## Diagnosis: Medulloblastoma ### Clinical Presentation **Key Point:** Medulloblastoma is the most common malignant brain tumor in children, typically presenting in children aged **3–10 years** with signs of increased intracranial pressure (morning headaches, vomiting) and cerebellar dysfunction (ataxia). ### Imaging Characteristics — Diagnostic Hallmarks **High-Yield:** Classic imaging features include: - **Location:** Midline, arising from the **4th ventricle floor** (from the cerebellar vermis) - **Signal intensity:** Hypointense on T1, hyperintense on T2 (gray matter–like signal) - **Enhancement:** Heterogeneous (not uniform) - **Restricted diffusion:** High cellularity causes **restricted diffusion on DWI** — this is a key distinguishing feature - **Hydrocephalus:** Obstructive hydrocephalus is common due to 4th ventricle obstruction - **Hemorrhage/necrosis:** May be present in larger tumors ### Why Restricted Diffusion Matters **Clinical Pearl:** Restricted diffusion (low ADC) indicates high cell density and is a hallmark of **high-grade, rapidly proliferating tumors**. Medulloblastoma is a WHO Grade IV tumor with very high cellularity, making restricted diffusion a key imaging clue. ### Differential Diagnosis | Feature | Medulloblastoma | Pilocytic Astrocytoma | Ependymoma | Brainstem Glioma | |---------|-----------------|----------------------|------------|------------------| | **Location** | 4th ventricle midline | Cerebellar hemisphere or brainstem | 4th ventricle wall | Pons/midbrain | | **Age** | 3–10 years (peak) | Children/young adults | 3–9 years | 5–10 years | | **Signal** | Hypointense T1, hyperintense T2 | Mixed | Heterogeneous | Hypointense T1, hyperintense T2 | | **Enhancement** | Heterogeneous | Homogeneous nodule | Heterogeneous | Homogeneous | | **Restricted diffusion** | **Yes (high cellularity)** | No | No | No | | **Hydrocephalus** | Marked (obstructive) | Mild–moderate | Marked | Mild | | **Grade** | WHO IV (malignant) | WHO I (benign) | WHO II–III | WHO II–III | | **Prognosis** | Poor (5-year survival ~70%) | Excellent (> 90%) | Intermediate | Variable | ### Pathology & Biology **Mnemonic:** **PNET** = Primitive Neuro-Ectodermal Tumor. Medulloblastoma is a small round blue cell tumor with high mitotic activity and apoptosis. It arises from primitive neuroectodermal precursor cells in the cerebellar vermis. ### Metastatic Potential **Warning:** Medulloblastoma has a **high propensity for leptomeningeal spread** (up to 30% at diagnosis). Spinal MRI and CSF analysis are mandatory at diagnosis. ### Management Algorithm ```mermaid flowchart TD A[Medulloblastoma diagnosed]:::outcome --> B[Staging: Spinal MRI + CSF cytology]:::action B --> C{Metastatic disease?}:::decision C -->|No| D[Maximal safe surgical resection]:::action C -->|Yes| E[Chemotherapy first, then surgery]:::action D --> F[Chemotherapy + Radiation]:::action E --> F F --> G[5-year survival ~70%]:::outcome ``` [cite:Osborn's Brain Imaging, Pathology, and Anatomy Ch 8; Harrison 21e Ch 397] 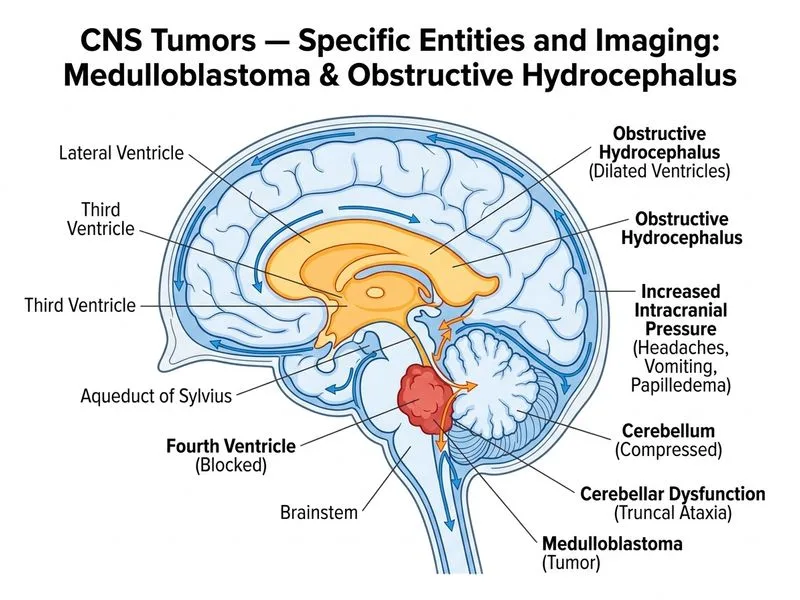
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.