## Pilocytic Astrocytoma: Classic Presentation and Imaging **Key Point:** The combination of a **well-circumscribed cystic cerebellar mass with an enhancing mural nodule** in a young adult (age 5–30 years) is the classic presentation of **pilocytic astrocytoma (WHO Grade I)**, the most common cerebellar tumor in children and young adults. ### Characteristic Imaging Features | Feature | Pilocytic Astrocytoma | Hemangioblastoma | Medulloblastoma | Ependymoma | |---------|----------------------|------------------|-----------------|------------| | Location | Midline cerebellum (vermis) | Cerebellar hemisphere | Midline cerebellum (vermis) | Fourth ventricle | | Morphology | Cyst + mural nodule | Cyst + mural nodule | Solid mass | Solid/mixed | | Enhancement | Avid nodule | Avid nodule | Heterogeneous | Heterogeneous | | Edema | Minimal | Minimal | Significant | Variable | | Age of onset | 5–20 years (peak) | 20–40 years | 5–10 years | 20–40 years | | Hemorrhage | Rare | Common (microhemorrhages) | Rare | Rare | | VHL association | None | 20–30% | None | None | **High-Yield:** Pilocytic astrocytoma is the **most common posterior fossa tumor in children and young adults**. The classic imaging triad is: (1) midline cerebellar location, (2) large cyst with a small mural nodule, and (3) avid nodule enhancement with minimal surrounding edema. ### Why NOT Hemangioblastoma? Although hemangioblastoma also presents as a cyst-with-nodule, key distinguishing features favor pilocytic astrocytoma here: 1. **Age:** Pilocytic astrocytoma peaks at 5–20 years; hemangioblastoma peaks at 30–60 years. A 28-year-old is at the upper end of pilocytic astrocytoma range but more typical than hemangioblastoma. 2. **Location:** Pilocytic astrocytoma classically involves the **midline cerebellum (vermis)**; hemangioblastoma more commonly involves the cerebellar **hemispheres**. 3. **Epidemiology:** Pilocytic astrocytoma is far more common overall; hemangioblastoma is relatively rare and usually sporadic or VHL-associated. 4. **Hemorrhage:** Hemangioblastoma is prone to microhemorrhages due to its vascular nature; pilocytic astrocytoma is not. ### Pathophysiology and Clinical Features 1. **WHO Grade I** — benign, slow-growing glial tumor with excellent prognosis after surgical resection 2. Biphasic histology: compact bipolar cells with Rosenthal fibers + loose multipolar cells with microcysts 3. Cerebellar location → truncal ataxia, nystagmus, appendicular dysmetria 4. Mass effect on fourth ventricle → obstructive hydrocephalus → morning vomiting, headache 5. Avid mural nodule enhancement due to leaky tumor vasculature (breakdown of blood-brain barrier) **Clinical Pearl:** The **cyst wall does NOT enhance** in pilocytic astrocytoma (unlike some other cystic tumors); only the mural nodule enhances avidly. Surgical resection of the nodule is curative in most cases. ### Why Other Options Are Incorrect? - **Ependymoma:** Arises from the floor of the fourth ventricle; typically solid with calcifications; "plastic" extension through foramina of Luschka/Magendie; does NOT present as a cyst-with-nodule. - **Medulloblastoma:** Solid, highly cellular, midline vermian mass in children; minimal cystic change; significant surrounding edema; aggressive (WHO Grade IV). - **Hemangioblastoma:** Cerebellar hemisphere (not midline); older adults (30–60 years); associated with VHL; prone to hemorrhage; less common than pilocytic astrocytoma. [cite:Robbins 10e Ch 27; Nelson Textbook of Pediatrics 21e; Osborn's Brain 3e] 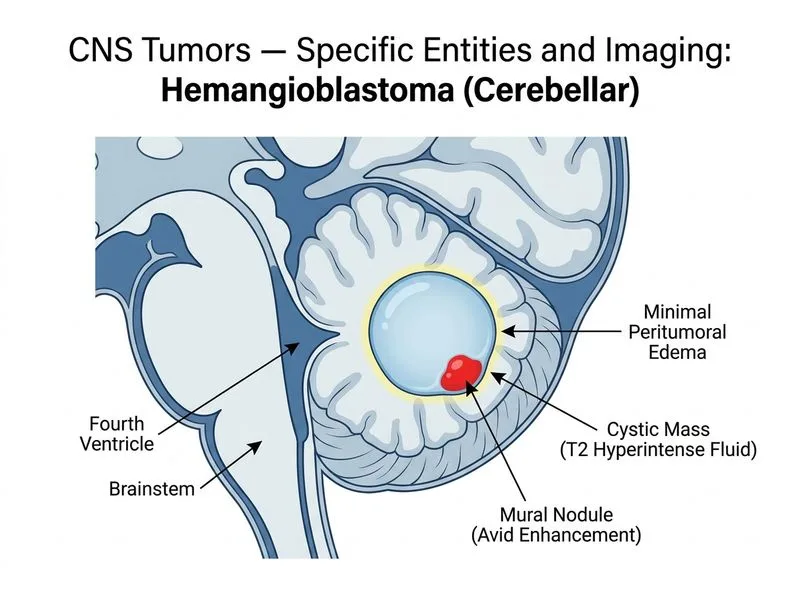
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.