## Diagnostic Confirmation and Urgency **Key Point:** This patient has clinical compartment syndrome with a critical compartment pressure differential. Compartment pressure of 58 mmHg with diastolic BP of 75 mmHg yields a differential of 17 mmHg — **well below the safe threshold of 30 mmHg**. Fasciotomy must be performed emergently. ## Why Intact Pulses Do NOT Exclude Compartment Syndrome **High-Yield:** Compartment syndrome causes **tissue ischemia** long before arterial flow is compromised. Distal pulses remain palpable because systolic pressure (typically 120 mmHg) exceeds compartment pressure (58 mmHg). However, capillary perfusion in the muscle tissue is already failing because: $$\text{Capillary perfusion pressure} = \text{Diastolic BP} - \text{Compartment pressure} = 75 - 58 = 17 \text{ mmHg}$$ Normal capillary perfusion requires ≥30 mmHg. This patient's tissues are **ischemic despite palpable pulses**. **Warning:** The presence of distal pulses is a **false reassurance** and a common diagnostic trap. Compartment syndrome is a **surgical emergency** based on clinical signs and pressure measurement, not on vascular examination. ## Management Algorithm ```mermaid flowchart TD A[Crush injury + severe pain + pain on passive stretch]:::outcome --> B{Compartment pressure measured?}:::decision B -->|Yes| C{Pressure differential < 30 mmHg?}:::decision C -->|Yes| D[Emergency fasciotomy]:::urgent C -->|No| E[Observe, repeat measurements q2h]:::action D --> F[Prevent rhabdomyolysis and tissue necrosis]:::outcome E --> G{Deterioration or pressure rise?}:::decision G -->|Yes| D G -->|No| H[Continue monitoring]:::action ``` ## Why Other Options Fail | Option | Why It's Wrong | |--------|----------------| | Mannitol monotherapy | Treats rhabdomyolysis sequelae (myoglobinuria, AKI) but does NOT decompress the compartment. Tissue necrosis continues unchecked. | | Cast and elevation | Immobilization and elevation worsen compartment pressure and reduce perfusion gradient. Contraindicated in compartment syndrome. | | MRI before fasciotomy | Imaging delays definitive treatment. Muscle viability is already compromised at 4 hours with critical pressure differential. Every minute increases necrosis. | **Clinical Pearl:** Rhabdomyolysis (myoglobinuria, hyperkalemia, AKI) is a **consequence** of compartment syndrome, not the primary problem. Fasciotomy prevents rhabdomyolysis by restoring tissue perfusion. Mannitol and IV fluids are **adjunctive** measures after fasciotomy, not alternatives to it. ## Time-Sensitive Tissue Damage **Key Point:** Irreversible muscle necrosis begins at 6–8 hours post-injury. This patient is at 4 hours — still within the window for salvage. Fasciotomy now prevents permanent disability; delay results in: - Muscle necrosis and fibrosis - Rhabdomyolysis and acute kidney injury - Volkmann's contracture - Amputation [cite:Campbell's Operative Orthopaedics 13e Ch 56; Rockwood & Green's Fractures in Adults 9e Ch 1] 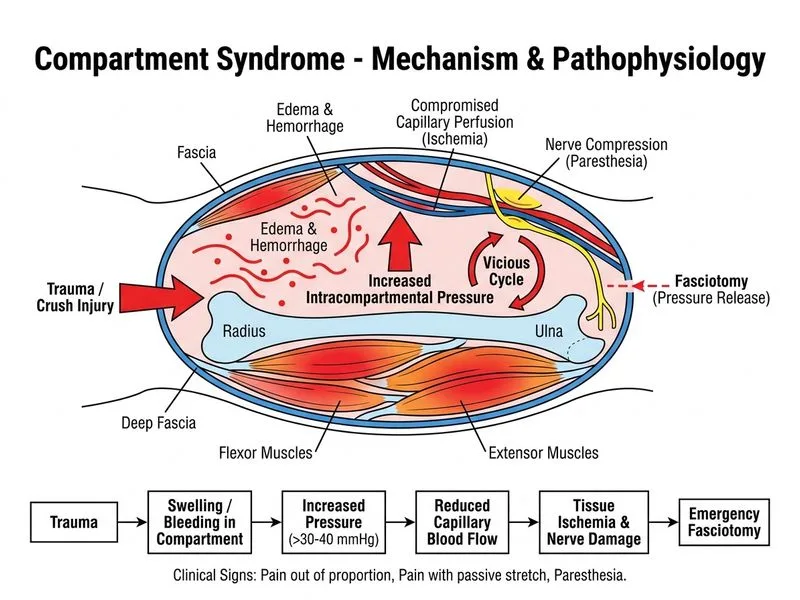
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.