## Clinical Context & Pathophysiology This patient has **cirrhosis-induced coagulopathy**, a complex disorder combining: 1. **Hepatic synthetic dysfunction** — impaired production of clotting factors (II, V, VII, IX, X, XI, XII, fibrinogen) 2. **Portal hypertension** — splenomegaly causing thrombocytopenia 3. **Impaired clearance** — reduced inactivation of fibrinolytic mediators (plasminogen activators) ## Why This Is NOT Acute DIC **Key Point:** Although this patient has some features suggestive of DIC (low fibrinogen, elevated D-dimer, prolonged PT/aPTT), the **persistent coagulopathy despite FFP transfusion** is the critical clue that points to **hepatic synthetic dysfunction**, not consumptive coagulopathy. ## Differential: Cirrhosis vs. DIC | Feature | Cirrhosis | DIC | |---------|-----------|-----| | **Fibrinogen** | Low (chronic) | Very low (acute consumption) | | **Platelets** | Low (splenomegaly) | Very low (consumption) | | **PT/aPTT** | Prolonged (factor deficiency) | Prolonged (consumption) | | **D-dimer** | Mildly ↑ (impaired clearance) | Markedly ↑ (active thrombin generation) | | **Response to FFP** | **Poor/transient** | **Good initial response** | | **Vitamin K response** | **Poor** (liver cannot use it) | **Good** (if deficiency component) | | **Antithrombin III** | Normal/high | Low (consumed) | | **Prothrombin time trend** | Chronic, stable or worsening | Acute, rapidly worsening | ## Why FFP Failed to Correct PT ```mermaid flowchart TD A[Cirrhotic patient with variceal bleed]:::outcome --> B{Cause of coagulopathy?}:::decision B -->|Hepatic synthetic dysfunction| C[Impaired production of factors II, V, VII, IX, X]:::outcome B -->|Consumption DIC| D[Active consumption of factors]:::outcome C --> E[FFP transfusion provides factors]:::action D --> E E --> F{Does PT improve?}:::decision F -->|Yes, sustained| G[DIC likely; factors being consumed but transfused]:::outcome F -->|No, or transient| H[Hepatic dysfunction likely; liver cannot produce new factors]:::outcome H --> I[Vitamin K ineffective because liver cannot activate factors]:::action I --> J[Only time + liver recovery improves coagulopathy]:::action ``` ## High-Yield Pathophysiology **High-Yield:** In cirrhosis, FFP provides a **temporary boost** of clotting factors, but because the **liver cannot synthesize new factors**, the PT remains prolonged. Vitamin K is also ineffective because: - Vitamin K-dependent factors (II, VII, IX, X) require **hepatic carboxylation** to become active. - A cirrhotic liver has **impaired synthetic capacity**, so even with vitamin K supplementation, factor production remains inadequate. ## Why Other Options Are Wrong **Ongoing consumption (Option A):** While some consumption may occur during active bleeding, the **failure of FFP to sustain PT correction** is not typical of DIC. In DIC, FFP transfusion usually produces at least a transient improvement because factors are being actively consumed and replaced. Here, the PT remains persistently prolonged despite FFP, indicating the problem is **production failure**, not consumption. **Vitamin K deficiency alone (Option C):** Cirrhotic patients often have vitamin K deficiency (malabsorption, antibiotic use), but vitamin K alone cannot correct the coagulopathy because the liver cannot activate the vitamin K-dependent factors. FFP + vitamin K should improve PT in pure vitamin K deficiency; failure to do so indicates hepatic dysfunction. **Platelet dysfunction (Option D):** While cirrhotic patients may have qualitative platelet dysfunction, the prolonged PT is a **coagulation cascade abnormality**, not a platelet function problem. Platelet dysfunction would cause prolonged bleeding time (now abandoned) or platelet aggregation defects, not prolonged PT. ## Clinical Pearl **"Cirrhosis = production failure; DIC = consumption failure."** FFP works in DIC (replaces consumed factors) but fails in cirrhosis (liver cannot make new factors). Vitamin K works in vitamin K deficiency but fails in cirrhosis (liver cannot use it). ## Management Implications 1. **FFP** — temporary measure only; repeated transfusions risk fluid overload. 2. **Vitamin K** — ineffective in cirrhosis; may help if concurrent deficiency. 3. **Prothrombin complex concentrate (PCC)** — more concentrated, preferred over FFP in cirrhosis. 4. **Platelet transfusion** — if platelet count <50,000/µL during active bleeding. 5. **Definitive treatment** — liver transplantation; medical management is supportive. [cite:Harrison 21e Ch 297] 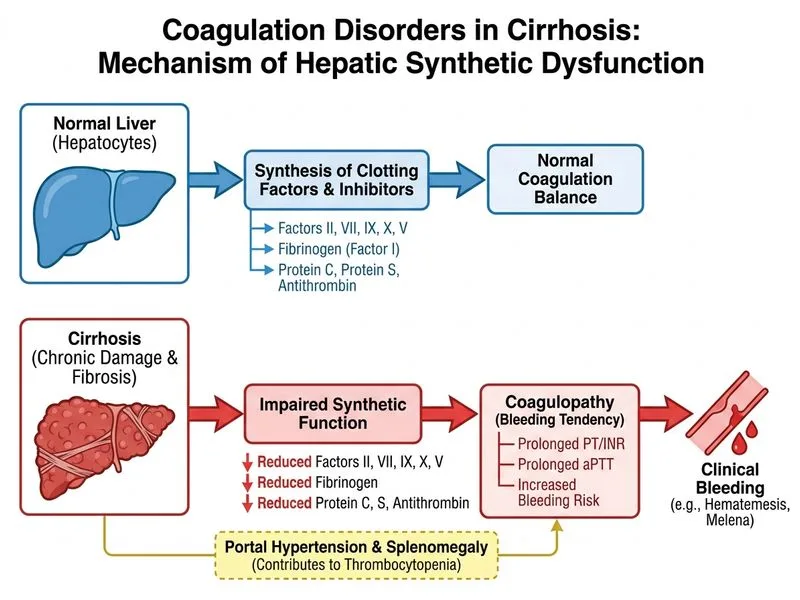
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.