## Cholesteatoma with Secondary Ossicular Damage: Diagnosis ### Clinical Features Supporting Cholesteatoma | Feature | This Patient | Significance | |---------|-------------|--------------| | **Perforation site** | Posterosuperior marginal | Classic for cholesteatoma (attic/posterosuperior retraction) | | **Discharge** | Foul-smelling, purulent | Keratin debris + anaerobic colonization | | **Granulation tissue** | Present in EAC | Chronic inflammatory response to cholesteatoma | | **Ossicular erosion** | CT confirmed | Hallmark of cholesteatoma's enzymatic bone destruction | | **Hearing loss** | Mixed (AC gap 40 dB, BC 35 dB) | Conductive from ossicular erosion + sensorineural from labyrinthine involvement | | **Duration** | 3 years progressive | Consistent with slowly expanding cholesteatoma | ### Why Cholesteatoma Is the Correct Diagnosis **High-Yield:** The clinical triad of **(1) posterosuperior marginal perforation, (2) foul-smelling discharge with granulation tissue, and (3) CT-confirmed ossicular chain erosion** is the textbook presentation of **acquired cholesteatoma** (Scott-Brown's Otorhinolaryngology 8e; Dhingra ENT 8e Ch 11). Cholesteatoma is defined as keratinizing stratified squamous epithelium that migrates into the middle ear/mastoid through a marginal perforation or retraction pocket. Its hallmarks are: - **Marginal (especially posterosuperior/attic) perforation** — the entry point for squamous epithelium - **Enzymatic bone erosion** (collagenases, osteoclast activation) — explains the CT finding of ossicular chain erosion - **Foul-smelling discharge** — from keratin debris undergoing anaerobic decomposition - **Granulation tissue** — chronic inflammatory response surrounding the cholesteatoma sac **Clinical Pearl:** In ENT practice, a posterosuperior marginal perforation with foul-smelling discharge and CT ossicular erosion is considered cholesteatoma until proven otherwise. The "osteitis" of atticoantral CSOM is, in the vast majority of cases, driven by cholesteatoma. Dhingra ENT 8e explicitly states that atticoantral CSOM is "unsafe" precisely *because* it is almost invariably associated with cholesteatoma formation. ### Why NOT Atticoantral CSOM with Osteitis Alone (Option D)? "Atticoantral CSOM with osteitis" (Option D) is a broader, less specific category. While all cholesteatomas occur in the atticoantral region, not all atticoantral CSOM involves cholesteatoma. However, the specific combination of **posterosuperior marginal perforation + granulation tissue + foul-smelling discharge + CT ossicular erosion** in a 28-year-old with 3 years of progressive disease is the classic, high-yield presentation of **cholesteatoma** — the most specific and clinically actionable diagnosis. Option D is a less precise diagnosis that does not capture the underlying pathological entity driving the bone destruction. ### Why Other Options Are Wrong - **Option A (Tubotympanic CSOM):** Features a **central** (not marginal) perforation, mucopurulent (not foul-smelling) discharge, no granulation tissue, and rarely causes ossicular erosion. Excluded by the posterosuperior marginal perforation. - **Option C (Acute suppurative otitis media):** Presents acutely (days) with fever and otalgia. A 3-year progressive course with CT bone erosion is incompatible with ASOM. - **Option D (Atticoantral CSOM with osteitis):** Less specific than cholesteatoma; does not identify the pathological entity responsible for the bone destruction described. ### Management Cholesteatoma requires surgical eradication: - **Canal wall down (CWD) mastoidectomy** (modified radical mastoidectomy): Preferred for extensive disease; creates open cavity for surveillance - **Canal wall up (CWU) mastoidectomy**: Preserves anatomy; requires mandatory second-look surgery at 12 months - **Ossiculoplasty**: For hearing rehabilitation after disease clearance [cite: Dhingra ENT 8e Ch 11; Scott-Brown's Otorhinolaryngology 8e; Hazarika ENT 5e Ch 12] 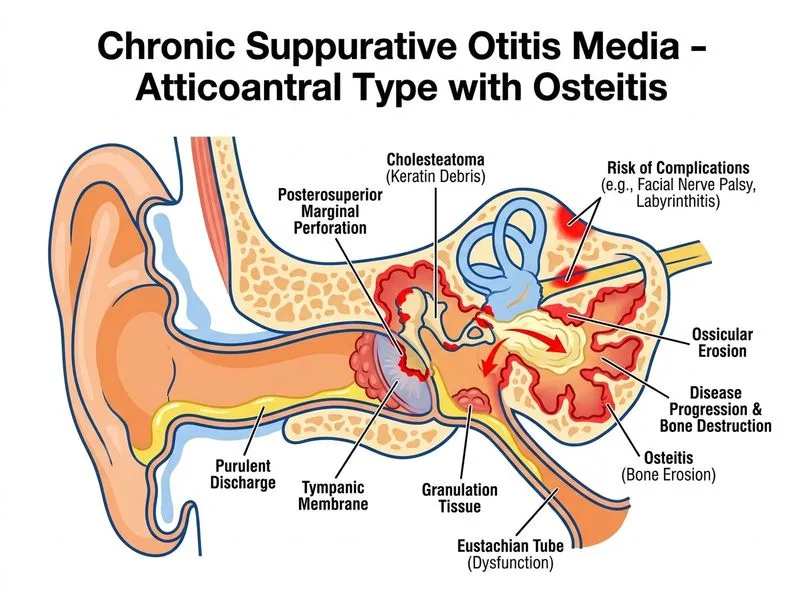
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.