## ESA-Resistant Anemia: Iron Deficiency vs. Chronic Inflammation ### Pathophysiology of ESA Resistance in CKD ESA-resistant anemia in CKD can result from multiple mechanisms: 1. **Absolute iron deficiency** — genuinely depleted iron stores (low ferritin, low serum iron, elevated TIBC) 2. **Functional iron deficiency (chronic inflammation)** — iron sequestered in reticuloendothelial system due to hepcidin-mediated blockade; iron stores are PRESENT but unavailable 3. **Cytokine-mediated suppression** — independent of iron status ### The Key Distinguishing Feature **Key Point:** The question asks what **best distinguishes** ESA-resistant anemia due to iron deficiency FROM ESA-resistant anemia due to chronic inflammation. The single most discriminating parameter is **ferritin**: - **Absolute iron deficiency:** Low serum iron + **LOW ferritin** (<30 ng/mL) + Low transferrin saturation (<20%) + Elevated TIBC - **Functional iron deficiency / Chronic inflammation:** Low serum iron + **HIGH ferritin** (>200 ng/mL, as ferritin is an acute-phase reactant) + Low transferrin saturation (<20%) + Normal or low TIBC **Option B — "Serum ferritin >200 ng/mL with low transferrin saturation"** is the pattern that characterizes ESA-resistant anemia due to **chronic inflammation** (functional iron deficiency). This combination — elevated ferritin (reflecting inflammation/iron sequestration) alongside low transferrin saturation (reflecting poor iron availability for erythropoiesis) — is the hallmark that distinguishes it from true iron deficiency, where ferritin would be low. ### Clinical Correlation **Clinical Pearl:** The patient in the vignette has ferritin 520 ng/mL (elevated), serum iron 45 µg/dL (low), TIBC 210 µg/dL (low), and transferrin saturation ≈ 21% (borderline low). This pattern is consistent with **functional iron deficiency due to chronic inflammation**, not absolute iron deficiency. The elevated ferritin in the setting of low serum iron and low TIBC is the discriminating feature. ### Table: Iron Metabolism in ESA-Resistant Anemia | Parameter | Absolute Iron Deficiency | Functional Iron Deficiency (Inflammation) | | --- | --- | --- | | **Serum iron** | Low (<60 µg/dL) | Low (<60 µg/dL) | | **Ferritin** | **Low (<30 ng/mL)** | **Elevated (>200 ng/mL)** | | **Transferrin saturation** | Low (<20%) | Low (<20%) | | **TIBC** | Elevated (>360 µg/dL) | Normal or low | | **Hepcidin** | Low | Elevated | | **Bone marrow iron** | Absent | Present (macrophage siderosis) | | **Response to IV iron** | Excellent | Poor | ### Why Other Options Are Incorrect - **Option A** (normal serum iron, elevated ferritin, normal TIBC): This pattern does not represent either condition accurately; in inflammation, serum iron is typically low. - **Option C** (elevated hepcidin, low serum iron, normal iron stores): While mechanistically accurate for inflammation, hepcidin is not routinely measured clinically and is not the standard discriminating test used in NEET PG practice. - **Option D** (low serum iron, low ferritin, low transferrin saturation): This is the classic pattern of **absolute iron deficiency**, not chronic inflammation. It does not distinguish inflammation-mediated ESA resistance. **High-Yield:** The combination of **elevated ferritin (>200 ng/mL) + low transferrin saturation (<20%)** in a CKD patient on ESA is the textbook marker of functional iron deficiency / anemia of chronic inflammation, as per Harrison's Principles of Internal Medicine and KDIGO 2012 CKD-MBD guidelines. [cite: Harrison 21e Ch 297; KDIGO 2012 Anemia Guidelines; KD Tripathi 8e Ch 12] 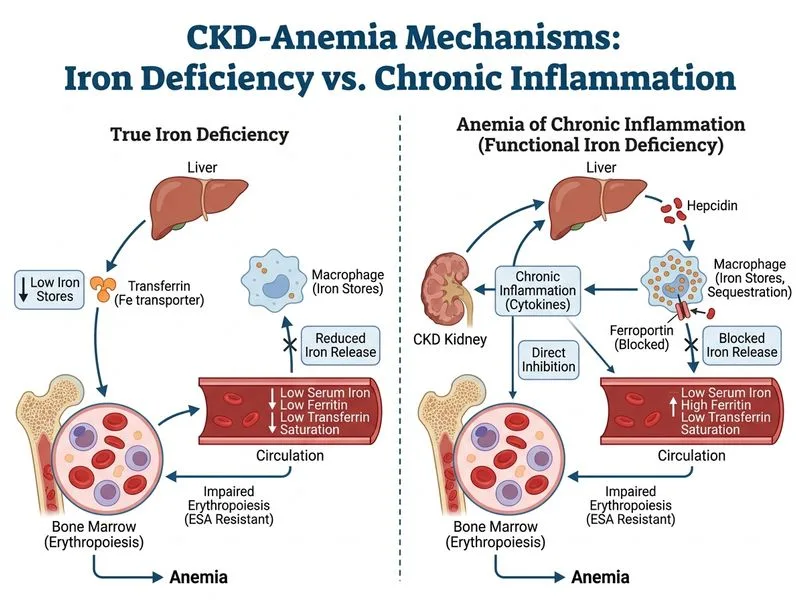
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.