## Clinical Presentation & Diagnosis This patient presents with **severe thrombocytopenia (8,000/µL)** with a long history of easy bruising and mucocutaneous bleeding, but **normal coagulation studies (PT, aPTT)** and a **normocellular bone marrow with adequate megakaryocytes**. These findings are pathognomonic for **Immune Thrombocytopenia (ITP)**. ## Pathophysiology **Key Point:** ITP is an autoimmune disorder characterized by IgG antibodies against platelet surface antigens (GPIIb/IIIa, GPIb/IX), leading to complement-mediated and Fc-receptor-mediated platelet destruction in the spleen and liver. ## Diagnostic Criteria for ITP | Feature | ITP | TTP | DIC | HUS | |---------|-----|-----|-----|-----| | **Platelet count** | <30,000/µL | <30,000/µL | <100,000/µL | <30,000/µL | | **PT/aPTT** | Normal | Normal | Prolonged | Normal | | **Fibrinogen** | Normal | Normal | ↓ | Normal | | **Schistocytes** | Absent | Present | Present | Present | | **Renal involvement** | Absent | Present (MAHA) | Present | Present (HUS hallmark) | | **Neurological signs** | Absent | Present (TTP hallmark) | Absent | Absent | | **BM megakaryocytes** | Adequate/↑ | Normal | Normal/↓ | Normal | ## Why This Patient Has ITP 1. **Isolated thrombocytopenia** — platelet count severely low, but RBC and WBC normal. 2. **Normal coagulation cascade** — PT and aPTT normal, indicating intact extrinsic and intrinsic pathways; fibrinogen not consumed. 3. **Adequate bone marrow response** — megakaryocytes present and adequate, ruling out bone marrow failure. 4. **Chronic presentation** — history of easy bruising since childhood suggests chronic immune-mediated destruction, not acute consumptive process. 5. **Absence of microangiopathic hemolytic anemia (MAHA)** — no schistocytes mentioned; Hb low due to bleeding, not hemolysis. ## High-Yield Mnemonic **"ITP = Isolated Thrombocytopenia with Preserved coagulation"** — when you see low platelets + normal PT/aPTT + normal fibrinogen + adequate BM megakaryocytes, think ITP first. ## Clinical Pearl **Bleeding time is prolonged in ITP** because platelet count is so low that platelet plug formation is impaired, even though individual platelet function is normal. Modern labs have abandoned bleeding time; diagnosis is clinical + platelet count + BM exam. ## Management Approach ```mermaid flowchart TD A[Platelet count <30,000/µL + mucocutaneous bleeding]:::outcome --> B{Coagulation studies normal?}:::decision B -->|Yes| C{Adequate BM megakaryocytes?}:::decision B -->|No| D[Consider DIC, TTP, HUS]:::outcome C -->|Yes| E[ITP diagnosis]:::action C -->|No| F[Bone marrow failure]:::outcome E --> G{Platelet count <20,000 or active bleeding?}:::decision G -->|Yes| H[Corticosteroids ± IVIG]:::action G -->|No| I[Observation or low-dose steroids]:::action ``` [cite:Robbins 10e Ch 13] 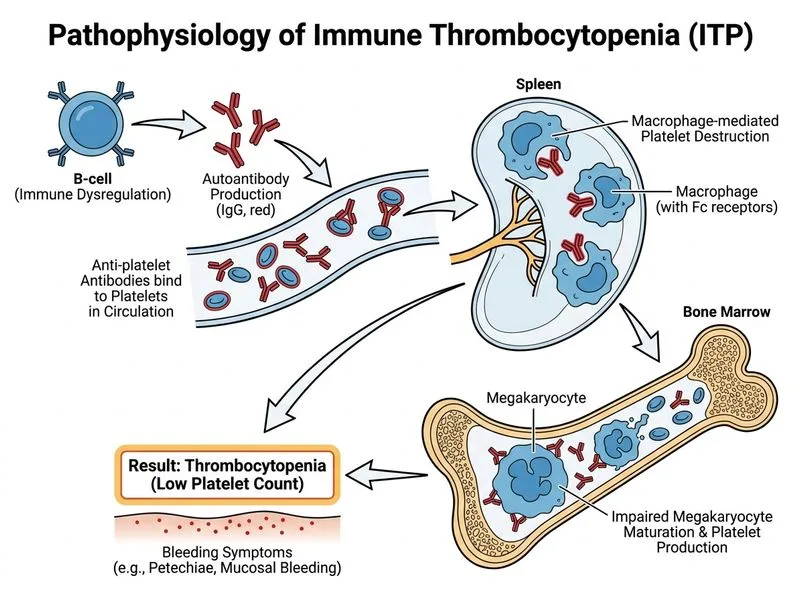
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.