## CKD-Mineral Bone Disorder: Adynamic Bone Disease ### Clinical Presentation Analysis **Key Point:** The combination of **low bone turnover** (on biopsy), **minimal osteoid**, **normal-to-low alkaline phosphatase**, and **relatively modest iPTH elevation** (180 pg/mL) in stage 3b CKD is pathognomonic for **adynamic bone disease (ABD)**. ### Pathophysiology of Adynamic Bone Disease ```mermaid flowchart TD A[CKD Stage 3-4]:::outcome --> B[Phosphate retention]:::outcome B --> C{Aggressive phosphate binder<br/>+ Vitamin D analog use}:::decision C -->|Over-suppression| D[PTH suppressed below target]:::action D --> E[Reduced osteoblast activity]:::action E --> F[Low bone turnover]:::outcome F --> G[Minimal osteoid deposition]:::outcome G --> H[Adynamic Bone Disease]:::outcome I[Impaired bone remodeling] -.-> H J[Increased fracture risk] -.-> H ``` ### Why This Patient Has ABD 1. **Over-suppression of PTH:** iPTH 180 pg/mL is *low-normal* for CKD stage 3b (target 70–110 pg/mL for stage 3, up to 300 for stage 5). If the patient has been on phosphate binders and vitamin D analogs, PTH may have been suppressed too aggressively. 2. **Low bone turnover:** Histology shows minimal osteoid and low turnover—PTH is the primary stimulus for osteoblast activity and bone remodeling. 3. **Low alkaline phosphatase:** Reflects reduced bone formation (osteoblast activity). 4. **Asymptomatic:** ABD is often clinically silent until fractures occur. ### Differential Diagnosis of CKD-MBD | Feature | ABD | Osteitis Fibrosa | Osteomalacia | Mixed | |---------|-----|------------------|--------------|-------| | **PTH** | Low-normal/suppressed | Very high (>600) | Normal-low | Variable | | **Bone turnover** | Low | High | Low | Mixed | | **Osteoid** | Minimal | Abundant | Abundant | Abundant | | **Alkaline phosphatase** | Normal-low | Elevated | Elevated | Elevated | | **Mechanism** | PTH over-suppression | Uncontrolled hyperparathyroidism | Vitamin D deficiency | Multiple defects | **Clinical Pearl:** ABD is increasingly recognized in CKD patients treated aggressively with phosphate binders and calcitriol. The goal of therapy is to maintain PTH in the "sweet spot"—not too low, not too high. ### Why Other Options Are Wrong - **Osteitis fibrosa cystica:** Requires *very high* PTH (usually >600 pg/mL), abundant osteoid, and elevated alkaline phosphatase. This patient's iPTH is only 180 and osteoid is minimal. - **Osteomalacia:** Would show abundant osteoid (not minimal), low alkaline phosphatase is expected, but the iPTH would typically be elevated (>300) as the parathyroids attempt to compensate for low 1,25-vitamin D. Here, iPTH is suppressed. - **Mixed uremic osteodystrophy:** Presents with *high* bone turnover and abundant osteoid. This biopsy shows *low* turnover and minimal osteoid. ### Management Strategy **High-Yield:** - Reduce or discontinue phosphate binders and vitamin D analogs temporarily. - Monitor PTH; target range for stage 3b is 70–110 pg/mL. - Ensure adequate dietary calcium and phosphate intake. - Avoid over-treatment of secondary hyperparathyroidism. - Consider PTH-stimulating agents (cinacalcet) only if PTH is high; avoid if already suppressed. **Mnemonic: "ABD = Aggressive Binder Dosing"** — Over-suppression of PTH with phosphate binders and vitamin D causes adynamic bone disease. 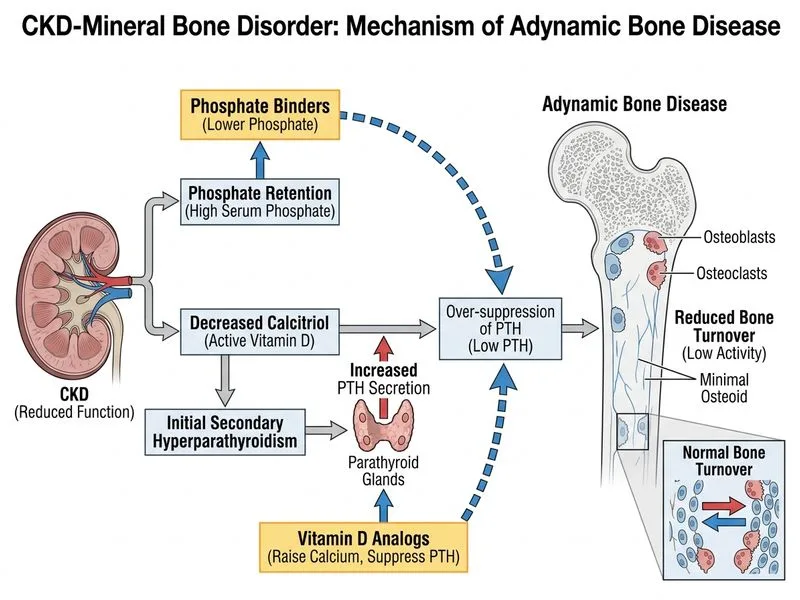
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.