelphia chromosome in >95% of CML cases - Fluorescence in situ hybridization (FISH) — faster, more sensitive - Reverse transcription PCR (RT-PCR) — most sensitive; quantifies transcript levels for monitoring ### Diagnostic Hierarchy for CML | Investigation | Role | Sensitivity | Timing | |---|---|---|---| | Peripheral smear + CBC | Initial screening | Low | Immediate | | Bone marrow aspirate/biopsy | Morphology assessment | Moderate | Confirmatory | | **BCR-ABL1 (cytogenetics/FISH/RT-PCR)** | **Definitive diagnosis** | **>95%** | **Gold standard** | | Cytochemistry (MPO, PAS) | Lineage confirmation | Moderate | Supportive only | | Flow cytometry | Rule out blast crisis | Moderate | Staging | **Clinical Pearl:** The presence of BCR-ABL1 is required to diagnose CML per WHO 2016 criteria. Without it, the diagnosis is "chronic myeloid neoplasm, not otherwise specified" — a fundamentally different entity with different prognosis and treatment. ### Why Other Tests Are Insufficient 1. **Cytochemistry (MPO, PAS):** Confirms myeloid lineage but is non-specific; does not distinguish CML from other myeloproliferative disorders or reactive leukemoid reactions. 2. **Flow cytometry:** Useful for detecting immature blasts and assessing for blast crisis, but cannot identify the BCR-ABL1 fusion. 3. **Biochemical markers (LDH, uric acid):** Reflect disease burden and tumor lysis risk but are non-specific and not diagnostic. **Mnemonic:** **FISH for BCR** — FISH (or cytogenetics/RT-PCR) to catch the BCR-ABL1 fusion in CML. 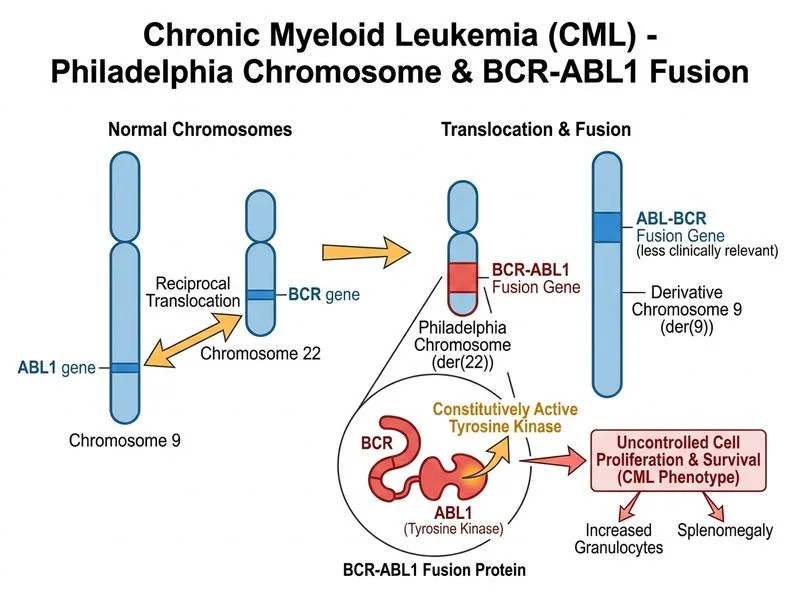
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.