## Pilocytic Astrocytoma — Imaging Hallmark **Key Point:** Pilocytic astrocytoma (WHO Grade I) classically presents as a **cystic lesion with an enhancing mural nodule** — this is the pathognomonic imaging pattern. ### MRI Characteristics | Feature | Pilocytic Astrocytoma | High-Grade Glioma | |---------|----------------------|-------------------| | **Cyst** | Large, prominent | Rare or small | | **Mural nodule** | Single, enhancing | Multiple nodules | | **Enhancement** | Nodule only | Heterogeneous | | **Edema** | Minimal | Extensive | | **Necrosis** | Absent | Common | | **Mass effect** | Mild | Severe | ### Typical Location & Demographics - **Cerebellum** (50–70% of cases) — most common pediatric posterior fossa tumor - **Optic pathway** (15–20%) — associated with neurofibromatosis type 1 (NF1) - **Brainstem and cerebral hemispheres** — less common - Peak age: **5–15 years** **High-Yield:** The **cyst + mural nodule** pattern is so characteristic that it is virtually diagnostic of pilocytic astrocytoma in a pediatric patient. This benign tumor has an excellent prognosis (>90% 10-year survival) and often does not require chemotherapy or radiation if completely resected. **Clinical Pearl:** Pilocytic astrocytomas are **indolent and slow-growing**. Even large cystic lesions with mass effect may be asymptomatic for years. Imaging stability over time is common and does not mandate immediate intervention. ### Why NOT the Other Patterns - **Heterogeneous enhancement with necrosis** = high-grade glioma (WHO III–IV) - **Homogeneous T2 hyperintensity** = low-grade diffuse astrocytoma (WHO II), not pilocytic - **Ring enhancement with restricted diffusion** = abscess or high-grade tumor, not pilocytic [cite:Robbins 10e Ch 28] 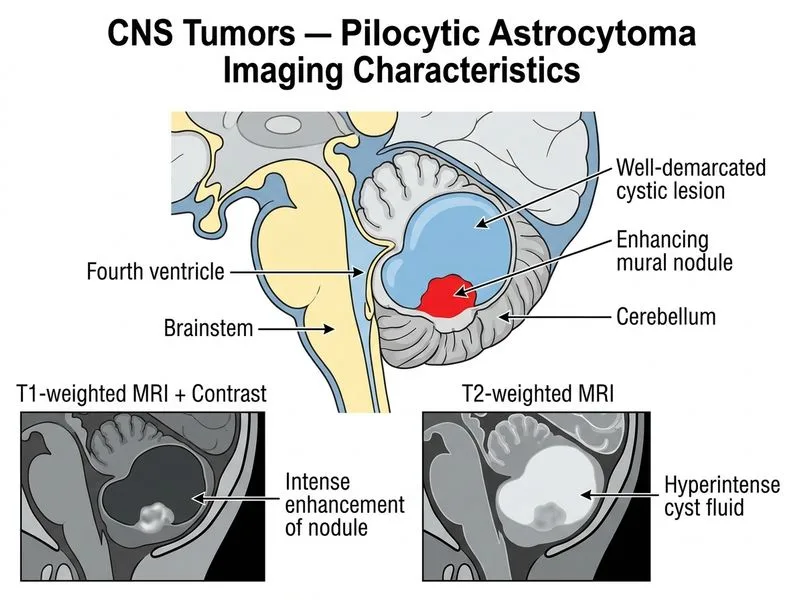
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.