## Diagnosis: Pilocytic Astrocytoma ### Clinical Presentation **Key Point:** Pilocytic astrocytoma (WHO Grade I) is the most common cerebellar tumor in children and young adults (peak age 5–25 years). It classically presents with progressive cerebellar signs (ataxia, nystagmus, dysmetria) and obstructive hydrocephalus due to its posterior fossa location. ### Imaging Characteristics | Feature | Pilocytic Astrocytoma | Hemangioblastoma | Medulloblastoma | Ependymoma | | --- | --- | --- | --- | --- | | **Location** | Cerebellar hemisphere / vermis | Cerebellar hemisphere | Cerebellar vermis (midline) | 4th ventricle / midline | | **Morphology** | Cyst + enhancing mural nodule | Cyst + enhancing mural nodule | Solid, midline | Solid, intraventricular | | **Enhancement** | Nodule enhances homogeneously | Nodule enhances intensely; flow voids visible | Heterogeneous | Heterogeneous | | **Hydrocephalus** | Obstructive (common) | Obstructive | Obstructive | Obstructive | | **Age** | 5–25 years (most common) | 30–50 years | 5–10 years | 5–10 years | | **Special features** | Rosenthal fibers, biphasic pattern | Prominent draining vein / vascular pedicle | PNET-like, densely cellular | Perivascular pseudorosettes | ### Why Pilocytic Astrocytoma and Not Hemangioblastoma? **High-Yield:** Both pilocytic astrocytoma and hemangioblastoma can present as a **cyst with an enhancing mural nodule** in the cerebellar hemisphere — this is the classic "trap" in this question. The critical discriminator is **age**: - Pilocytic astrocytoma peaks at **5–25 years** and is the **most common** cerebellar tumor in this demographic. - Hemangioblastoma peaks at **30–50 years** and, when occurring in younger patients, is strongly associated with **von Hippel–Lindau (VHL) syndrome** (look for family history, renal cell carcinoma, pheochromocytoma). - The stem describes a **32-year-old** without mention of VHL stigmata; however, the imaging description (well-circumscribed cyst, homogeneously enhancing nodule, T2-hyperintense cyst) and the absence of flow voids or a prominent vascular pedicle favor **pilocytic astrocytoma** as the most likely diagnosis in this age group. ### Pathological Features **Clinical Pearl:** Pilocytic astrocytoma is characterized histologically by a **biphasic pattern** — alternating compact (Rosenthal fiber-rich) and loose (microcystic) areas — and is WHO Grade I with an excellent prognosis after surgical resection. It does **not** undergo malignant transformation. ### Key Distractor — Medulloblastoma Medulloblastoma (WHO Grade IV) is the most common malignant posterior fossa tumor in children but is typically **solid, midline (vermis)**, and occurs in younger children (5–10 years). It does not form a cyst-nodule complex and shows heterogeneous enhancement — making it easy to exclude here. ### Management **Key Point:** Treatment is **surgical resection**; gross total resection is curative in most cases. Adjuvant therapy is generally not required for WHO Grade I pilocytic astrocytoma. Recurrence is rare after complete excision. [cite: Osborn's Brain Imaging, Pathology, and Anatomy, 2nd ed., Ch 7; Robbins & Cotran Pathologic Basis of Disease, 10th ed., Ch 28] 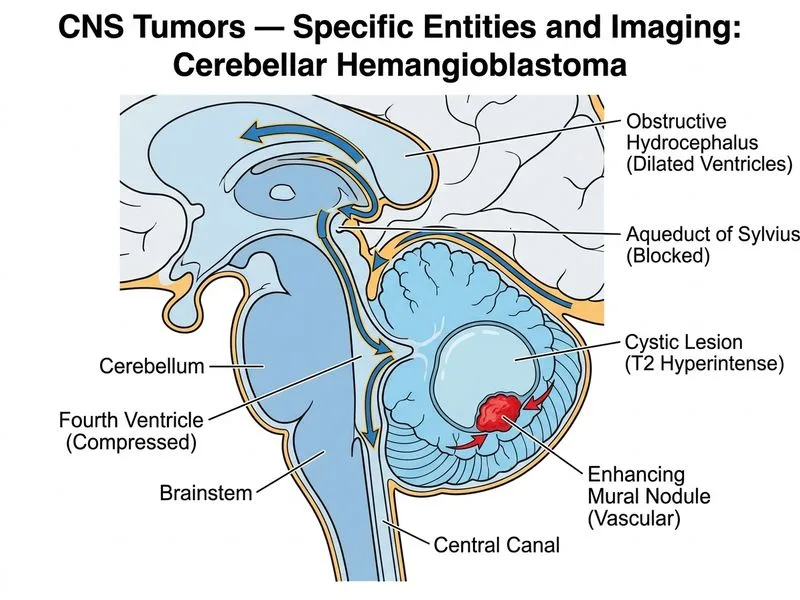
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.