## Critical Compartment Pressure Threshold **Key Point:** The critical threshold for compartment syndrome diagnosis and intervention is a compartment pressure of **30 mmHg or within 30 mmHg of diastolic blood pressure**, whichever is lower. However, the most commonly cited absolute threshold for tissue ischemia is **45 mmHg**. ### Pressure Physiology Compartment syndrome develops when increased pressure within a fascial compartment exceeds capillary perfusion pressure, leading to: - Microvascular collapse - Tissue hypoxia - Cell death and fibrosis ### Clinical Decision-Making | Pressure Level | Clinical Significance | |---|---| | < 20 mmHg | Normal compartment pressure | | 20–30 mmHg | Monitor closely; consider if symptomatic | | 30 mmHg (or within 30 mmHg of diastolic BP) | Threshold for fasciotomy consideration | | **45 mmHg** | **Absolute threshold for tissue ischemia** | | > 60 mmHg | Severe compartment syndrome; urgent fasciotomy | **High-Yield:** The "30 mmHg rule" (or within 30 mmHg of diastolic pressure) is the most practical threshold used in clinical practice. A pressure of **45 mmHg** is the absolute ischemic threshold above which irreversible tissue damage occurs. **Clinical Pearl:** In a hypotensive patient (e.g., diastolic BP 50 mmHg), fasciotomy may be indicated at a compartment pressure of only 20 mmHg (50 − 30 = 20). This is why relative pressure (delta P) is as important as absolute pressure. **Warning:** Waiting for compartment pressure to reach 60 mmHg before intervening risks irreversible muscle necrosis and Volkmann's contracture. Early fasciotomy (within 6–8 hours of symptom onset) is crucial. 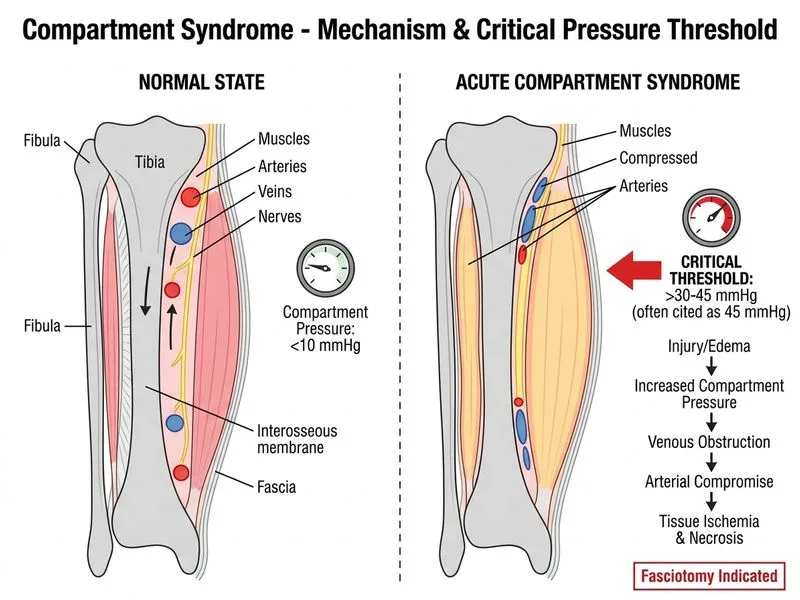
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.