## Diagnosis: Glioblastoma Multiforme (WHO Grade IV Glioma) ### Clinical Presentation **Key Point:** Glioblastoma (GBM) is the most common and aggressive primary malignant brain tumor in adults. It typically presents with rapid onset (weeks to months) of focal neurological deficits, seizures, cognitive changes, and signs of increased intracranial pressure. ### Imaging Characteristics | Feature | GBM (Grade IV) | Anaplastic Astrocytoma (Grade III) | Low-Grade Astrocytoma (Grade II) | Oligodendroglioma | | --- | --- | --- | --- | --- | | **Enhancement** | Irregular, patchy, heterogeneous | Moderate, less heterogeneous | Minimal or none | Patchy, less aggressive | | **Necrosis** | Prominent (hallmark) | Rare or absent | Absent | Absent | | **Edema** | Severe, extensive | Moderate | Minimal | Minimal to moderate | | **T1 signal** | Hypointense (tumor) + hyperintense (hemorrhage/contrast) | Hypointense | Hypointense | Hypointense | | **T2/FLAIR** | Hyperintense | Hyperintense | Hyperintense | Hyperintense | | **Mass effect** | Marked, with midline shift | Moderate | Minimal | Minimal to moderate | | **Age** | 45–70 years (peak 55–65) | 30–50 years | 20–40 years | 40–50 years | | **Prognosis** | Median OS ~15 months | Median OS ~2–3 years | Median OS 5–10 years | Median OS 5–10 years | ### Pathognomonic Features **High-Yield:** GBM is defined by the presence of **necrosis** and **microvascular proliferation** on histology. Imaging hallmarks include: - **Heterogeneous enhancement** (irregular, patchy, "Swiss cheese" pattern) - **Central necrosis** (non-enhancing core) - **Severe perilesional edema** (vasogenic) - **Rapid growth** and significant mass effect ### WHO Classification Context **Mnemonic:** **GOAD** — Grade IV (GBM) has **O**verall poor prognosis, **A**ggressive growth, **D**istinct necrosis. ### Diagnostic Workup **Clinical Pearl:** MR spectroscopy (MRS) shows elevated choline, depressed N-acetylaspartate (NAA), and elevated lactate/lipid peaks in GBM, reflecting high cellularity and necrosis. Perfusion-weighted imaging (PWI) demonstrates elevated relative cerebral blood volume (rCBV) due to necroangiogenesis. ### Management **Key Point:** Standard of care is **maximal safe surgical resection** followed by **concurrent chemoradiotherapy** (Stupp protocol: 60 Gy radiation + temozolomide), then adjuvant temozolomide. Despite aggressive treatment, prognosis remains poor (median overall survival ~15 months). [cite:Osborn's Brain Imaging, Pathology, and Anatomy Ch 7; Harrison 21e Ch 375] 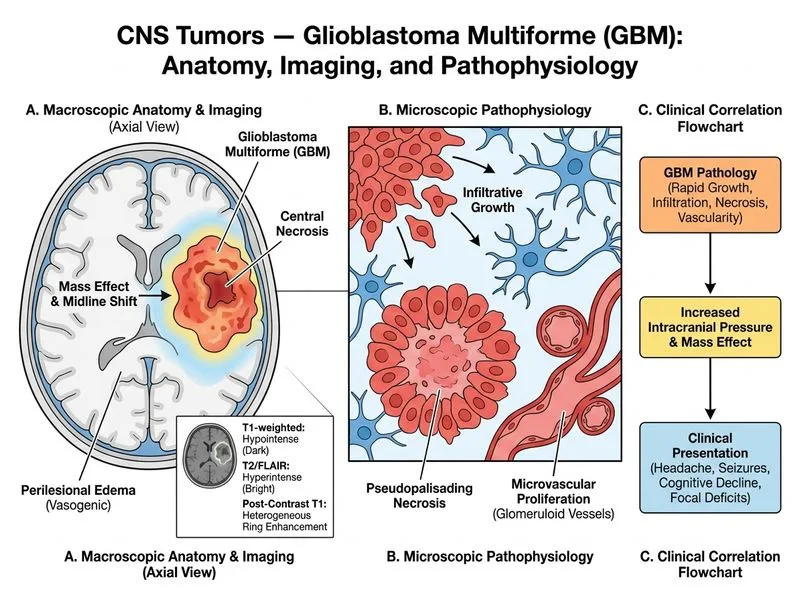
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.